EPISODE 449
Emma | Postpartum – bicornuate uterus, placenta previa, placenta accreta, hysterectomy

“We conceived pretty quickly with our firstborn, Ivy, and it was a really smooth pregnancy up until 20 weeks. That was when they discovered I have a bicornuate uterus (a heart-shaped uterus) and it can restrict the baby’s growth. From then on I had scans and checks every week to monitor her blood flow through the umbilical cord and her growth. She was also breech and positioned in the right half of the uterus so she wasn’t going to budge. I wish I had looked into breech vaginal birth but I didn’t know that I could seek a second opinion at that stage and I definitely have continuity of care – I was just seeing a different obstetrician at every appointment and none of them knew me. My caesarean was planned for 36 weeks and it all went like clockwork. Ivy was 2.35kg and she went to special care because she was cold and couldn’t regulate her temperature so she spent some time in the humidicrib.
“I breastfed Ivy till she was three. After that I really felt Arnold’s presence which is a bit spiritual but also undeniable so when I was ready, I conceived straight away. I was really hoping for a VBAC and, ideally a homebirth so I hired a private midwife. I’d done so many scans in Ivy’s pregnancy which was emotionally draining and stressful so I opted to only do the 20 weeks morphology scan. The baby was looking great but the placenta was over the cervix and growing over the scar which I immediately knew would likely be another planned caesarean. I knew that the placenta could move but I was still hopeful.
“My midwife explained that I had major placenta previa and that I had placenta accreta which is a placental disorder; instead of growing on the lining of the uterus, it starts to invade the uterus and grow into the muscle layer. There are levels of severity and sometimes it can grow right through the uterus and onto the bladder. Risk factors are IVF, advanced maternal age, lots of D+Cs and over 3-5 caesareans. Perhaps the shape of my uterus, my previous caesarean and where the embryo implanted contributed. It meant my pregnancy was instantly high risk so when this happens, it means it’s almost impossible to remove the placenta from the uterus. I knew I would need a planned caesarean between 35-36 weeks and if they couldn’t remove the placenta, I would need a hysterectomy at the age of 35. There was also a chance of dying, considering the significant blood loss.
“I could no longer have my care from my private midwife so I needed to transfer to the hospital and I was processing it all…all I really wanted was to experience labour. I saw the head of maternal and foetal medicine at The Mercy and he was incredibly empathetic. I really advocated for myself, I told him exactly what I did and didn’t want and I wanted to control the controllables. I was also grieving the loss of my menstrual cycle…I still am.
“I really wanted the chance to be awake to meet Arnold but generally women with placenta accreta will have a general anaesthetic. I said to my obstetrician: ‘If I’m going to die on this operating table, I want the chance to meet my son’ and he understood. He didn’t agree with it but we came to the compromise that I would have the spinal block and he would open me up to see the severity of the accreta. It was very scary.
“I had a bleed at 34 weeks which was resolved but at 35+5 I had a bigger bleed so I went straight to emergency. I wasn’t happy with the care so I discharged myself and the bleeding had stopped. The next day I spent time with a friend and I went to bed that night and had a feeling that I would bleed again. At 1am I went to the toilet and had a huge bleed so I went straight to the hospital. I had a huge bleed when I was there and at that point I just surrendered…it was up to Arnold to choose his birthday. I was 36 weeks at that point.
“I just kept saying to the team in the operating theatre: ‘please do everything you can so I don’t need a hysterectomy!’ They allowed me to be awake but I could feel the incision – not the pain but the sensation – so they put me under then and there. Apparently my obstetrician said he took one look at the uterus and could see the accreta so he went out to tell my husband that he’d need to do the hysterectomy. They did a vertical incision and cut through the placenta to get to Arnold and they delivered him really quickly. The placenta half detached from the wall of the uterus which meant the uterus didn’t contract down so I lost 4 litres of blood on the operating table. It was a controlled environment, they were prepared, they called a code white which means that they need many units of blood. I was under for three hours all up and during that time Arnold was in NICU.
“I woke up in recovery and I was in a lot of pain. I was asking for pain relief but they couldn’t give me anymore because I kept passing out. The obstetrician came in to tell me I’d had the hysterectomy but I just had to deal with the pain in that moment, the emotions came later. I went straight to the high-dependency ward and my nurse got my pain under control there. They didn’t take my ovaries, tubes or cervix which meant I didn’t go through menopause and my pelvic floor will still be intact.
