EPISODE 425
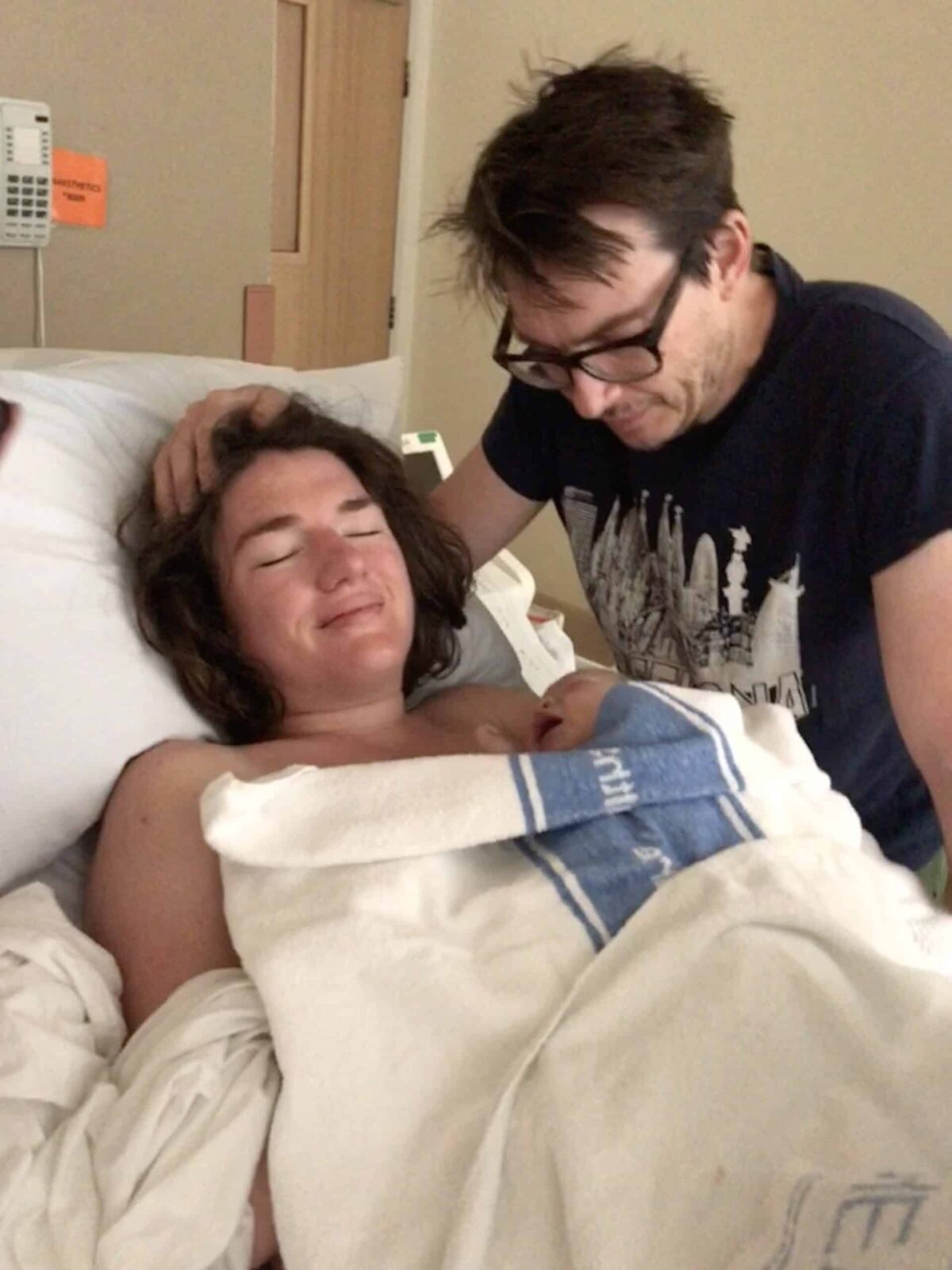
Bridie
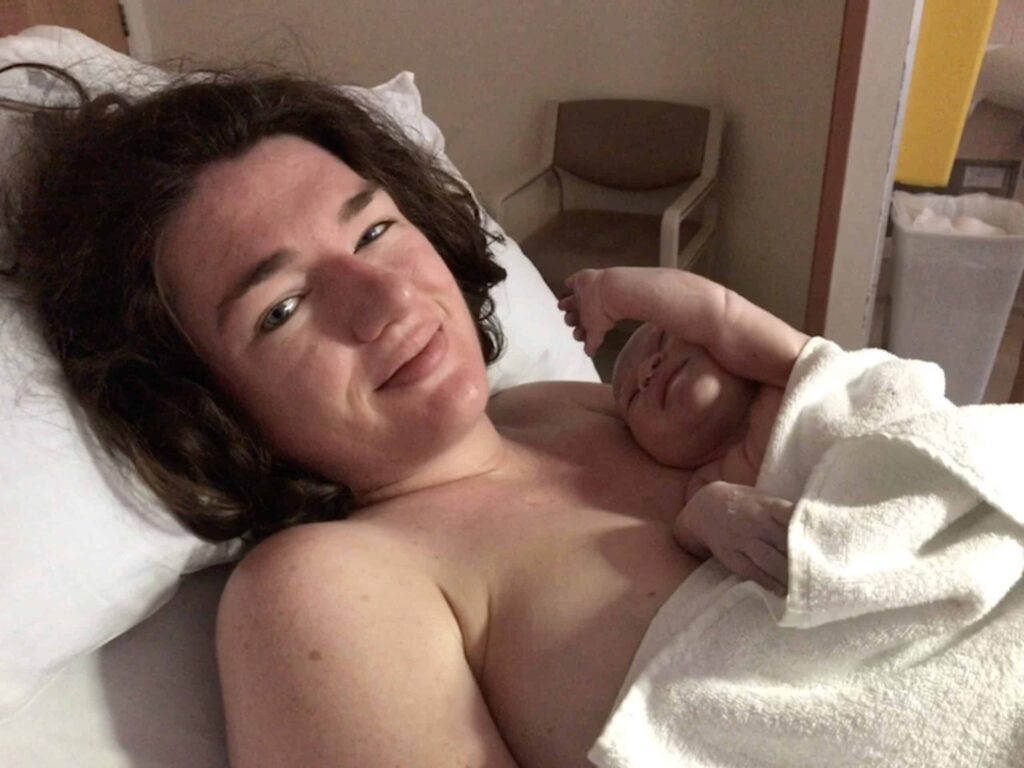
“My mother is a midwife and she’s one of ten, my dad is one of six, and they had four children so I was always hyper-aware of our family’s fertility. I was really conscious of contraception and quite strict with it. I suppose like most girls and women I was quite scared of getting pregnant. In my early twenties I was diagnosed with endometriosis so while I was thinking I could conceive at the drop of a hat, I was also concerned that I would have issues. I feel like I went into pregnancy with a lot of knowledge.
“I went off contraception and we conceived within four months. My mum never told me this but she was concerned about my ability to conceive after my endo diagnosis so she was absolutely over the moon when I told her. It was a really exciting time telling everyone and my partner and I were thrilled. I even took some friends out to dinner to tell them; it was a really special announcement and I kept a diary of how everyone reacted.
“My mum would always want me to give birth in a hospital; she’s been a midwife for 40 years so she’s witnessed a lot of both happy and devastating moments. I wanted her to be at the birth but she never forced anything on me. She was really happy for me to make informed decisions for myself. Her motto is: a natural birth is a healthy mum and a healthy baby so she never drilled into us the fact that there was a better way to birth. I went into a continuity of care model at St George Hospital and I loved the program and loved getting to know my midwife.
