Podcasts Annabelle- private midwifery care, postpartum confinement
EPISODE 356
Annabelle- private midwifery care, postpartum confinement

“Tom and I got married in June 2020 and then a year later we decided to start trying. I have regular cycles and I’ve been tracking them since I was in high school so I was quite aware of when I was ovulating. We conceived soon after we started trying but that pregnancy ended in an early miscarriage. I had been quite stressed about conceiving and after the miscarriage, I knew I needed to relax and we conceived Jonah on the next cycle.
“I was a bit anxious even though my blood tests showed really good hCG levels. After a few weeks I realised that I should try to be happy and excited and at about 8 weeks I got a dating scan and they told me that everything looked good. I’ve always been a bit of a midwife wannabe and I’ve been listening to the podcast so I knew I wanted midwifery care but I didn’t know that you needed to get a MGP referral from the GP early on. I missed out on the MGP programme at The Royal Women’s so I also sought out a private midwife through Mama Midwives and developing that relationship was so lovely. I felt super supported by my midwife and her team. Most of the women who go to Mama Midwives are planning homebirths so we saw my midwife antenatally and postnatally and I just had a hospital midwife and a student midwife at the birth. My student midwife was such a good support and she had three kids herself.
“Throughout my pregnancy my mum was battling leukaemia so it was bittersweet to experience pregnancy with her. She passed 10 days after Jonah was born; we took him to palliative care when he was five days old and she was so happy to meet him. It was covid so we had to jump through so many hoops to see her. Tom, Jonah and I are living with my dad now and it’s so lovely to have so much support.
