EPISODE 424
Bryley | Postpartum – hydrops fetalis, amniocentesis, thoracentesis
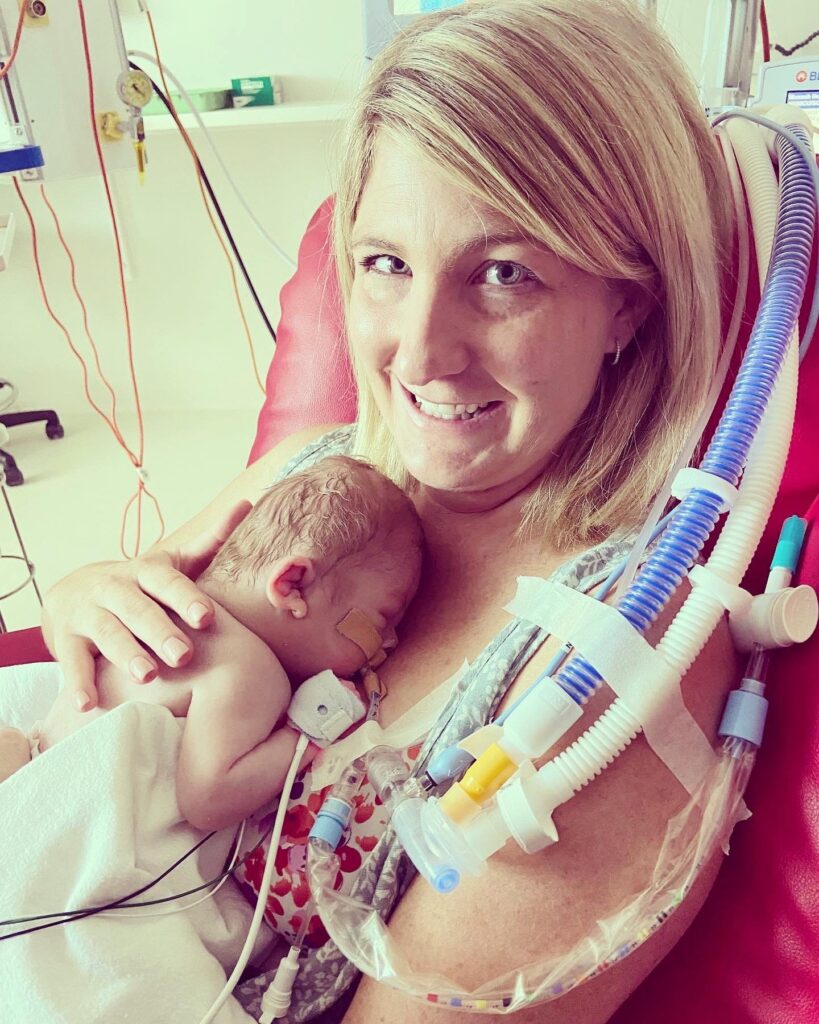
In today’s episode Bryley shares her challenging pregnancy experience and five-month NICU journey with baby Mason who was diagnosed with hydrops at 20 weeks. For the remainder of her pregnancy Bryley required frequent ultrasounds and procedures on her baby while in utero while navigating the challenge of many unknowns. Mason spent 148 days in the NICU and towards the end, Bryley had to advocate for his discharge because her family was at breaking point.
“Mason’s pregnancy was planned but there was a big gap between our girls and him; we’d sold all our baby items, we could go out to dinner without being interrupted … .but we’d done it before so we knew we could do it again. I decided to go with a private obstetrician like I had with the girls but in the end, it was all taken out of our hands.
“I was a lot sicker in my first trimester and the 12 weeks scan was fine although I had a two-vessel umbilical cord but they weren’t concerned by it. At my 20 week scan, which was the first one my husband could attend because of covid, the sonographer left the room and came back with a doctor and that’s when we knew there was something wrong. We were told that there was fluid on Mason’s lungs and they needed us to go to the city to see the senior doctor. I presumed I’d have to make an appointment but they told us we had to go straight there and see the doctor immediately and that’s when we knew it was serious.