“The fatigue hit me; I wasn’t prepared for the physicality of pregnancy in all the trimesters and how difficult I found it at times. I feel like you should tell people at work in the first trimester because it’s so hard and back then, no one worked from home so I was commuting five days a week.
“Mum encouraged me to go to a birth class and it was at the hospital; I walked out halfway through because it was very alarmist, I felt like they were trying to scare us and I also found it very ideological about the use of pain relief and caesareans. But I was so lucky because anytime I had a question, I just called mum.
“I really enjoyed a break from my period and endo pain. When I was twenty I got a labial hematoma – which is where a blood vessel burst and it was swelling over weeks and I was in a lot of pain. I ended up having surgery for it which is unusual and it kept bleeding and swelling and I had stitches…and I ended up going into surgery for a second time in a week. There was a bed shortage and I ended up going on the postnatal ward and I was crying and telling the midwife that I couldn’t go through that pain again and she said labour was nothing like that.
“The second half of my pregnancy was so painful; I didn’t know pregnancy could be so painful. I had symphysis pubis dysfunction – an unstable pubis – and I couldn’t walk or sleep. It’s when your ligaments overstretched and the baby’s movements put pressure on them. Mum came to stay because she was concerned about my mental wellbeing and my midwife decided to schedule an induction for 39 weeks because they thought if I went any further I’d be too exhausted to labour.
“I was showing signs of pre-labour; I was getting the cramping, I lost my mucous plug. I had always believed that my due date was the end of November based on my cycle but the scans made my EDD mid-December which is a big difference. My mum gave me a vaginal examination so it did get quite intimate towards the end and she was so emotional and excited that when she ripped the glove off she just sprayed my juices all over me.
“I went into hospital at 4pm and they inserted the gel and it worked straight away. My brother is a nurse and he worked in the same hospital so he came down to see me and then he left, mum left and they sent Matt home at 8pm and I was left alone, the contractions getting more intense and closer together. I don’t think I’ve ever felt more alone in my life. There was a shift change and a senior midwife could see I was in labour and she called Matt and got him straight back in the hospital.
“At 1am I had morphine which didn’t touch the sides and at 2am my midwife ruptured my membranes and that’s when we called mum back in. My baby was posterior as well so I had consistent pain, even though it did go up and down. At 4am I opted for an epidural and I made that decision; I didn’t feel the need to check in with mum because I knew she was there to support me. I slept for two hours after that even though the epidural wasn’t heavy at all; I actually felt like I could stand up if I wanted to.
“I felt completely and utterly safe; I knew mum would spot something immediately, she was on top of it. I didn’t need to worry about advocating for myself, I just needed to get the baby out.
“At about 6:30 my midwife turned off the epidural and by 8:45am I was pushing. Matt was next to me and I didn’t let him go. I was pushing and I was playing mantras in my head and one of them was: this is just going to be a story one day. I pushed for an hour-and-a-half – the longest hour-and-a-half of my life and the hardest thing I’ve ever done. At one point I gave up – common, obviously. My mum cried and turned away from me and she said she just wished she could have taken the pain away from me.
“My midwife was quite firm with me, she put my foot on her shoulder and she snapped me out of it. My mum caught him and I was so exhausted at this point that I lay on the bed, closed my eyes and tried to go to sleep. I was so shattered. The midwife put him on my chest and that’s the cliche of not getting to do what I wanted, I had someone else to look after now. I got the instant rush of love and connection and awe. Mum left soon after so Matt and I could be together with our baby.
“I stayed overnight and the next day I told mum that I thought something had gone wrong with the epidural because I was sore from head to toe; my muscles were aching. And she just looked at me and told me it wasn’t the epidural, it was the marathon of labour. Mum helped me establish breastfeeding, showed us how to bath the baby and then she left after a few days.
“My recovery was a bit difficult so on night three, mum took Hamish for six hours because she knew how much I needed the sleep. There was no anxiety or questioning because I had the consistency of trusted care.
