Podcasts Brigitte
EPISODE 327
Brigitte
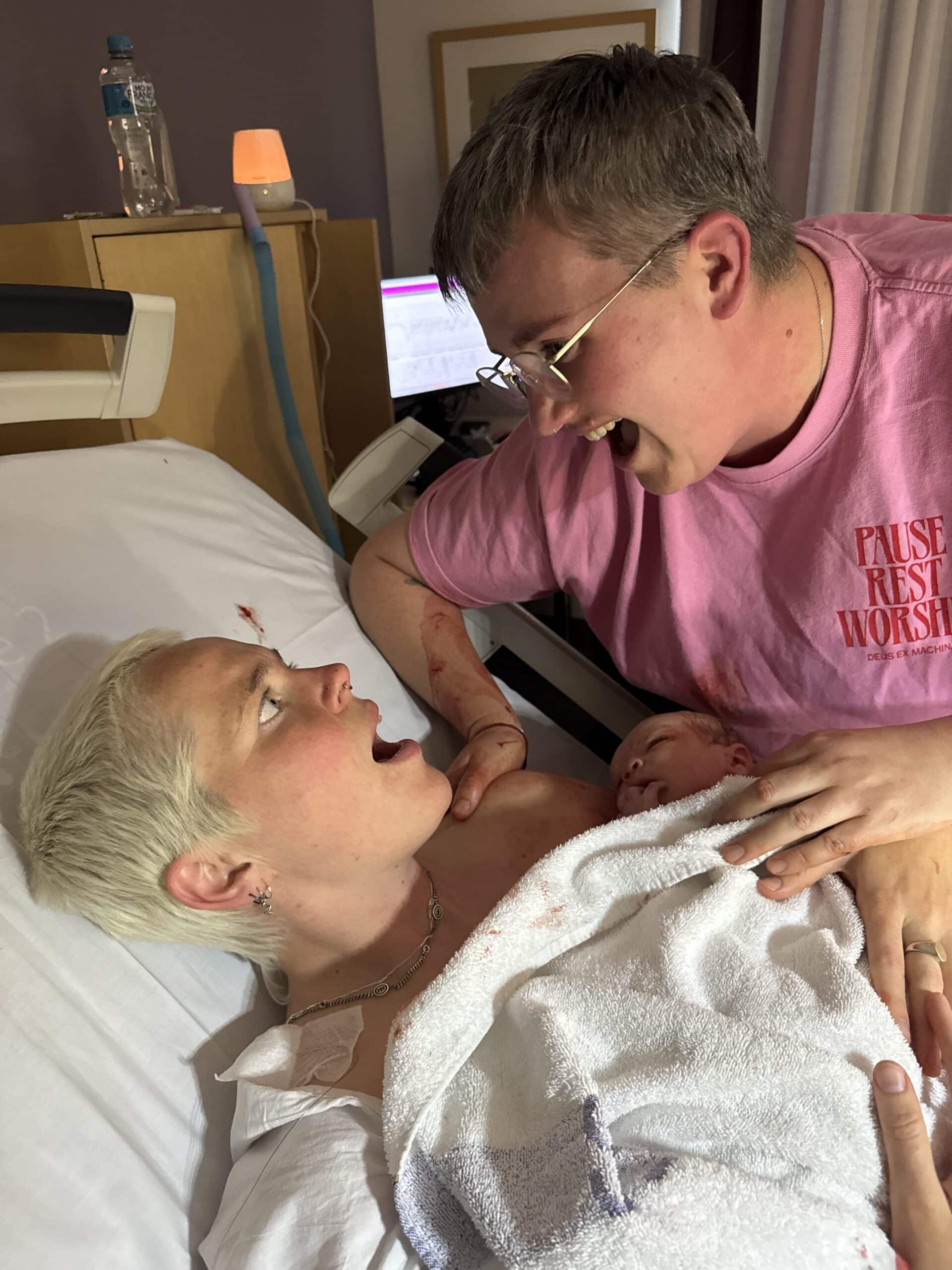
At 10 weeks Brigitte noticed pink mucous and an ultrasound confirmed that she’d had a missed miscarriage; her baby had stopped developing at 7 weeks. She was given two options: wait for another ultrasound or have a dilatation and curettage (D+C).