‘At my 40 week appointment they were asking me about his foetal movement and I hadn’t been focussing on it much because my grandfather had died from covid in Malaysia so I was quite shaky. A few days later I was anxious about it again and they did another CTG and baby was doing well but because I’d been in twice after 40 weeks, the OB offered me an elective induction. Before that I was really against it but I told her what was going on and how concerned I was about the baby, so she scheduled it for 40+3 and she also offered me a stretch and sweep and I was already 3cm which was amazing. That meant I could skip the cervical ripening and go straight to breaking my waters. The hospital was really busy and they kept pushing me back so they told me they’d call when they had a bed.
“I started getting tightenings so Tom and I went for a walk and they got more intense and when we got home I told him that I thought I was in labour. I got on the birth ball and put on the TENS machine and at midday I called the hospital because contractions were five minutes apart. The midwife encouraged me to stay at home and keep going. By 5pm it was getting more intense so I called the hospital again and they told me to come in. We spent a few hours in ED before we went through to the assessment centre so when I got in I asked for a vaginal examination but the midwife just presumed I was there for the induction and was feeling anxious. They put the wireless CTG monitor on me because they wanted a trace for about 20 minutes and when the midwife came in she told me she didn’t think I was in labour. I was like: really? Because I was so confident that I was in labour, and my student midwife thought the same, but the midwife pointed to the trace and she said she wanted it to look a certain way.
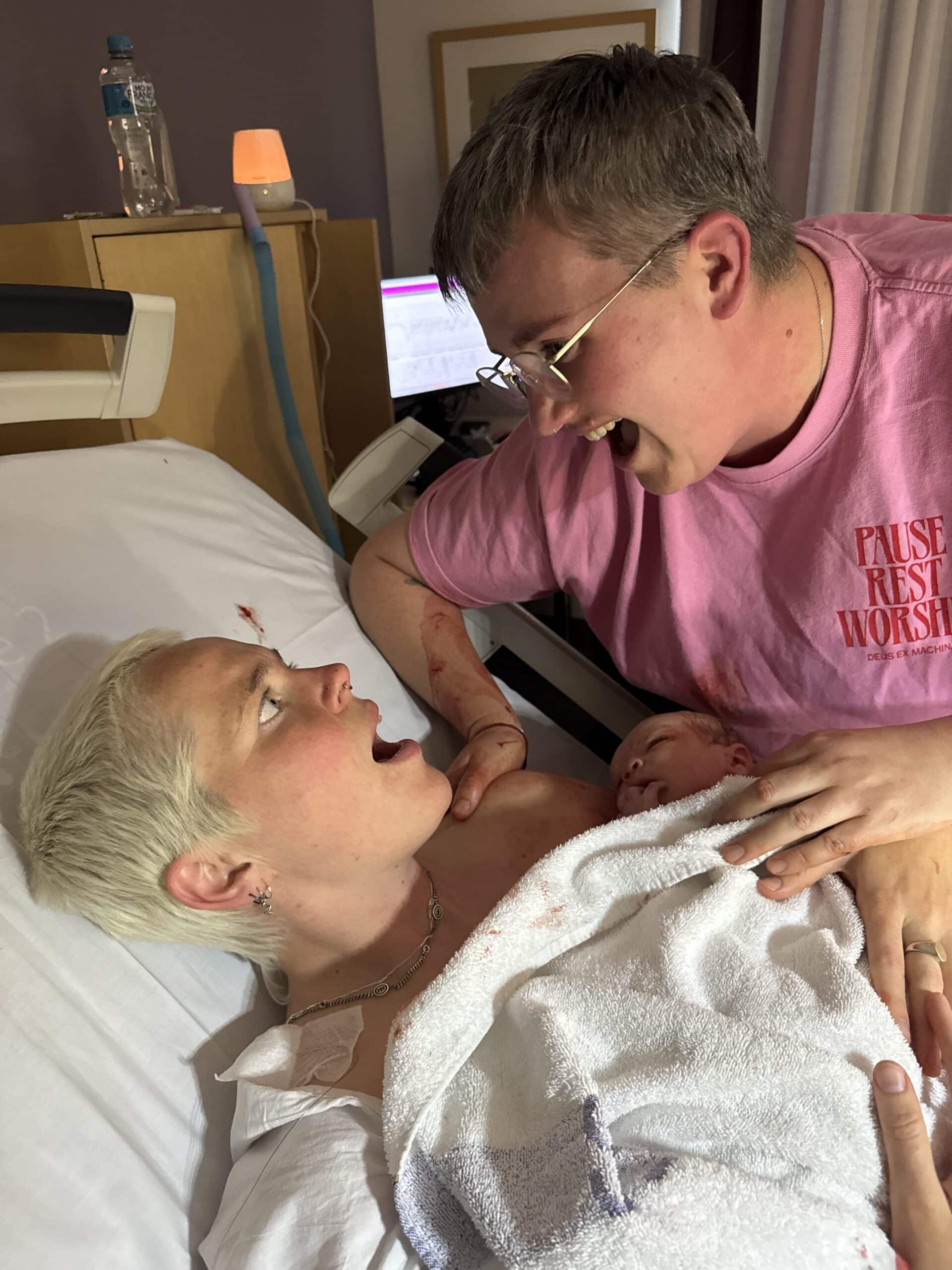
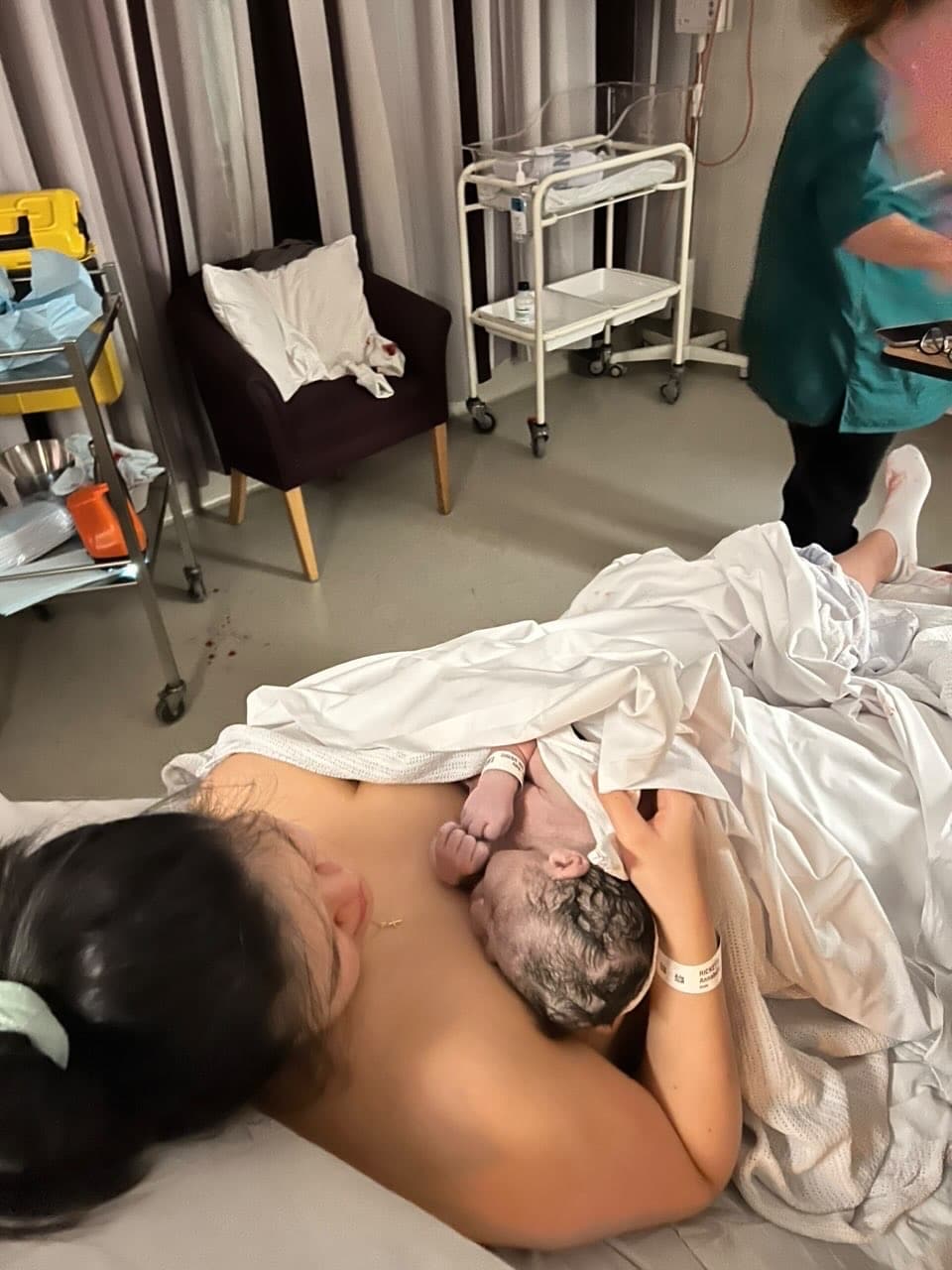
“At 9:30pm there was a shift change and a new midwife came in. She looked at me and said: this is different to what they told me, you look like you’re in labour. She offered to check me and she laughed and told me I was 7cm. I was in shock but I felt so vindicated and so happy. The moment I stood up I felt a “pop” but I had