EPISODE 355
Steph – cord prolapse, birth trauma

“Lachlan and I have been together since I was 13. We got a bit slack with contraception and I just felt that something wasn’t right so I did a test and there were two pink lines. I went to the shops and bought two more tests and both were positive.
“Both of us broke down; we weren’t prepared or ready for it. We’d had conversations in the past about what we’d do if I fell pregnant as a teenager so we just decided to sit on it and decide what to do. I’m a nurse and the hospital I work at is the only one that offers maternity services in the area and the day after I had to do training for pregnancy and birth issues including cord prolapse, postpartum haemorrhage….all I could think of was that if I went through with the pregnancy, all these things could happen to me. I made a doctor’s appointment that day and that was to get a blood test but also to talk through my options if we decided to go through with a termination.
“In the end we decided to embrace the pregnancy and I think that decision was made easier because we know so many people who have had fertility issues and here we were with this blessing that had just arrived in our lives.
“We’ve got a unique maternity system in the Riverland area of SA. There’s two birthing hospitals; one that does GP shared care whereas at Riverland General Hospital we do a combination of MGP and GP shared as well as obstetrician-led care. I was assigned my own midwife and every second appointment I saw an obstetrician. There was a lot of continuity of care which was amazing and the midwives see you for six weeks after birth, too.
“My first trimester was easier than my second. At twelve-and-a-half weeks I started vomiting and having headaches and because the hospital I worked at was also the only covid hospital, I was quite stressed. I took a few weeks off but then around that time I started to get pelvic girdle pain and got support garments from the local physio which definitely helped.
“Lachlan and I are over the top planners so we were really excited about having a baby but of course we still had some fear about the changes ahead. I had a birth plan figured out before I was pregnant and I learnt so much from listening to your podcast.
“At 38 weeks Lachlan started to feel unwell and the next day he got a positive covid test. A few days later I started to feel unwell so I got a PCR which was negative but a few days after that I got a positive RAT. My midwife advised me to rest and keep an eye on the baby’s movement and she told me the anaesthetist team would want to meet with me at 40 weeks to decide whether I was still safe to give birth at the local hospital. The anaesthetist told me that because I’d had covid, in the case that I would need a category 1 emergency caesarean and a general anaesthetist, I may have an asthma attack and I wouldn’t be safe under their care. He recommended I go to Adelaide and he wanted me to make a decision then and there. He was in this frame of mind because two days beforehand he had transferred a woman to Adelaide after this exact scenario had played out and she went straight to ICU.
“I was still low risk in pregnancy but I was a high-risk anaesthetic patient. Basically once you’ve had covid, for eight weeks afterwards, you’re at a risk of a bronchospasm, which meant I needed to be in a tertiary hospital. I had my last midwife appointment at the hospital and then I drove to Adelaide and stayed with my extended family.
“Once I got there I had a midwife appointment and an induction was scheduled for later that week. She told me to do everything I could to get labour to start naturally. When I went in for an induction they started with the cervidil gel to soften my cervix so the next morning they could break my waters. I had so much pressure in my back that I was rolling around on the bed and I just couldn’t get comfortable. I started timing my contractions and when the midwife asked if I wanted to have a vaginal examination I consented. She put her hand in and it was so painful that I asked her to stop and get away and she ignored me and pushed her hand in further. I felt so violated. Soon after my waters broke and I vomited over the bed at the same time.
“My midwife told me I needed to go to birth suite and she didn’t help me at all, she didn’t offer any support, it was like I was a hindrance. Lachlan finally arrived and I was just so relieved to have him there to support me. I was in the shower and a student midwife came in and it was so lovely to have someone caring for me. I kept saying I couldn’t do it anymore. The midwife moved me to the bed and I felt something slip out of me but I didn’t think anything of it and then the midwife looked down and told me she could see the cord. I knew what cord prolapse meant so I immediately put my head on the ground and my bum in the air because that’s the protocol. Twenty people came into the room and there was panic in their voices. I was on the bed and then a midwife introduced herself and told me she would be putting her hand in my vagina and when she did she said she could feel a hand and a foot.