“They did another ultrasound and the senior doctor explained the conditions that can be associated with fluid on the lungs and all the possibilities were really confronting. He offered us an amniocentesis for genetic testing and I had to go for a blood test and we agreed that was the best course of action. We did the amniocentesis that day and straight after we did a session with a genetic counsellor who took us through the possibilities and informed us that it would take three weeks to get the results. One of the possibilities was hydrops fetalis which is very rare and only 20 percent of babies diagnosed with it actually survive the pregnancy and for those who are born, only 50 percent will survive so it was very confronting.
“I had to stop googling because nothing I was learning was positive. My obstetrician was in touch with me weekly and she did inform us that when we did get the results, I would be past the date where I could choose to terminate. In that case, if the genetic results did show a condition and we did want to terminate, it would have to go to an ethics board. I was absolutely floored that someone else could make a decision for me and my body and my baby; it seemed so inhumane. This is when it felt like we didn’t have any control over my life. We went back for a scan at 23 weeks and the fluid had spontaneously resolved and we thought it was a miracle. The genetic counsellor called me and she said the results were all clear.
“Three weeks later my obstetrician did a scan and she saw fluid on the lungs so from then on I had ultrasounds weekly. By 30 weeks there was oedema; fluid around his head, under his skin, in his lungs, and I was huge; it felt like my skin was going to rip apart. It was around this time that my obstetrician encouraged me to go to a high-risk OB – Ryan Hodges – at Monash and the foetal medicine team managed me and they were incredible.
“I went to the hospital that night for steroid injections because Mason could be born at any stage and then I had an ultrasound every second day. You’re thrust into this medical world and you’re trying to understand how DNA and genetics works and it was really overwhelming. At 32 weeks my OB suggested doing a procedure called a thoracentesis where they inserted needles into my womb and into Mason’s lungs to drain the fluid. They put five huge needles into my stomach and you could literally see Mason’s lungs expand as they drained the fluid. While they were there, they drained 2 litres of amniotic fluid from me and I instantly felt better. They were hoping that would buy us another two weeks. I went back the next day for monitoring and an ultrasound and as soon as the machine was on my stomach we could see that all the fluid was back, within 24 hours. It just felt so unfair. My OB wanted to do a scan the next day and amongst all of this it was my second daughter’s first day of school and I just wanted to be there for it, it was important. The doctors wanted me at the hospital at 9am and I just told them I couldn’t because I wanted to be there with Chloe; it was such a big milestone.
“The ultrasound wasn’t great; my OB suggested shunts to drain the fluid in utero or deliver. Another doctor called me and told me all the teams were organised for the birth at 5pm that night. I remember standing there and thinking about how crazy it was. The doctor called me back to see if I was okay and I explained that i hadn’t packed my bags and she said: just pack for yourself, you don’t need to pack anything for the baby. At the time I didn’t think much of it but she was telling me how sick my baby was. I understand the severity of it now.
“Looking back I was so naive; I had no idea how bad the odds were for him or how sick he was. I think this ignorance helped get me through the pregnancy. We went to pick the girls up from school, told them the baby was coming, and off we went to the hospital.
“The NICU consultant came to the birthing suite and explained that Mason wouldn’t be breathing at birth and would need to be resuscitated. There was a team of specialists looking after him and a team looking after me. They took me to theatre and I got a spinal block and they decided to do an extra thoracentesis before Mason was born so we had the fetal medicine team in there too.
“They cut me open and I started screaming in pain because I was having cramps and the whole theatre went silent and my OB asked where my pain was and I explained it was cramping around my middle and he asked me if I’d had stomach trauma and he said my whole stomach was bleeding out. My whole stomach was covered in scar tissue, my placenta was stuck to my uterus and I was hysterical and just full of anxiety. The anaesthetist gave me fentanyl which did the job and they brought Mason out and he was just a floppy marshmallow and that’s when our next journey began. I was also haemorrhaging and my OB thought I’d started to develop mirror symptom which is where the mother mimics the baby’s systems. They kept Mason’s cord connected and they worked on him on my legs and then he was intubated and he had drains coming out of his lungs. Brad went with Mason to NICU and I went back to the ward and the nurse came in in the early hours and told me the doctors were trying to ring me to ask for approval for a blood transfusion. From that moment on, for the next five months, my phone was never on silent and it was never out of my sight because I was so scared that I would miss another call.