disposable underwear on and my underpants caught my waters. From that moment I felt intense pressure and it took me aback; I hadn’t prepared for that much pressure. I could feel him moving down and I waddled down the hall. When I got into the birth suite I immediately got on all fours on the floor and started pushing. It was a really overwhelming sensation and I beared down really hard but my midwife encouraged me to pant to slow down. He was born within twenty minutes and I distinctly remember the moment the midwife passed him between my legs and his eyes were open and I looked at him and felt like I knew him; I knew his face. It was such a bizarre feeling and I was so giddy, on a huge hormonal high.
“During my contractions I’d remember to just be thankful, I would talk to myself and tell myself I was thankful and happy and that new life was on its way. I’m religious and I was praying and I knew that when I was in pain I went inwards and I’d prepared Tom and my student midwife for that and asked them not to talk to me or touch me.
“The midwife had made a point of reading my birth preferences and she knew I wanted a physiological third stage and so she got me on the bed and then 15 minutes later I had a few contractions and felt the urge to push and even though I didn’t really care about it at that stage, I birthed without the syntocinon. They put my legs in stirrups and while I was feeding Jonah they gave me a local anaesthetic which hurt more than the entire labour and then they stitched my second-degree tear.
“We had some latching difficulties in the first week or so but we saw a lactation consultant and as Jonah grew stronger, his latch did too. I stayed in hospital for two nights and by then I was ready to go home and I wanted to do my best to take him to see mum.
“Mum came home for palliative care and she passed about a week later. Navigating postpartum alongside losing mum was so hard and I wouldn’t wish it on anyone and yet having the extra support of my dad and grandma and being able to grieve together.