“I opted for the D+C and it was really hard. Three of my work colleagues had just announced their pregnancy and it just felt really challenging. Frankston hospital offered me counselling and I refused it at first but then I realised that it was something that I really needed. Because we fell pregnant straight away that first time we presumed it would happen easily again. My period returned immediately but mentally I wasn’t really ready and then my period became quite inconsistent. A friend recommended an acupuncturist and it was so interesting the way they approach fertility. The acupuncturist recommended my partner get a sperm analysis. He started going to acupuncture as well and we both cleaned up our diet and a few months later I found out I was pregnant again. A few days after that positive test I started bleeding and I knew I was miscarrying again. We decided to give up for a while but then that next month I fell pregnant with Isla.
“You want to get excited and positive but after a loss it’s hard not to worry. I held off telling my partner, Jack, for a week till I’d seen my GP and had blood tests because I didn’t want to disappoint him. I also requested a dating scan with my GP and it showed a strong heartbeat. I opted for continuity of care with a private obstetrician through the public hospital. I paid out of pocket about $1200 and that payment needed to be made by 28 weeks. I also got a Medicare rebate of about $200.
“I wanted a natural physiological birth and I was really motivated to achieve it. I had my birth preferences but I also knew that plans change and I was open to that. I’d been listening to your podcast and we both loved The Birth Class, we just wanted a lot of information about what to expect and what our options were. We also did one through the hospital so we knew the hospital’s policies and recommendations, especially in regards to Covid.
“My waters broke and the hospital asked me to go in especially because I’d noticed that my baby’s movements had reduced overnight. They put me on the monitor and gave me a button to press whenever I felt her move. My waters had broken but they were the hind waters so my obstetrician came and broke my waters and I was hooked up to the syntocinon drip. It started off as mild period cramps but within the hour it really ramped up. I was getting Jack to squeeze my hips which helped a lot but then after four hours Isla’s heart rate wasn’t picking up as quickly as they’d like after contractions. The midwife pressed the button and all these people came into the room. They gave me an injection in my leg to ease the contractions. The CTG belt kept moving and they couldn’t get a consistent reading so I agreed to a fetal scalp monitor. I was using the gas and TENS machine and I was coping, I didn’t want anyone to push pain relief on me.
“By 1am it was getting really intense, there was sometimes no break between contractions, but I hadn’t dilated any further at all and I’d been going for 10 hours. I knew I needed the epidural then; I was physically and mentally exhausted. They turned the syntocinon drip down so I had more breaks between contractions so I could stay still for the epidural. It was so good to have a sleep, I woke up from a 20 minute nap and there was something wrong with the epidural and it was starting to wear off so I had to start on the gas again.
“A few hours later I was fully dilated and they put my legs up in stirrups. I was so uncomfortable and my hips were really sore but nothing really helped with that. I pushed for just over an hour and then the obstetrician admitted that we weren’t getting anywhere and she suggested a caesarean. At that point I agreed, I just wanted it to be over. When we were doing The Birth Class we didn’t think we’d need to listen to the caesarean module but then I thought it was best to listen and I’m glad I did because I knew what to expect. We waited thirty minutes and they prepared me for theatre.