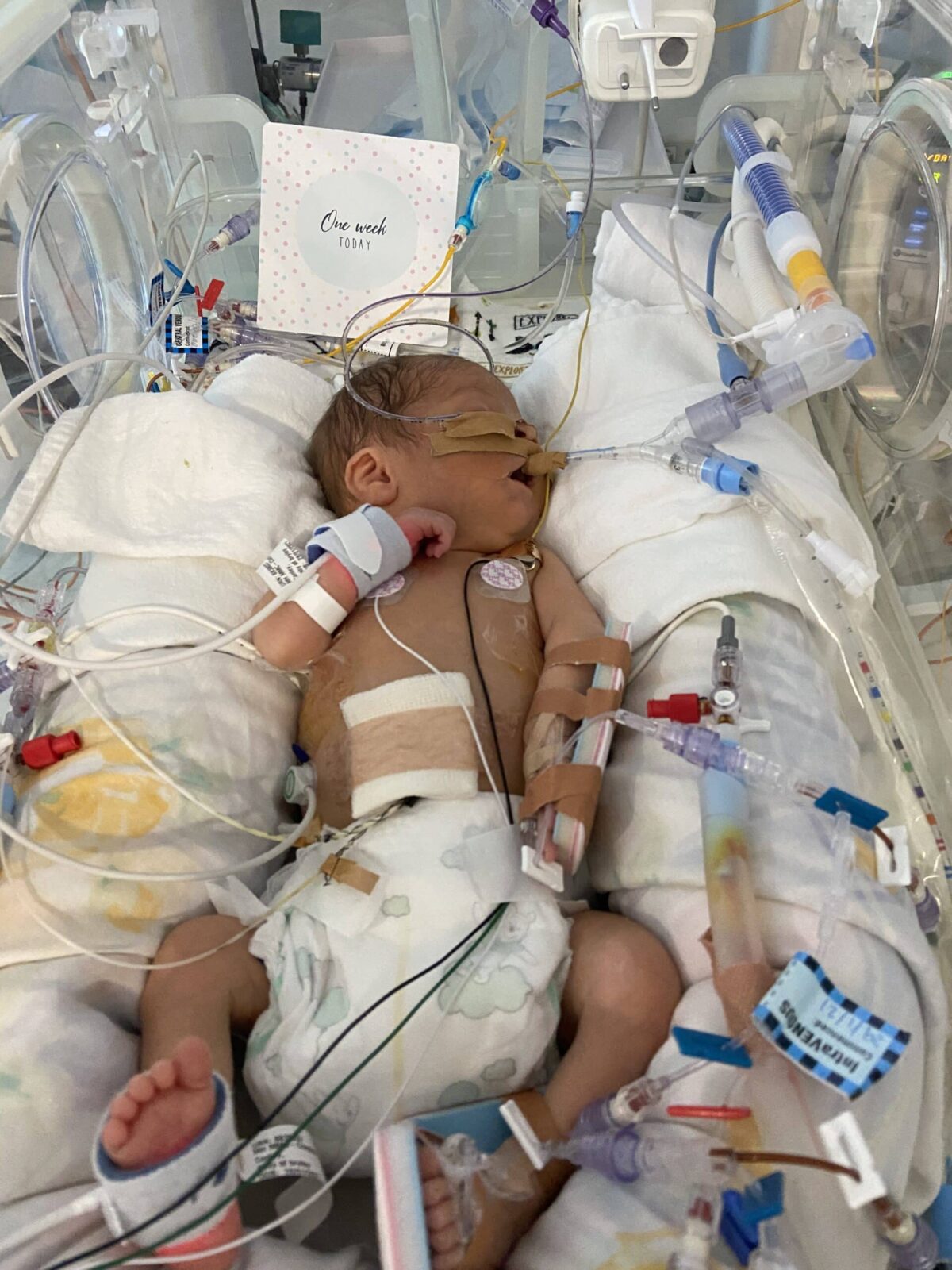
“He was in NICU for 148 days. The day after birth I couldn’t move, I was in so much pain, so the NICU doctor came to me. I still hadn’t been to see Mason at this stage. She told me he was in the highest level of breathing support possible and he was the sickest baby in the NICU. I remember I didn’t even really understand. They took me down in a wheelchair and he was in the 4-bed ward so he had his own nurse 24/7. There was a wall of machines and it was quite noisy and I remember vomiting because I felt so sick and overwhelmed. It became this whirlwind and we were thrust into this medical world of new terminology and big decisions but also not having much control over decisions either because they were so medically complex.
