EPISODE 454
Kirsty – uterus transplant, IVF, planned caesarean
At the time of recording, four Australian women have received uterus transplants in Australia, three of whom were born without a uterus (MRKH syndrome). It’s so exciting to see such significant advancements in women’s reproductive health and I’ll always be grateful to be in the position to interview mothers and share their stories. Enjoy Kirsty’s story, it’s definitely a memorable one.
“In my first birth, after a long labour I had an emergency caesarean and a significant postpartum haemorrhage that resulted in the need for a hysterectomy. I was in ICU in an induced coma to help with healing and as soon as I woke up we started talking about how I would have more children because prior to my hysterectomy, I wanted three children. I conceived Violet very easily so I just assumed that I would be able to have all the babies I wanted and it would come very easily. I had one-and-a-half fallopian tubes and both ovaries left and we were speaking with the midwives and doctors early on about our options. They reiterated that I would still be able to do IVF and go down the surrogacy route which meant someone else would carry our embryo. My mum offered straight away but we also chatted to my sister-in-law about the possibility.
“When I was pregnant with Violet I took for granted how wonderful it was to be pregnant. When you lose something like that and know you can’t go back – it’s really hard. There was so much grief around it but also, I had a beautiful, healthy baby and we were surrounded by the support of health professionals, friends and family.
“When I was in hospital I remember thinking that if we could transplant a liver and a heart, surely we can transplant a uterus. At about six months postpartum I joined a hysterectomy facebook group and someone posted about the clinical trial in Australia. I sent an email to the contact address on the website and the next day I received a reply from Dr Jana Pittman. She explained that it was still in the early stages but I could get started by getting a referral from my GP. Jana also explained that I needed to present with a team; a donor and a recipient. My mum was on board and my husband was supportive although at that stage I’m not sure he realised how serious I was. Mum had to be a blood and tissue match to me, she had to be in perimenopause (not menopause, fit, healthy and a healthy uterus. It took six months of pre-testing and then two days before Christmas 2022, Jana called me to tell me that they had an international doctor visiting in January to do the transplant.
“The uterus is the oven – it doesn’t create or provide hormones so it’s purpose is to carry a pregnancy. Neither of us had to take medication beforehand. The uterus is very vascular so to keep it alive, they needed two arteries and veins. Mum went in at 6am and it took 12 hours; my surgery only took six hours. We were very positive it would work but there was always the chance that it wouldn’t. When I woke up in recovery they told me straight away that it all went okay and they wheeled us into our shared room and we both slept through till the next morning.
“I got my first period thirty days post-surgery. The doctors told me to expect my period within the first three months if everything went well. I was very surprised that it happened so quickly; I was still swollen and sore and walking very short distances. I was so excited because it was the ultimate reassurance – it was working as it should. I’d already done IVF and had five embryos – that was a requirement of the clinical trial.
“Initially I was told it would take six months of healing before we did an embryo transfer but Sweden had started doing it three months post-op and I was happy with that. It was a discussion with the renal team who were overseeing my anti-rejection drugs so I had to change my prescription and once that was all good, I was ready for the transfer. We flew to Sydney on April 19th for the embryo transfer and everyone was really excited to be at this next stage of the process. I was awake and watched it all on the screen; it was really interesting. That was Henry – the first cycle worked!
“I was doing home pregnancy tests twice a day for two weeks. I saw two lines but I really wanted to hear the results from Dr Deans. She called us on May 1st and it was the best; I had tingles from my toes to the top of my head. Every week I was glad that I’d made it to another week. I don’t have the nerve that connects to the uterus so I couldn’t tell if I was having contractions so I needed regular scans to monitor my uterus. I had early spotting which was nerve wracking but I was using progesterone pessaries and I had classic early pregnancy symptoms and ended up having pregnancy sickness till 20 weeks.
“The research isn’t strong enough to support a vaginal birth and it wasn’t something any of us wanted to risk – that pressure on the uterus. Many transplant recipients have their babies by 36 weeks and many are born premature. Most women who are having uterus transplants are born without uterus’ – not many are going through it after hysterectomy. I always knew I would be having a caesarean birth and we were aiming for 37 weeks. From 34 weeks we moved to Sydney so we were nice and close to the hospital and I was monitored regularly. Thankfully I made it to 37 weeks to the day and Henry was born on the 15th of December.
