EPISODE 428
Kirby – Infant loss, breech and VBAC

“Everything went really smoothly for Maeve’s pregnancy. She was flagged for growth-restriction from 28 weeks so I had fortnightly growth scans to monitor her and she was breech for most of the pregnancy; I tried spinning babies but she wouldn’t turn. I was at peace with an elective caesarean; I just wanted her here the safest way possible. I was booked in for 39 weeks but I went into labour a few days before so I had an emergency caesarean and she came straight to me in theatre which I was really grateful for.
“When I fell pregnant with my second, we had moved to the South Coast of NSW and my baby, Minnie was head down so I started considering a VBAC. At 39 weeks I went for a big walk and a swim in the river and I started having contractions. My midwife encouraged me to come in for monitoring and I was 5cm. Labour progressed quickly and Minnie was born at 10am. I stayed in hospital for one night and then I was keen to get home.
“When Maeve started kindy we decided to try for a third baby but I started to bleed at six weeks and I miscarried at home. It was very upsetting and sad but at the same time I knew that miscarriage was common.
“When we were ready to try again, we ended up not conceiving for six months so we saw a fertility specialist who wasn’t too concerned. He ran a blood test and encouraged us to keep trying. We returned to him after another six months and he encouraged me to do a fallopian tube flush which I didn’t find too painful; it was just a bit uncomfortable. It was an opportunity to also see the exact shape of my uterus and it turns out I have a septate uterus which is quite normal aside from a slight dip at the top. On the next cycle I fell pregnant with our little boy Walt. I started spotting at six weeks and of course I was thinking the worst but an ultrasound showed a heartbeat and that was really reassuring. They could see a large hematoma but Walt looked really happy so we just had to wait to see if it would resolve which it did.
“At my 16 week appointment I was discussing my birth options with my obstetrician and he did a scan and as soon as began the ultrasound he turned to me and told me there wasn’t a heartbeat. I felt like I wasn’t in the room. I had to go for another ultrasound and the sonographer gave me the opportunity to look at the screen as it can help you process and it was very clear to me that he had passed. I think I did need to do that because I wasn’t registering that it was happening. When my husband arrived we talked about our options; I could birth him or have a surgical evacuation but I knew I wanted to birth him; I felt like it would help with my grief. I took the medication that stops the placenta working and I was to return to the hospital two days later.
“They were an awful two days. We had to tell the girls that there wasn’t going to be a baby which was really heartbreaking. I went into hospital for the induction and we had a beautiful midwife who held our hands and prepared us for what was to happen. The labour took a few hours and he was born. He was perfect but small and fit in the palm of my hand. We were encouraged to spend as much time as we wanted with him; we did his footprints and took photos and then we went home.
“I was so desperate for answers and asked for all the tests but nothing came back so we didn’t get any answers. We were told that it was just unlucky; I think the statistics are 1 in 200 in the second trimester so they encouraged us to have faith and try again.
“We fell pregnant a couple of months later and I was happy and scared. I kept telling myself that it was a different pregnancy and would be a different outcome. I was offered extra scans for my peace of mind; my fertility specialist wrote ‘TLC’ on my referrals. I had spotting again at six weeks so I was very anxious but again, it resolved. The 12 weeks scan was perfect and I had scans every fortnight afterwards and they were all fine. I remember at 16 weeks that it would be ok.
“A few days after my 16 weeks scan I woke in the middle of the night and noticed a lot of pink fluid. I went into emergency and they could see the baby was ok and there was lots of fluid around him. A registrar did an internal and she could feel the fluid pooling at the cervix and she told me that I would most likely birth my baby soon after. They transferred me for a proper ultrasound and they could see two large hematomas and then I was taken to the birth suites. I remember thinking that it wasn’t a coincidence; it felt like we were missing something. We were told it was inevitable that we would lose the baby bit they also said the waters may reseal. I stayed in the hospital for three days and it looked like the waters were resealing and the hematomas were shrinking. But on the third day I started having contractions and the doctor said that it may be an irritable uterus but I had a feeling it was labour and I was right; it was really quick that night. We named him Alby. I kicked into survival mode at that point and I don’t think I was processing what was going on, I was just trying to get through it physically. The emotions didn’t come till later.
