Home » Postpartum » Caesarean Birth Recovery
Caesarean Birth Recovery

If you’re recovering from a caesarean birth (c-section) it’s helpful to remember that your body needs to heal after major abdominal surgery. Caesarean births are common (roughly one in three in Australia) but significant surgery requires adequate recovery time. Here's what you can expect in your caesarean recovery.
Granted, it’s not easy to recover from a caesarean and take care of your newborn; lifting, twisting and feeding can be awkward and painful. The best advice we can give you is take it slow; you need to prioritise rest for the first few weeks, at least. Your body has worked so hard to bring your baby into the world and it continues to do all the vital work of repairing and healing so you can move confidently into parenthood. If you’re unsure about what will happen immediately after your baby is born, here are six quick facts about the hours after a caesarean birth.
Caesarean Birth Recovery
Everyone’s birth experience is different and the same goes for recovery. Generally we’ve been told that six weeks is the end goal for recovery but this isn’t quite true. Yes, by six weeks you’ll generally feel much stronger but your body still has months and years of healing ahead. A caesarean requires the cutting and stitching of seven layers of fat and connective tissue which can take up to two years to completely heal. There is no bouncing back to before; the only way is forwards, starting with small steps and lots of rest.
C-Section Recovery Day Week 1
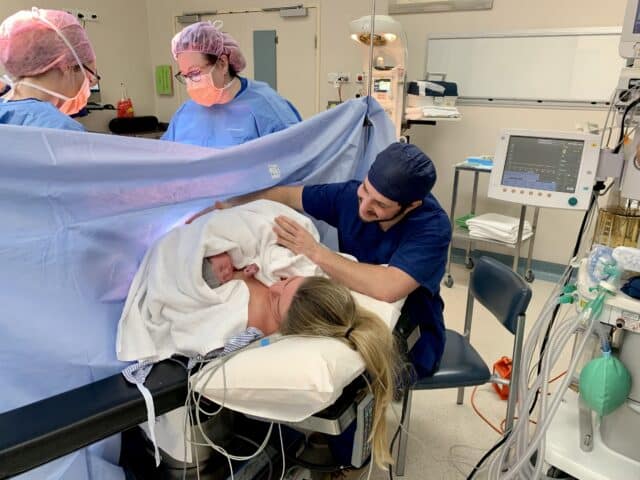
After birth you’ll be transferred to the recovery ward where a midwife will monitor you and, depending on hospital policy, you’ll be with your baby and hopefully practising skin-to-skin. If you plan to breastfeed, your midwife will help you initiate your first breastfeed. If everything is okay, you’ll be wheeled to the postnatal (maternity) ward after an hour. Your epidural will still be in (as will your catheter) so you won’t be able to get out of bed till the next day (one day after surgery). You can expect a midwife to give you a gentle sponge bath to freshen you up after surgery. You won’t be in any pain as the epidural will still be numbing you from the mid-section down.
Day 1
Your epidural will be removed and you’ll be given oral pain medication. Your urinary catheter will also be taken out and you’ll be assisted to the shower. It’s so important to get the body moving because moving encourages healing, relieves fluid buildup (particularly in your legs) and helps shift trapped gas which can be a painful common side-effect after surgery. You’ll need to wear maternity pads as you’ll bleed for up to six weeks after a caesarean
Day 2
You’ll be encouraged to walk around your room to assist with circulation and recovery. When you move from lying to sitting, do so slowly and with support. You’ll have waterproof bandages over your stitches but do your best not to get the area wet. Pain medication can make you constipated so you may be given stool softeners to assist with opening your bowels.
Day 3
Your pain should be under control and if you feel confident, it’s a good idea to walk around the ward. Research shows that recovery shorts or a belly binder can assist with healing by holding your core which ultimately gives you extra confidence when moving.
Day 4
If you don’t have any postoperative complications, you’ll generally be discharged on day four or five, depending on your hospital policy and whether you choose public or private care. Before you go home you can expect your obstetrician to check your wound and tell you how to care for it. They’ll also highlight the importance of checking it each day for signs of infection.
Signs of C-Section Infection
If you have any of the following symptoms, you’ll be advised to contact your care provider without delay:
- Redness or swelling around the incision
- Fluid and/or bleeding from the incision
- Increasing wound pain or pain that isn’t getting better
- A strong, unpleasant smell at the wound site
- Fever
- Increased abdominal pain
- Chills, fatigue, body-ache and flu-like symptoms
- Foul smelling vaginal discharge
Exercise after a C-Section
Movement gets easier every day but you should still prioritise rest (no walks or exercise for a few weeks yet). You’ll be advised to avoid driving, climbing stairs and lifting anything heavier than your baby. It’s good to remember that:
- Your uterus is still contracting back to its original size
- Horizontal rest is the best way to heal your wound as there’s no pressure (gravity) on it or your pelvic floor (which connects with your abdominal muscles)
- Recovery shorts or a belly band encourages the abdominal muscles to come together, assists with good posture and pelvic floor awareness
- Gentle pelvic floor and abdominal exercises in the first few days after birth can greatly assist healing because you’re encouraging blood flow and activating muscles that need strengthening. Continue doing them every day.
- If you feel like you need some fresh air and movement, a gentle walk may be okay but just remember that you’ll get sore and tired easily and you can expect an increase in your blood loss.
- You won’t be advised to return to exercise until you’ve seen your GP or OB at six weeks. It’s also advisable to see a pelvic floor physiotherapist before you return to high-intensity workouts as your pelvic floor is still recovering from the weight and hormones of pregnancy.
- Your pelvic floor can also be affected by a caesarean because the abdominal muscles are lifted in the stitching process which may cause a tight (hypertonic) pelvic floor.
Categories
Related Products
-
The Caesarean Birth Class
4 reviews$198.00The empowering online childbirth education program that will help you confidently prepare for birth.
Get your copy of our Perineal Massage Guide in your inbox
Keep Reading
We think you might enjoy these articles

The First Postpartum Poo: How to Protect Your Pelvic Floor, Perineum and Stitches After Birth

The Top 5 Vaginal Birth Recovery Products Every New Mum Needs

Breastfeeding: What to Expect in the First 72 Hours

How to Plan for Postpartum (and Why You Really Should)

Cracked Nipples: Causes, Treatment and Prevention

Caesarean Birth Recovery
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us