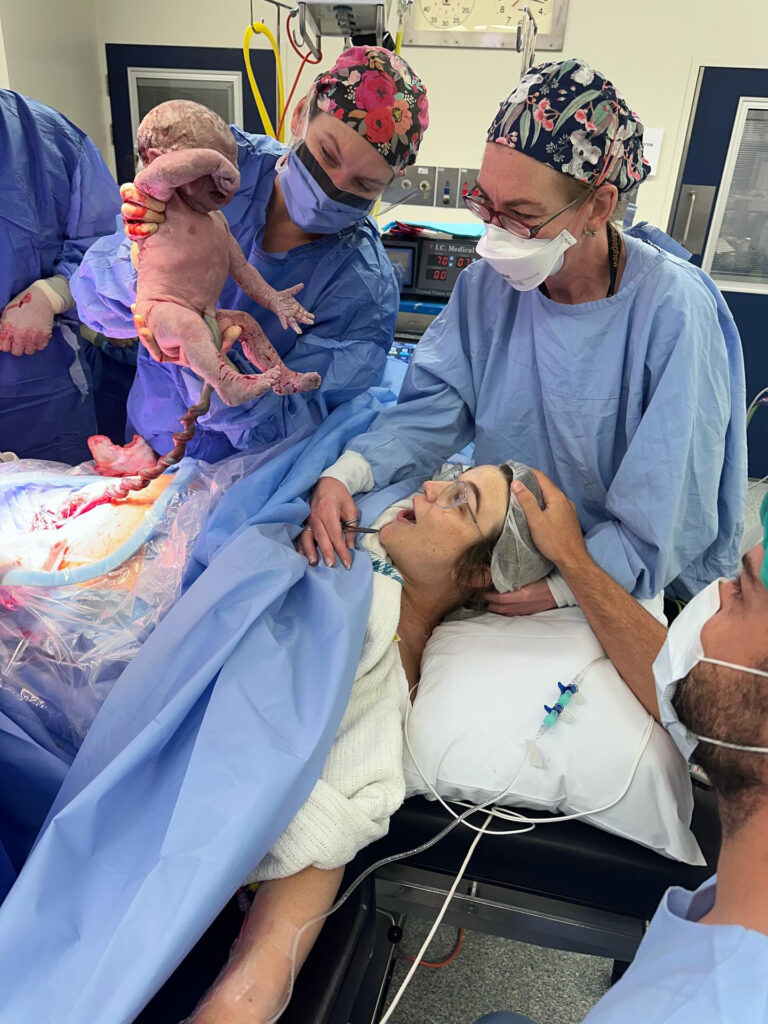
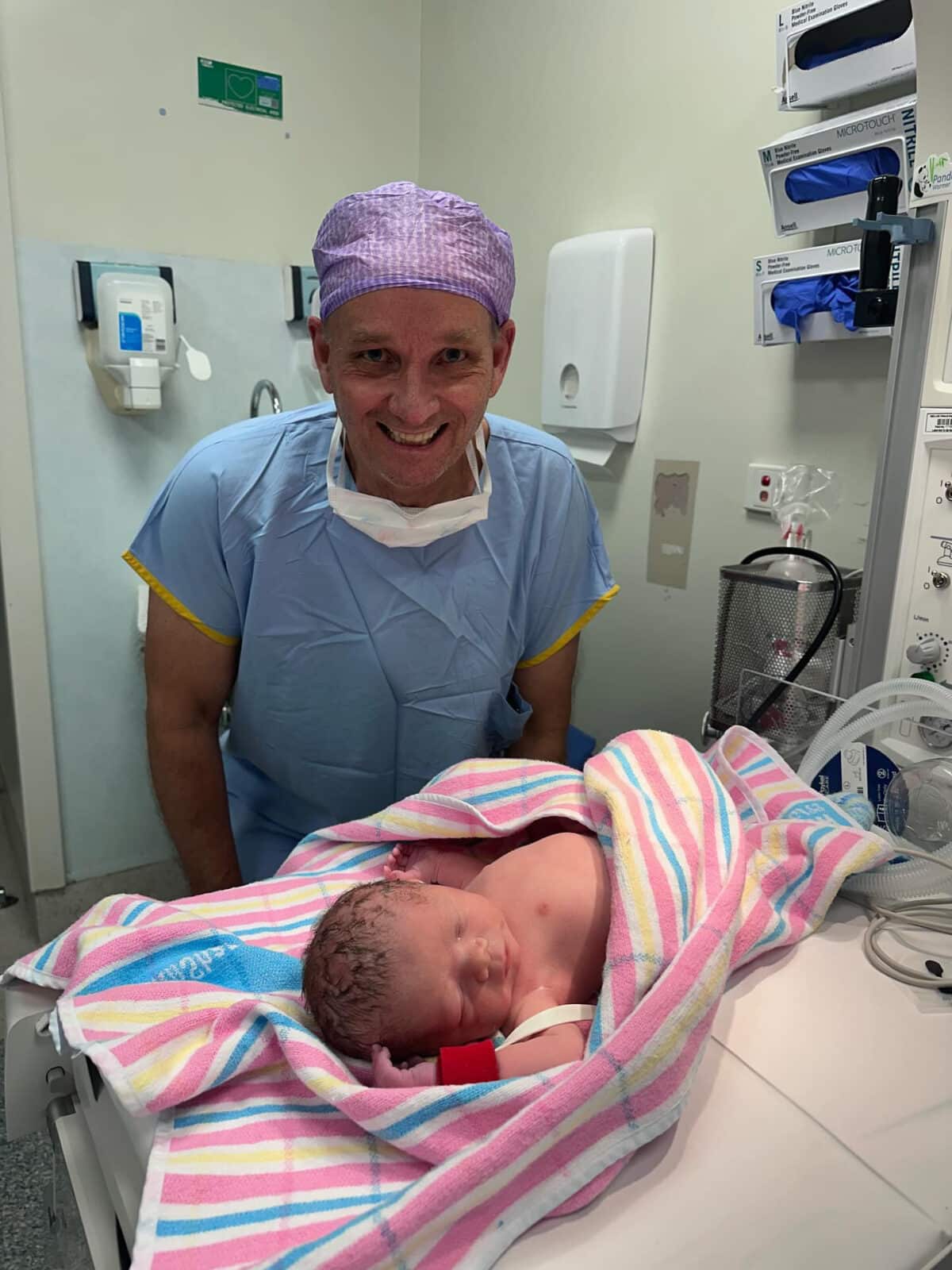
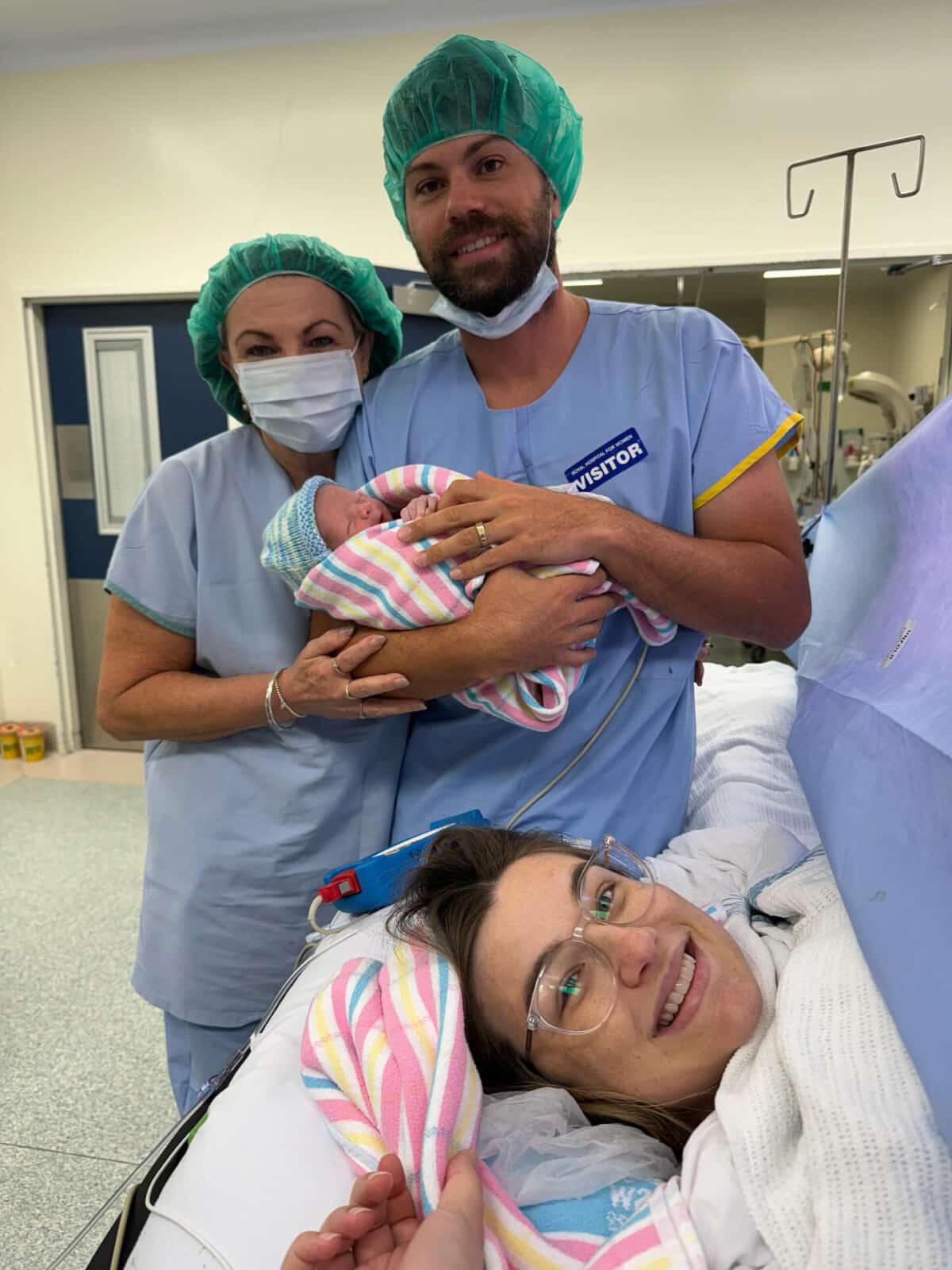
“I was very nervous going into the caesarean. My mum and my husband were with me and the room was full of doctors, midwives, all these beautiful faces including Dr Jana Pittman and my transplant surgeon. It was such a nice experience and everyone was relaxed and taking their time. Henry was transverse and he cried a bit after birth but needed a bit of oxygen. He was given to me in recovery and we got to have skin to skin which is something I missed out on with Violet.
“I didn’t expect the afterbirth pains that were worse when I was breastfeeding. I didn’t have the nerve that connected to my uterus but I still felt the pain and my midwife reassured me that the hormones were doing exactly what they should be doing.