“It was so hard to go home and tell the girls again. Particularly Maeve, she was so sad and asking questions like: why do all our babies die? I reached out to Bears of Hope and I saw a lovely counsellor through there and she was great. It was really hard trying to show up for the girls but they were also a big comfort.
“My husband and I both knew that we wanted to try again but we weren’t getting any answers from the testing. In the autopsy they said it was a placental abruption but there wasn’t a cause. The hospital gave us the option to try naturally again but I didn’t think I could do that. We booked in to see our fertility specialist again and he suggested surgery on my uterus because he felt that may have been a contributing factor in my losses. I had day surgery and I also made an appointment with a reproductive immunologist and he ran some extra blood tests that we hadn’t done before and he suspected immune issues that were affecting my placentas.
“Emotionally I was in such a hard place; it was an unbearable sadness, like grief on grief. I was doing everything I could to stay well; walking every day, doing acupuncture, seeing my counsellor. Almost another year passed when I didn’t fall pregnant and I was 37 at this point. I really started to feel the pressure of time ticking away and it felt like a really low point; it felt cruel to be going through infertility after so much loss. I was starting to feel quite angry and hopeless and all around us people were falling pregnant and welcoming healthy babies.
“I had a small bubble of people I could talk to at that point. When you experience loss people say the wrong thing even if it comes from the right place. There’s nothing anyone can say to make it better but I definitely felt supported.
“We went back to see the immunologist and he ran one more test which was a DQ Alpha. It’s debated and not all doctors believe it’s relevant but basically it’s a genetic match between me and my husband that causes an immune response to the placenta. It’s like an allergy so it can get worse with each pregnancy. The treatment is Lymphocyte Immunisation Therapy (LIT) where they extract about 40,000 of my husband’s white blood cells and they inject it under my skin, almost like a vaccine, in the hope that my body will make antibodies and the body will be less hostile towards the placenta.
“We decided to do IVF and we got 27 eggs and 17 were mature and fertilised. By day six we had eight embryos and six were able to be tested and frozen. We prepared for a transfer on the next cycle and I got a call from the clinic and out of the seven embryos only one was normal. I was quite upset but my mum encouraged me to be positive for this one embryo but it was really hard.
“I fell pregnant on that transfer and I couldn’t believe it. That pregnancy was baby June. From the very start I was full of anxiety; it was the longest nine months of our life. I was on a lot of medications and I had spotting again at six weeks so I stopped the blood thinners and went on bed rest. I decided to see a private obstetrician because I needed continuity of care and the support of someone who knew our story. He was excellent; very patient and caring and everything that I needed. I saw him weekly for scans and he encouraged me to come in whenever I needed for peace of mind scans.
“At around 16 weeks it was really hard. We didn’t tell a lot of people that I was pregnant because I couldn’t handle hearing ‘congratulations’ until I had a baby in my arms. At that time I had felt the baby move for about a week and I woke up one morning and couldn’t feel her move. I went into the hospital and it turned out she was in a weird position but she was okay and I cried all the way home from relief. I was 20 weeks when we told the girls and by that stage they were asking a lot of questions and were suspicious of my bump. Mentally it was really hard; I was always checking on the baby’s movements, I had a lot of fear, I couldn’t imagine a live baby and I couldn’t buy anything because if I did I felt like something would go wrong.
“I was about 34 weeks when I felt like I could start thinking about the birth and my obstetrician was happy to support me in having a vaginal birth. I prepared with The Birth Class and your book but at 35 weeks I had a bleed so I went into hospital but my obstetrician wasn’t concerned. I was always worried about the baby’s movements and I chose to have an induction at 39 weeks for my mental health. The day before the induction I had a vaginal examination and I was already 2cm so I didn’t need a balloon catheter.