“They told us he would be in NICU till his due date and then the conversation changed and they warned us he would be in there for a bit longer. A week after I took the girls to school and the phone rang and it was the doctor and he asked me to make my way into the hospital. Mason had a bowel perforation so he needed emergency surgery but he was too sick to move so the surgical team were bringing everything up and were going to operate on him in his cot. He was on life support, he’d had blood transfusions, I still hadn’t held him because he was just too sick.
“I held him for the first time at three weeks old and he was placed so carefully and I couldn’t move; it was so awkward, there was nothing natural about it.
“Mason was baffling the doctors, he was having scans on his brain and heart daily and I remember thinking; how can he heal and recover if he’s constantly having things done to him. He moved from being intubated to CPAP and then high-flow oxygen. He had a nasal-gastric feeding tube so I was expressing in the early weeks but it got too hard so he was on a special formula. They weren’t sure if he could suck on the bottle and breathe at the same time so we expected that when he was discharged he would have the feeding tube.
“It was a battle to get him to come home because hospital policy doesn’t usually let a baby come home on high flow and with a feeding tube. I learnt that I had to advocate for him and our family; we were breaking by that point. I was at the hospital during the day, I’d go home to be with the girls in the afternoon and evening and then Brad and I would return to hospital at night to be with Mason and we did that seven days a week. The doctors called a multidisciplinary team meeting and I had the support of the social worker and I felt so prepared and had such strength to fight for Mason and my family. I had a letter and I just begged them to work with me to get Mason home. I told them our family was breaking and I said: ‘this is your job and you go home every night but this is our life and we’re stuck in a hospital system.’ That was the turning point. We finally got agreement that if he could have three hours off high flow then he could go home so I spent the next few weeks getting to that three-hour mark. Brad and I had to do CPR training, learn how to administer his tube feeding and reinsert his tube and then the day came…
“We had a hospital in the home so we had a nurse come every day and it was so hard, the next phase of life, but we were together all under one roof. He came off oxygen and we eventually got him onto a bottle after weaning off the tube feeding. He has severe chronic lung disease and they can’t tell if it will improve as his lungs grow but he looks like a very normal two-year-old.
“I’ve received a lot of support throughout our journey but I do have PTSD after everything I went through and I see a psychologist and it really is so important for NICU mums to have that support around them. I did EMDR treatment and it’s so important for people to reach out for support after trauma; put your hand up, tell your mum, sister, friends that you’re really struggling and you need help. My EMDR treatment changed my whole experience and the way I recall my memories; it was transformational. The benefits were instant. I mapped all my traumatic experiences and did the therapy and later that day if I thought of those experiences I no longer had the same emotions that I had previously; the benefits were instantaneous. A year after Mason was born I couldn’t watch a birth on tv and I couldn’t handle seeing a photo of a mum holding her newborn on instagram because I didn’t hold Mason for three weeks so it was really triggering. I realised that I hadn’t processed the trauma of my pregnancy and postpartum and I didn’t want it to impact my life; I wanted to be happy for friends if they were having a baby.”


Topics Discussed
Amniocentesis, Caesarean birth, foetal medicine team, hydrops fetalis, NICU, thoracentesis
Episode Sponsor
Today’s episode is brought to you by Kin. Kin are giving you twelve dollars off their best-selling prenatal vitamin with the code ABSKIN12. Why twelve dollars? Because Kin’s prenatal vitamin is packed with 12 high-quality, bioavailable ingredients like Methylated Folate, Iron, Choline, Omega-3 DHA and more, in just the ideal amounts.
We know that pregnancy and birth can be full of unknowns so choose a prenatal like Kin’s that you can rely on. Not only will it help you to meet your nutritional needs when trying to fall pregnant but, it will also support your baby’s development through pregnancy too. It’s gentle on tummies and has a subtle vanilla taste that’s naturally delicious.
Head to Kin and use the code ABSKIN12 at the checkout for $12 off your prenatal vitamin today.
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