“The obstetrician asked me for consent for a caesarean and I just said: do what you have to do to get the baby out of me. We rushed down to the theatre, they were running while I was on the bed and the midwife’s hand was still in me. Once in the theatre, I was having a cannula put in as well as all the monitors but the whole time there was someone holding my hand which meant so much to me. All I remember then is them putting the oxygen mask over me and everything went black.
“Mason was born at 4:49am. When I woke up in recovery they told me I had an emergency caesarean, they told me my baby was in NICU and he may have permanent brain damage. Lachlan came in and he was so frazzled and stressed. He told me the baby was a boy and he stayed with me so we could meet him together. My only concern at that moment was giving him a name, that’s all I cared about. While we were there a few of the birth team came to see us and explained that he was born with an APGAR of 1 which is terrible. They did five minutes of CPR and gave him one shot of adrenaline. They intubated him and rushed him up to NICU and everything was waiting to go up there because they knew I’d had a cord prolapse.
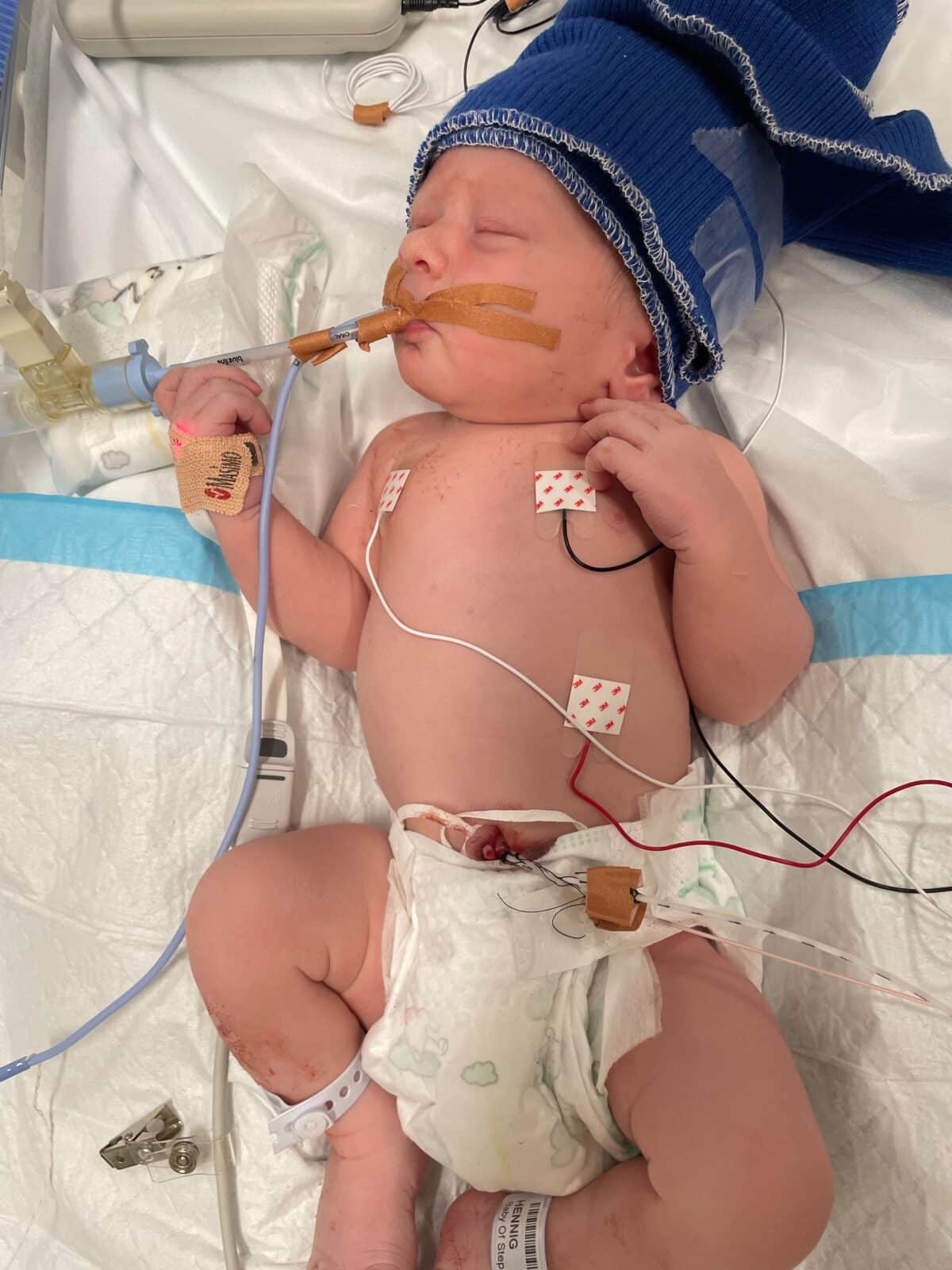
“The first photo of us seeing him was at 7:03am, which was two hours after birth. He was covered in tubes, including monitors for his brain activity. He had a tube down his throat and a few in his mouth to monitor his core temperature and CO2. The really hard thing was that I couldn’t hold him but I was able to put a hand on his chest. The NICU staff were absolutely amazing, they really supported us from the moment we got in there.