“I’m one of four and I’m so close to my siblings so I always envisioned that I’d have more than one baby. However, recovering from my birth was really difficult and I was more shaken by it than I thought I would be; I thought about it every day for months. I thought I’d start trying again when Hamish was one but I was not physically, emotionally or psychologically ready. When Hamish was about 19 months old I felt ready and we fell pregnant the first month we tried.
“My pubis started earlier and I remember just sobbing in bed at 20 weeks not knowing how I was going to cope. Then I went psycho journalist-mode to find the best pelvic health physio in Sydney and she had me pain-free for three weeks at a time. She used internal physio and strapping and she was phenomenal. My baby was due in June 2020 so there was a lot of external anxiety, my work went bonkers and my brother was working in ICU in Sydney so he was treating some of the first Covid patients. I was consuming all the stories of women birthing in New York alone.
“Halfway through my pregnancy I started working from home and physically I felt so much better because I wasn’t commuting. It made me think that maternity leave should start in the third trimester. I was at the same hospital but I didn’t want to stay in the hospital, I didn’t want to be alone with my baby overnight, I really wanted mum there but I was only allowed one support person. Matt was my number one birth partner but we came to an agreement that if I had a complication with my pregnancy, mum would be with me in labour but if it continued to be a straightforward pregnancy, Matt would be with me. I ended up writing to the head of the health district laying out why the policy should be changed around birth partners, laying out the risks and all the evidence for having proper support. I wanted the whole policy change but what they gave me was an exception to have my mum and Matt with me.
“Mum and dad came down to help us move house at 39+2 weeks and the night before my due date my waters broke at home. I went into hospital and they said everything looked fine and they told me to come back the next day for an induction if labour hadn’t started. I slept at home that night, went back to hospital, had the syntocinon drip and labour really kicked off by about 1pm. The gas and air really helped in this labour; I got into a zone with it and I was riding each contraction. Within an hour I felt every contraction on top of me, it was like being dumped by waves. I told mum I wanted an epidural and she said: let’s see what the midwife says.
The midwife examined me and told me I could have an epidural but to do so, I needed to get out of the bath, lie on the bed and wait for the anaesthetists and by the time I’d done all that, I could just have my baby. So of course I agreed.
“I pushed for 25 minutes and birthed him in the water. It was amazing and I feel so lucky that it happened for me. I pushed and could see his head between my legs and he had a full head of black hair. I breathed his body out and we watched him floating in the water; I was in awe, mum was in tears and Matt was internally freaking out because he didn’t understand that babies born in water didn’t take a breath till you lifted them out. Mum lifted Cormac out of the water and put him on me. I felt amazing but I was also spent. I didn’t tear and I think the perineal massage and water birth helped. I went home a few hours later and I was stunned at how different it was and how strong I felt.”
You can check out Bridie’s podcast Cool Story here.

Topics Discussed
Endometriosis, Epidural, Induction, MGP, Posterior labour, pubis symphysis dysfunction, Two births, Water Birth
Episode Sponsor
If you’re pregnant, we encourage you to start thinking about your birth recovery now. You need more support in the fourth trimester (the 12 weeks after birth) than you do in pregnancy which can be surprising to many new mothers. It’s for this reason that Bare Mum began and now they offer a beautiful collection of practical and supportive products to assist your postpartum healing.
All new mums need lower back, abdominal and pelvic floor support after birth. Bare Mum’s Postpartum Briefs gently hold you in the first days and weeks, helping you feel confident. Endorsed by the Australian College of Midwives, they offer a unique pocket design so you can insert a warm or cold pack to offer soothing relief and assist with caesarean wound or perineal healing.
Ideal for caesarean and vaginal birth recovery, Bare Mum Postpartum Briefs are soft, stretchy, and supportive, offering you essential post-birth care. They’re a must-have for your hospital bag.
Bare Mum is offering you 15% off storewide with the discount code ABS15
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