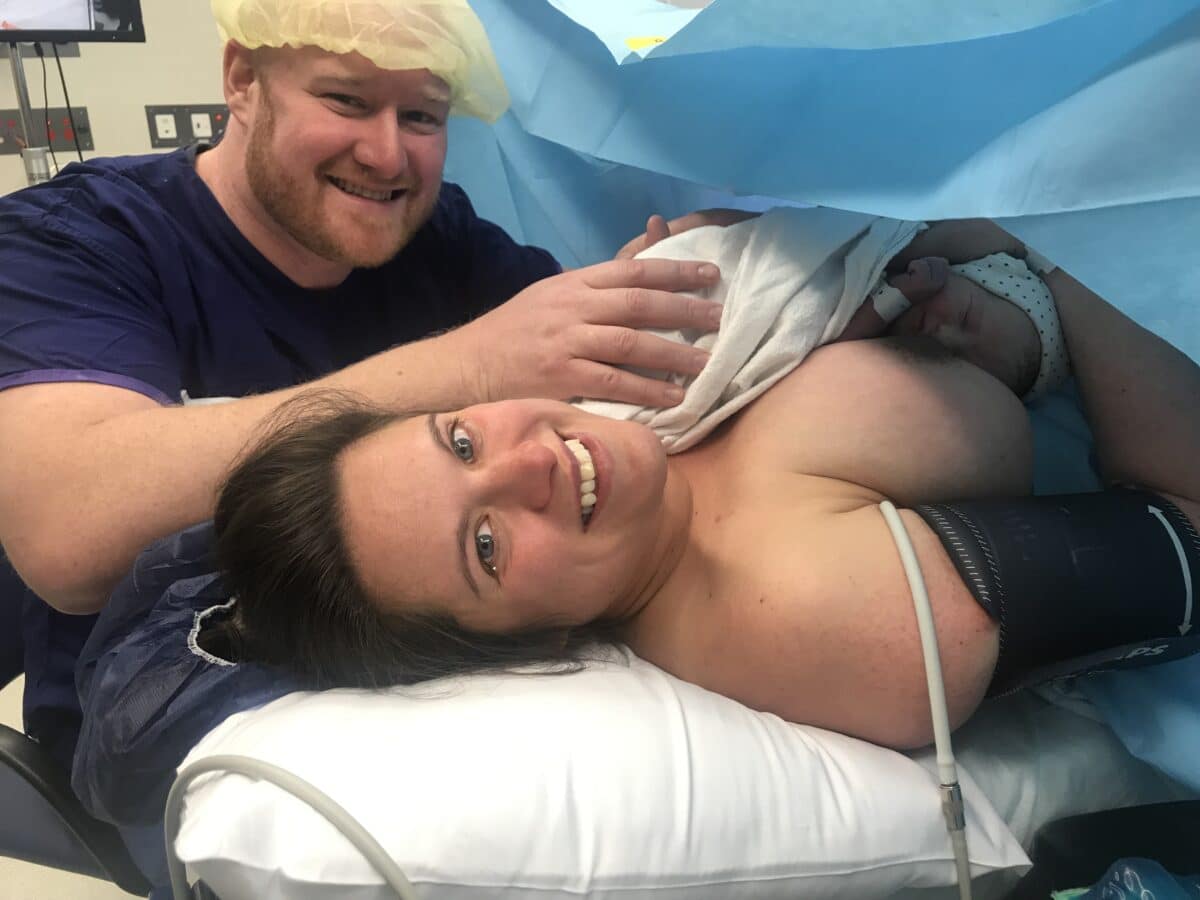
“They wheeled me down to the nursery the next day. My husband took a photo of me holding Arnold and you can see the joy and the grief; it was so strange to hold those two emotions at the same time. I was moved to the maternity ward and I advocated for myself to have a private room because the emotions were starting to hit me and I needed the safe space to wail and process. I was discharged within a few days and I had ‘hospital in the home’ (HITH) care from the midwives which was really, really helpful. Being through such a traumatic experience meant that I was more anxious so it was good to have reassurance from them. Andrew had five weeks off work and I was on bedrest for six weeks because I was still in a lot of pain and there was a lot of recovery needed.
“Something that’s helped me process my hysterectomy is burying both my uterus and my placenta. I spoke to one of the beautiful pastoral nurses at the hospital and told her that it felt really important to me to have them back. She advocated for me and the hospital stored them and returned them to me. It was an amazing experience to have them returned to me; it was like I felt whole again. I buried them, I wrote my uterus a letter thanking it for my two babies and since then I’ve felt so much better, it was like another layer of healing.”



Topics Discussed
Bicornuate uterus, hysterectomy, placenta accreta, Placenta previa, Planned caesarean, Two Babies
Episode Sponsor
Today’s episode of the show is brought to you by my online childbirth education course, The Birth Class.
What makes The Birth Class so unique?
Well, instead of learning from one person with one perspective, we’ve gathered nine perinatal health specialists to take you through everything you need to know about labor and birth.
Realistic information is key to thorough preparation.
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