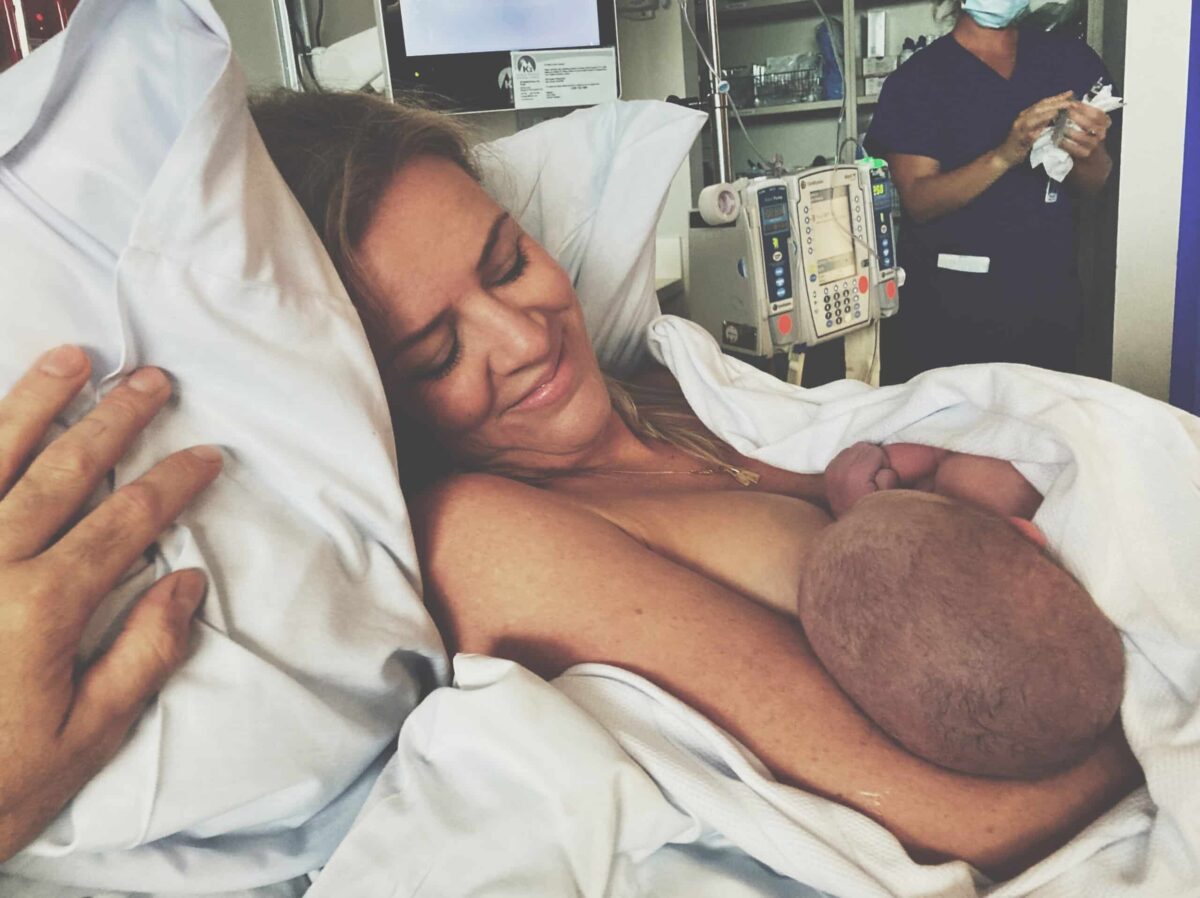
“I woke up on the morning of the induction and I was so excited. We hadn’t told the girls because I didn’t want them worrying but I made a point of thanking my husband because I couldn’t have done it all without him. It was 2pm when the syntocinon drip started and to be honest I was just really excited. I didn’t have any pain relief because I wanted to stay really present. She came out screaming which is what I needed to hear; it was such a relief. I lifted her onto my chest and I was so amazed to have an alive, crying baby.”


Topics Discussed
second trimester pregnancy loss, septate uterus, five babies, VBAC, Tongue-tie, Breech, Miscarriage, Emergency caesarean, IVF
Episode Sponsor
Today’s show is brought to you by Kiwi Co.
Panda Crate is a subscription box filled with playful open-ended activities backed by research and designed especially for naturally curious and creative babies and toddlers with a Panda Crate subscription from Kiwi Co.
Your baby receives a new crate filled with two months worth of products and content every other month, whether you have a brand new baby or a trailblazing toddler, the Panda Crate is perfect for your little ones developing brain. Build a foundation for early learning this new year with Panda Crate from Kiwi Co. Get 50% off your first month with the code ‘Birth Stories’
Categories
Related Products
-
The Birth Class
108 reviews$249.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