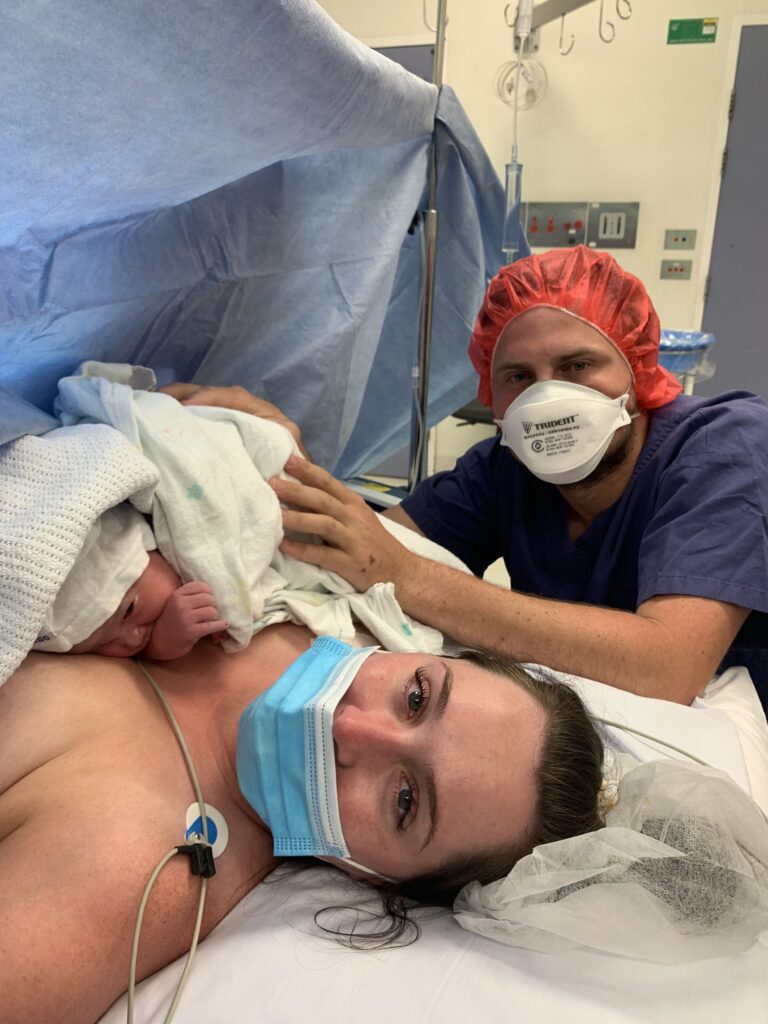
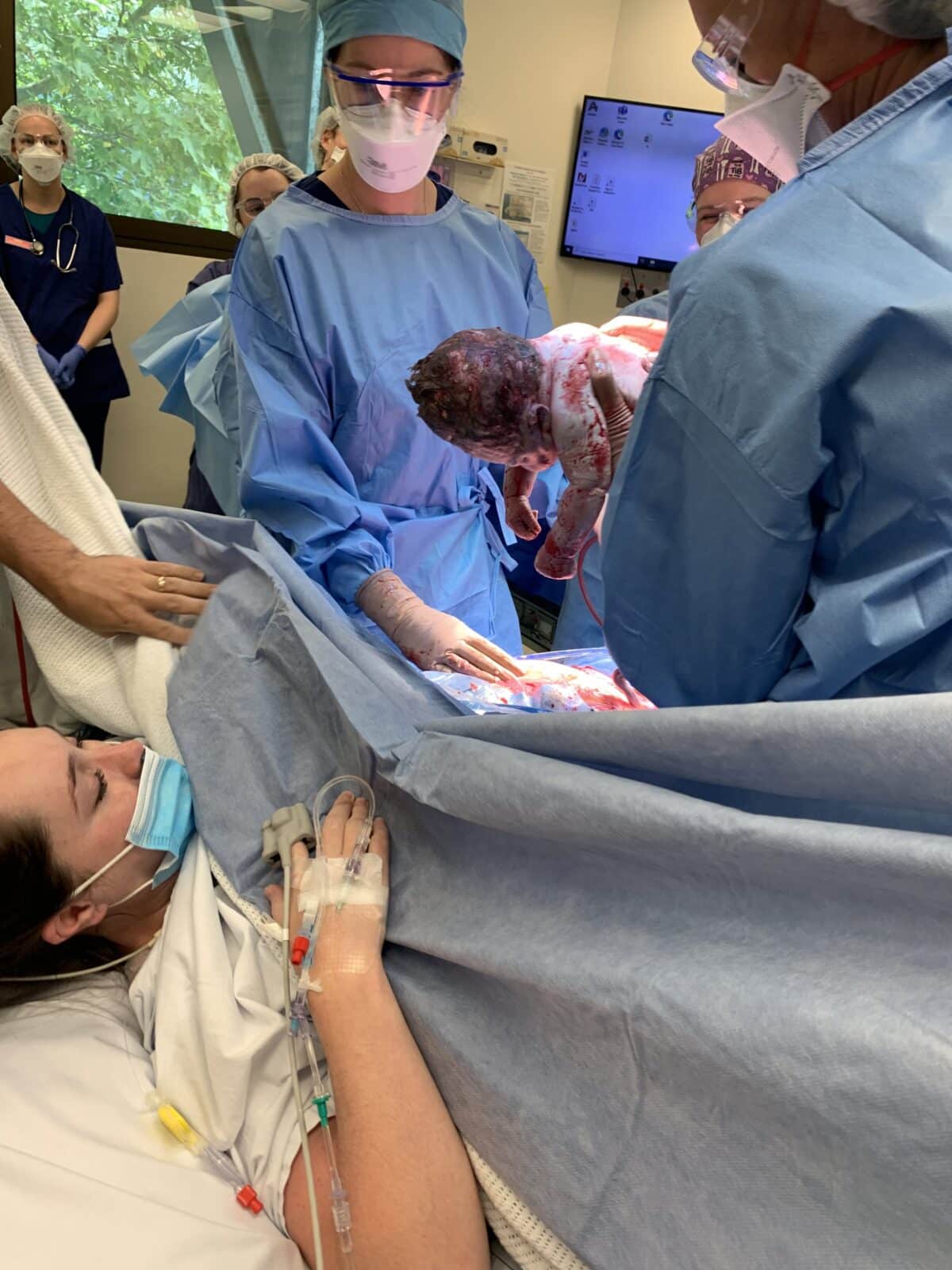
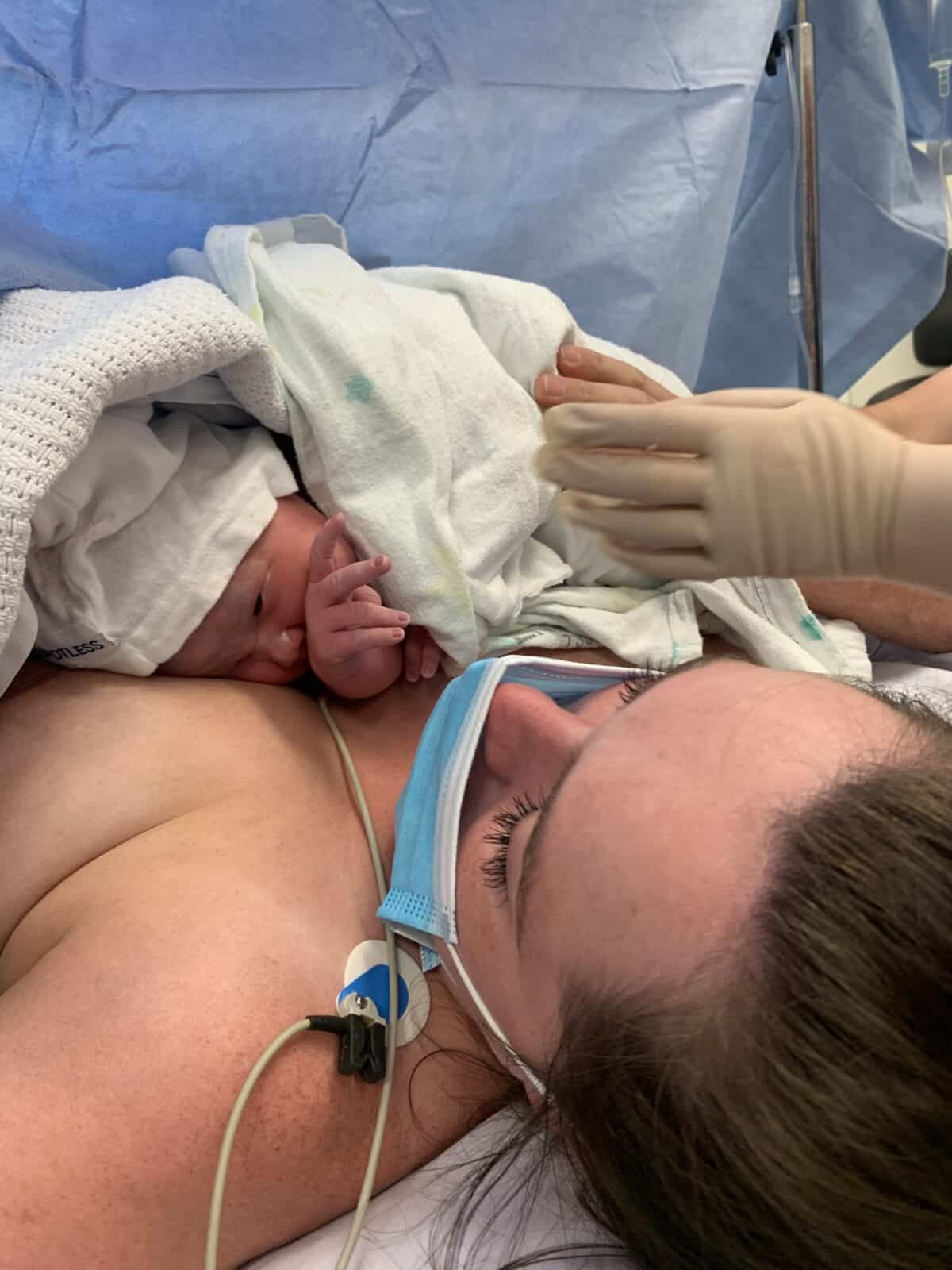
“I could feel them tugging her out and then they pulled down the drapes and there she was. She was very loud once she started crying. The paediatrician looked over her and then she came to me for skin to skin. Once they’d transferred me off the operating table they noticed blood in my urine and they were worried that my bladder had been perforated but thankfully that wasn’t the issue.
“I had done some antenatal expressing which was handy because on the second day she wasn’t latching well and she was quite jaundiced so the colostrum was very helpful in clearing her jaundice. I had pain relief before getting out of bed the next day; I felt a bit like a hunchback getting to the toilet but