Postpartum Get to know your pelvic floor
Get to know your pelvic floor

You may not have thought much about your perineum or pelvic floor before you conceived but now that you’re pregnant (or in postpartum) it may be demanding your attention.
Here are five things you should know about your postpartum pelvic floor:
What is the pelvic floor?
The pelvic floor muscles stretch like a hammock from the pubic bone (at the front) to the coccyx or tailbone (at the back) and from side to side. They support the pelvic organs (the bladder, bowel and uterus), and the urethra, vagina and rectum pass through them. The front group of pelvic floor muscles work to prevent unintentional urination, while the rear group does the same for bowel motions, and together they play an important role in sexual function and enjoyment.
What happens to the pelvic floor in pregnancy?
In pregnancy, thanks to weight gain and the weight of your baby, your placenta and amniotic fluid, your pelvic floor is under more pressure. Subsequently, the muscles and tissues stretch and have a tendency to weaken. Pregnancy hormones also contribute to this; they allow your muscles to soften and stretch more easily in preparation for birth.
What can we expect from the pelvic floor after birth?
The pelvic floor muscles work tirelessly in labour and birth, hence it takes time for them to recover in postpartum. Age plays a significant role in pelvic floor recovery; if you’re 35 or older, your muscles won’t bounce back as well as a younger mother (this is relevant to everyone, regardless of how you birthed your baby). However, spontaneous recovery does happen, even when prolapse is diagnosed in early postpartum.
We encourage you to listen to Sophie’s interview with renowned women’s health physiotherapist, Sue Croft in episode 380. Sue shares everything you need to know about your pelvic floor in pregnancy and postpartum, including the management of prolapse.

Head to boody.com.au/australianbirthstories – you’ll find everything you need for this time in your life and beyond plus a code to enjoy 15% off everything in the edit.
What is a prolapse?
If you experience a heavy or dragging sensation in your pelvis, this may be a symptom of prolapse. The word prolapse means ‘to fall out of place’ and when we are discussing pelvic floor prolapse, it means one of the pelvic organs (Pelvic Organ Prolapse – POP) sags or may bulge into the vagina. This occurs when the pelvic floor muscles, ligaments and tissues that work to support the organs are torn or stretched, and therefore can’t hold the organs in place.
How can a woman’s healthy physio benefit postpartum recovery?
All bodies are different and likewise, all pelvic floors are different. When you leave hospital or see your GP or obstetrician at your 6-week checkup, they may mention pelvic floor exercises or ‘kegels’. Unfortunately being guided by exercises in a pamphlet isn’t always helpful (sometimes undirected pelvic floor exercises can do more harm than good). A women’s health physio is incredibly beneficial to your postpartum recovery and long-term pelvic floor health; they will explain your pelvic floor to you, highlight any areas of concern and educate you about correct exercise.
If you want to know more, we encourage you to tune into episode 380 of the podcast, where Sophie interviews women’s health physio, Sue Croft about the pelvic floor in pregnancy and postpartum.
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Get your copy of our Perineal Massage Guide in your inbox
Keep Reading
We think you might enjoy these articles

The Top 5 Vaginal Birth Recovery Products Every New Mum Needs

Breastfeeding: What to Expect in the First 72 Hours

How to Plan for Postpartum (and Why You Really Should)

Cracked Nipples: Causes, Treatment and Prevention

Caesarean Birth Recovery
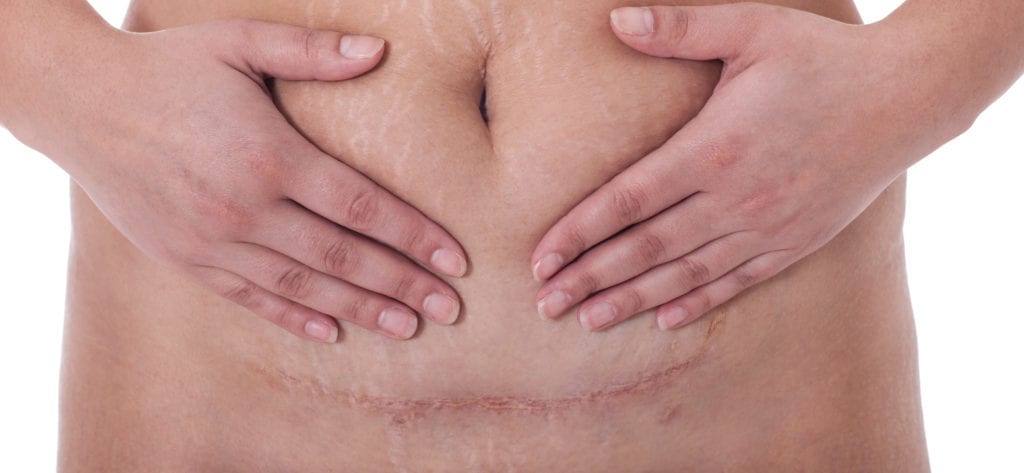
What is a C-Section Shelf?
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us


