Postpartum Understanding Vaginal Prolapse After Birth
Understanding Vaginal Prolapse After Birth

Pelvic Organ Prolapse - The biggest cause of prolapse is pregnancy and birth – almost 50 per cent of women who have been pregnant will have some kind of vaginal prolapse after birth.
What is a prolapse?
The pelvic organs, which include the bladder, vagina, uterus and bowel, are held in place by the pelvic floor muscles and supporting tissues (known as fascia and ligaments). These help to join the pelvic organs to the walls of the pelvis and keep them in place. The pelvic floor muscles are often described as a hammock in your pelvis; they support your pelvic organs from underneath.
Pelvic floor issues can arise when the tissues that support your pelvic floor muscles are torn or stretched, or weakeded. During pregnancy the weight of your growing baby and the hormones in pregnancy can contribute to a weakened pelvic floor. Torn muscles most often occur as a result of instrumental birth (when your obstetrician uses a vacuum or forceps to help you birth your baby).
How common is prolapse?
After birth, up to 50 per cent of women will experience some form of prolapse. This occurs when the ligaments and muscles that support the pelvic organs have been stretched, which causes the organs to drop down and bulge from the vagina or rectum.
Pelvic organ prolapse is treatable and the best thing you can do in pre-conception or pregnancy is to see a women’s health physio. Everyone’s pelvic floor is different, hence the exercises that work for one woman may be detrimental to the next. Personalised care and guidance from a professional is the best way to prevent and/or treat prolapse.
Statistics show that instrumental births and a long second stage (pushing stage) are significant contributors to pelvic organ prolapse. The methods to prevent vaginal tearing are similar to those that prevent prolapse; stay active and birth in an upright position with perineal support from your midwife as your baby crowns. If you can, avoid an epidural and instrumental birth as both are associated with prolapse.
Types of Pelvic Organ Prolapse
-
Vaginal prolapse: when the walls of the vagina become overstretched and bulge downwards towards the vaginal entrance. The bulging can be the front vaginal wall with the bladder in front of it or the back vaginal wall with the rectum immediately behind.
-
Uterine prolapse: the uterus (womb) and cervix (opening to the womb) drop down towards the vaginal entrance and may protrude outside the vagina.
-
Bladder prolapse: the bladder causes a bulge in the vaginal wall. This usually occurs because of weakened pelvic floor muscles, which support the uterus, bladder and bowel. It can occur by itself or it may happen alongside other types of prolapse.
-
Bowel prolapse: when the bowel bulges forward into the back vaginal wall.
Sign and symptoms of Prolapse
If you experience a long pushing stage, instrumental birth or a third or fourth-degree tear, your care provider will most likely refer you to a women’s health physiotherapist in postpartum. At your six-week check-up, either with your obstetrician, private midwife or GP, they will do a pelvic floor examination and will let you know if you have a prolapse. If you do, it’s highly recommended that you seek out support from a women’s health physio as you’ll want to embrace exercises and lifestyle choices that correct your prolapse, not make it worse.
Signs of Prolapse Include:
-
A sense that your vagina is different. It may feel heavy or like it is dragging. This is a common sensation in early postpartum as your pelvic organs and pelvic floor is still healing; it’s a sure sign that you’ve been on your feet for too long and you need to rest. Later on in postpartum and motherhood, this sensation may be apparent when you sneeze or cough, have been standing for a long time, or have done something very physical such as running or at the end of the day.
-
see or feel a lump. This can be inside your vagina or poking out of it.
-
you have achy pain in your pelvic region or back.
-
you have difficulty going to the toilet. You may need to urinate a lot, have trouble emptying your bladder or bowel, or urinate accidentally.
-
have a urinary tract infection (UTI) that often comes back again.
Treatment for Pelvic Organ Prolapse
There are so many things you can do to help manage a prolapse and reduce your symptoms, including:
Seeing a women’s health physio:
A women’s health physiotherapist will accurately diagnose what type/stage of prolapse you have and give you lots of reassurance and advice to help manage it. The earlier you book in, the better!
Pelvic floor exercises:
Everyone seems to know a little bit about pelvic floor exercises but do you know if you’re doing them correctly for your body? Guidance from a physio will ensure that you know how to locate your muscles, you understand the difference between contracting and relaxing them and you understand exactly what exercises will help your symptoms.
Bowel and bladder health:
Embrace correct breathing and exercise techniques and antigravity positions to ensure that you’re going to the toilet and not worsening your prolapse.
Social support:
share the load with your partner, family and friends when it comes to parenting and housework; two things that can definitely affect your pelvic floor health.
Pessary:
Think of it as a push-up bra for your pelvis. Physiotherapists commonly fit a pessary in the early postnatal period. It’s a small plastic or silicone support that is placed inside the vagina to decrease the symptoms and discomfort associated with a prolapse.
Our Podcast Picks for You
Categories
Related Products
-
The Birth Class
106 reviews$249.00The empowering online childbirth education program that will help you confidently prepare for birth.
Get your copy of our Perineal Massage Guide in your inbox
Keep Reading
We think you might enjoy these articles

Why planning for postpartum is just as important as planning for birth – and how to do it right

Cracked Nipples: Causes, Treatment and Prevention

Caesarean Birth Recovery
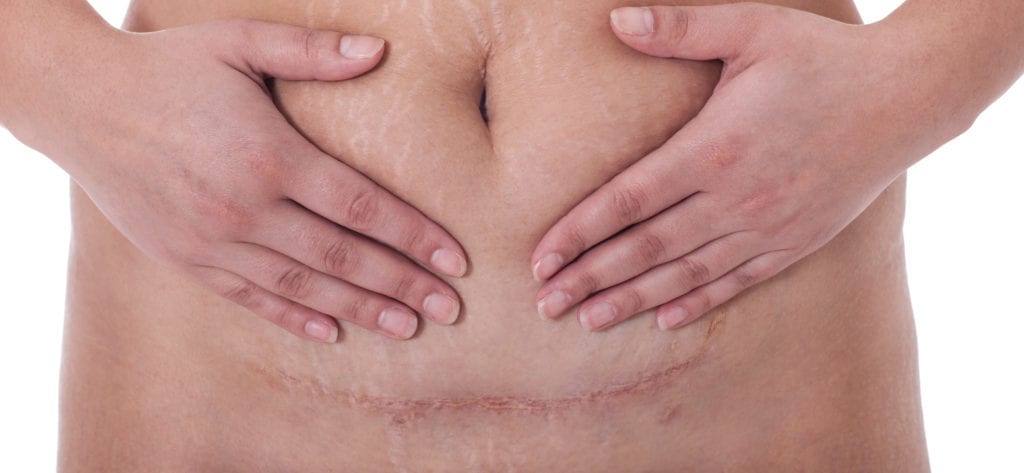
What is a C-Section Shelf?
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