overall I think I recovered quite well. I stayed in hospital for two nights but in hindsight I wished I had stayed an extra night as my nipples were cracked and I had some breastfeeding issues. I had a midwife from the hospital see me twice and then I saw a midwife from the obstetrician’s rooms two weeks postpartum and then I saw my obstetrician at six weeks.”
Topics Discussed
Acupuncture, Epidural, Induction, Miscarriage, One emergency caesarean, Private obstetrician, Public hospital
Episode Sponsor
What’s better than mum’s supporting mums? Sometimes the support required is more than just a scented candle. That’s where Belly Bands, the female-run, Australian-made brand comes in. Made by mums for mums.
Belly Bands create award-winning pregnancy, postpartum and recovery products to provide support and comfort at every stage. Their most popular 3-in-1 band can be used through the whole pregnancy journey and is even TGA approved!
Each product is individually produced to ensure superior quality and a perfect fit to alleviate back pain, increase comfort and assist in postpartum and Caesarian healing.
They’ve helped support over 60,000 bumps and have thousands of 5-star reviews. Medically backed and regarded as one of Australia’s most trusted and recommended maternity essential products, it makes the perfect gift for yourself or your loved ones.
Let Belly Bands support you. Available online directly at bellybands.com.au. Free shipping for orders over $89.
Receive 20% off your order with promo code ABS22.
Categories
Related Products
-
The Birth Class
108 reviews$249.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us