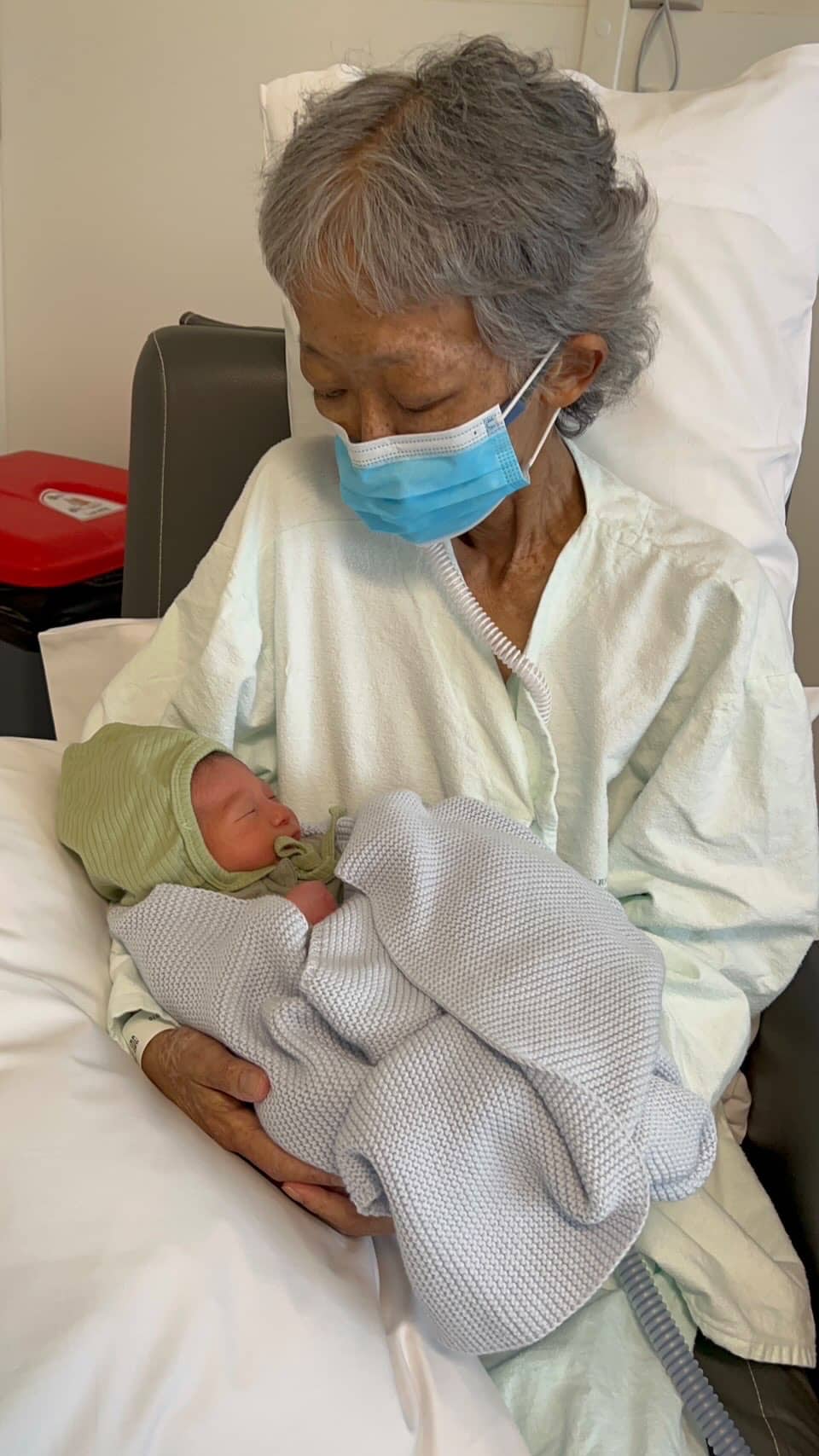
“My mum had always talked about traditional Chinese confinement in postpartum and we spoke about it alot during pregnancy. My grandmother really took care of me despite the fact that she’d lost her husband and daughter within a month. She kept reminding me to lie down, to not wash my hair and she made me lots of fish soup and chicken wine soup to warm and nourish me. She also gave me a red date drink which helped my milk supply so I credit my good supply to that. I fed Jonah next to mum’s bed and it really did feel like a blessing that he was there…he brings me so much joy.”

Image by Hilary Walker

Topics Discussed
Physiological birth, physiological third stage, Private midwife, Student midwife, TENS, Traditional Chinese confinement
Categories
Related Products
-
The Birth Class
108 reviews$249.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us