“Breastfeeding has been a really different and challenging experience this time. I’ve had mastitis four times and each time I’ve been admitted to hospital for IV antibiotics and because I am immunosuppressed, I have to take infection really seriously. Unfortunately I was advised to stop breastfeeding because of my health. I’ve been a mess; I really love breastfeeding and I wanted to continue with Henry so it’s been difficult to let it go.
“Now we’re talking about whether I save the uterus for future births or have a hysterectomy. The clinical trial allows you to have it for five years or two pregnancies. I’m on a lot of drugs that have lots of side-effects so it’s definitely better to have the uterus removed if we don’t decide to have more pregnancies.”

Topics Discussed
hysterectomy, IVF, Mastitis, Planned caesarean, Two Babies, uterus transplant
Episode Sponsor
If you’re considering The Birth Class, now is the time to buy. It just got bigger and better thanks to new content that enhances your birth education and preparation experience, including:
- A cheat sheet for your birth partner. This simple outline takes your support person through early and active labour – what to expect, how to support and what to say when challenges arise
- Images of birth positions – the ideal addition for visual learners
- 3 meditations to release tension, foster trust and navigate a change of plans
- An illustrated guide to antenatal expressing – everything you need to know about collecting and storing colostrum
GET 20% OFF FOR A LIMITED TIME WITH THE CODE: ABS2024
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