“Later that morning when I was on the postnatal ward so many of the people that were in theatre with me came and saw us to check on us. There was no counselling provided by the hospital but the staff who were there for the birth came to debrief and check on us regularly. We got an exception for Lachlan to stay in hospital with me which was amazing.
“I have healed really well and I think it’s because I could look after myself because Mason was so well cared for in the NICU. He’s done so well too; within 13 hours they took the intubation tube out and he was feeding within a few days. He did a lot better than what they first predicted. MRI and brain wave monitoring haven’t shown anything of concern. Once he was discharged at 10 days old we were told that he needs to see a team of people at every developmental step to ensure his development is on track and we’ll do that till he’s five.
“We were set up to fail at breastfeeding from the beginning; we had no skin on skin, I didn’t pump for the first twelve hours. I eventually started hand pumping that I would take to the NICU and I wanted to exclusively feed once we were home so I had to feed in NICU. So far, our breastfeeding journey has been wonderful, we’ve had no issues. On his last night in hospital we stayed in a room with a queen bed overnight so we did that and the next morning we packed up and drove three hours home.
“He’s such a happy and smiley boy, he’s just doing everything as expected. I hated my birth and I’m so sad that it was that way. I definitely have plans to do counselling and move through my fear of birth and my anxiety with Mason because I’m scared of him getting sick and I’m scared of him dying. There’s a lot of work for me to do.”

Topics Discussed
cord prolapse, Covid, Emergency caesarean, General anaesthetic, Induction, informed consent, MGP, NICU, Regional hospital, Surprise pregnancy, tertiary hospital
Episode Sponsor
It’s that crazy time of year again, when most of the country is waiting for the biggest sale of the year
ahead of Xmas, Black Friday! Our friends at iL Tutto love this time of year, it’s when they offer the
biggest savings across their Nursery Furniture range to their pregnancy and new family audience.
If you haven’t heard of iL Tutto, they’re an Aussie brand that make premium, stylish & comfortable
Nursery Chairs along with baby furniture to make the perfect nursery. Their known best for the
biggest range of Stylish and Supportive Nursery Chairs in Australia, along with their CoZee Co-
sleeping Bassinets, of which are available at both iltutto.com.au and Baby Bunting.
For Black Friday, starting from Wednesday 23 rd of November at 6pm until Wednesday 30 th November,
they are offering HUGE savings across iltutto.com.au where you’ll find their biggest range.
Save up to 40% storewide including their range of Cots, Chests, CoZee Breeze Co-Sleeping Bassinets,
and of course their best-selling Nursery Chairs, including our favourite, the new & stylish Bouclé
fabrics along with their ever-so-comfortable Electric Recliner Chairs that include charging USB ports
for your phone! Their chairs are a mix of creams, earthy tones and greys in a premium fabric that will
last, exclusive to iL Tutto. But fear not, if you miss the sale, they offer 10% off your first purchase
online and also offer free delivery in most metro cities in Australia.
Shop the largest range of Nursery Chairs in Australia during Black Friday! iL Tutto, loved by parents
since 2007.
Only available at iltutto.com.au. Sale excludes any other offer including their sign up code and also
excludes their Signature Collection.
Categories
Related Products
-
The Caesarean Birth Class
4 reviews$198.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






