EPISODE 303
Chantelle
Chantelle fell pregnant for the first time in June 2019. She was elated and instantaneously told their family and friends but she noticed that she was having cramps and lower back pain. A week later she noticed brown spotting. Her GP referred her for an internal ultrasound that didn’t reveal anything of concern so she decided to start tracking her hCG levels with blood tests every second day. The next week on the morning of her follow-up scan, Chantelle woke and realised she was bleeding.
“I had an internal ultrasound and they spotted I had an ectopic pregnancy which was close to my ovary and it had ruptured the left fallopian tube. I remember I couldn’t lie flat on my back in bed for the whole week prior and there was a pressure build-up in my stomach. The doctor said he usually gives options for treatment but because it had already ruptured they had to do the tube removal that afternoon. I had an overwhelming realisation that I could have died from it. Rowan and I were both in shock, we were both crying and we’d lost our baby. The surgery recovery was really hard, I had bad shoulder tip pain from the laproscopy and I caught a virus from being in hospital.
“I was so upset about losing my baby and I just wanted to be pregnant again. The stress and trauma of it all played a big impact on my cycles; I bled for three to four weeks after my operation and then I didn’t get a period for 50 days. It was so odd because I usually had a 28 day cycle. I started testing my ovulation and I wasn’t ovulating and I was sinking into a deep, dark pit of depression. I hated my body because it was failing me. It took us over six months to conceive again.
“I got a positive test but I wasn’t sure how I felt about it. I couldn’t get excited because I didn’t know if it was going to be another ectopic pregnancy. I was six weeks pregnant when I went back to work and I started to get brown discharge again. I knew it was ectopic straight away. I went straight to the Womens and Children’s Hospital after work as my doctors had told me if I had a positive pregnancy test and similar symptoms I needed care immediately. I had another internal ultrasound and the radiologist found it straight away in the right tube but it hadn’t ruptured. They gave me the option of methotrexate to induce a miscarriage and the nurse administered it in full PPE and I was told I need to use a different toilet to Rowan in the days following because you urinate out the toxins. It was really confronting.
“My care was paramount in the hospital instead of recognising my pregnancy loss because ectopic pregnancies are a bit of a ticking time bomb. I took the methotrexate and went home and cried in my bed. When you take it you have to have blood tests every second day and the pregnancy hormone reduced quite quickly. You’re not allowed to get pregnant for three months after taking the medication and that was a relief for me because it was out of my control. I bled for quite a while afterwards because I didn’t have a D+C.
“My GP referred us to a fertility clinic and we started doing some investigations including a hyCoSy where they checked if the tube was patent. I wanted a baby but I was terrified of getting pregnant again and the day we decided to do IVF I got a positive pregnancy test. My period wasn’t even due but I had that similar cramping again.
“After my second pregnancy and ectopic pregnancy I was the angriest person in the world. When I was pregnant for the third time there was not one iota of happiness. I had an early scan and there was a sac in the uterus which was a good sign and I finally allowed myself a bit of hope. Then a day later I felt a gush and there was so much red blood. We went to the hospital for blood tests and ultrasounds but it was so early so nothing was showing up. Days later a scan revealed that the sac in the uterus was a pseudo sac and the embryo was in the exact same spot as the second pregnancy. I bawled my eyes out, I just lost it. I was furious because I knew it was going to happen if we conceived naturally. I opted for the methotrexate again and promised myself that the next time I would do IVF to conceive.
“I was in so much pain that I couldn’t even get out of bed. I knew we needed to get to the hospital immediately. I could barely move and my stomach was bloated; they rushed me through and they did another scan which showed my tube had ruptured and I had internal bleeding. This was 5am and they got me straight in for emergency surgery where they removed the right tube.
“I felt relieved because I knew I wouldn’t have to go through that again because the tubes were gone. To have that off the table was definitely relieving. I was still dealing with the grief of losing another baby but I knew I had some form of control about pregnancies moving forward. I’d had three ectopic pregnancies in one year and I really wanted to love my life again and spend time with Rowan. We spent three months working with psychologists and preparing for IVF.”
Chantelle started IVF and she did all the injections herself but after a week she was bloated and uncomfortable and ended up being diagnosed with ovarian hyperstimulation. She got 22 eggs and out of that she got five embryos. It was a big journey. Two weeks after the transfer she did a sneaky pregnancy test which was positive and later that day she received a call from the fertility clinic to give her the same news.
“The pregnancy felt so different. In retrospect I could see that my ectopic pregnancies were so painful but with Lucy’s pregnancy I was a bit nauseous but I was energetic and grateful and excited. I didn’t get any spotting at all. Mount Barker has a birthing centre and so many of my friends have raved about it. My GP and my psychologist were based there so it just made sense to go there for my pregnancy and birth.
“My pregnancy was really smooth aside from some pelvic girdle pain. I was so excited to do birth preparation so I listened to your podcast every day to and from work. I wanted to listen to every birth story!
“With IVF pregnancies the baby can be a bit smaller and the baby often grows better on the outside than the inside. At our 36 week Lucy wasn’t much bigger than she was at 32 weeks and they really didn’t want me to go past my due date. I pushed them to 39+5 and from 38 weeks I tried everything to get labour going including expressing colostrum. I was walking, walking steps, drinking raspberry leaf tea, inhaling clary sage, I tried everything but she stayed put.
“I went in on Monday for a stretch and sweep but my cervix was still closed. We went in the next day for induction but the midwife couldn’t get the balloon catheter in so in the end we opted for the cervical gel which prompted mild contractions. I used the TENS machine and I loved it an
d the contractions continued throughout the night. At 1am they applied more gel and at 6am they tried to break my waters but it took multiple people and a lot of effort to break them.
“After two hours my contractions hadn’t progressed so I was happy to have the syntocinon drip. The contractions ramped up then, I used my breathing techniques, I was in the shower and had the TENS machine. My midwife kept trying to feel the contractions because there wasn’t much rhythm to them. After many hours of labour I was only 1cm and Lucy was showing signs of distress so they decided to give me medication to ease the contractions. They told me they could up the syntocinon again but Lucy may not cope or I could have a caesarean section. I was back having to make a hard decision and I just sobbed with Rowan. I knew I was there for a healthy baby and I trusted that my body wasn’t going to birth vaginally. I had a thorough birth plan in case I needed a caesarean and my student midwife was all over it.
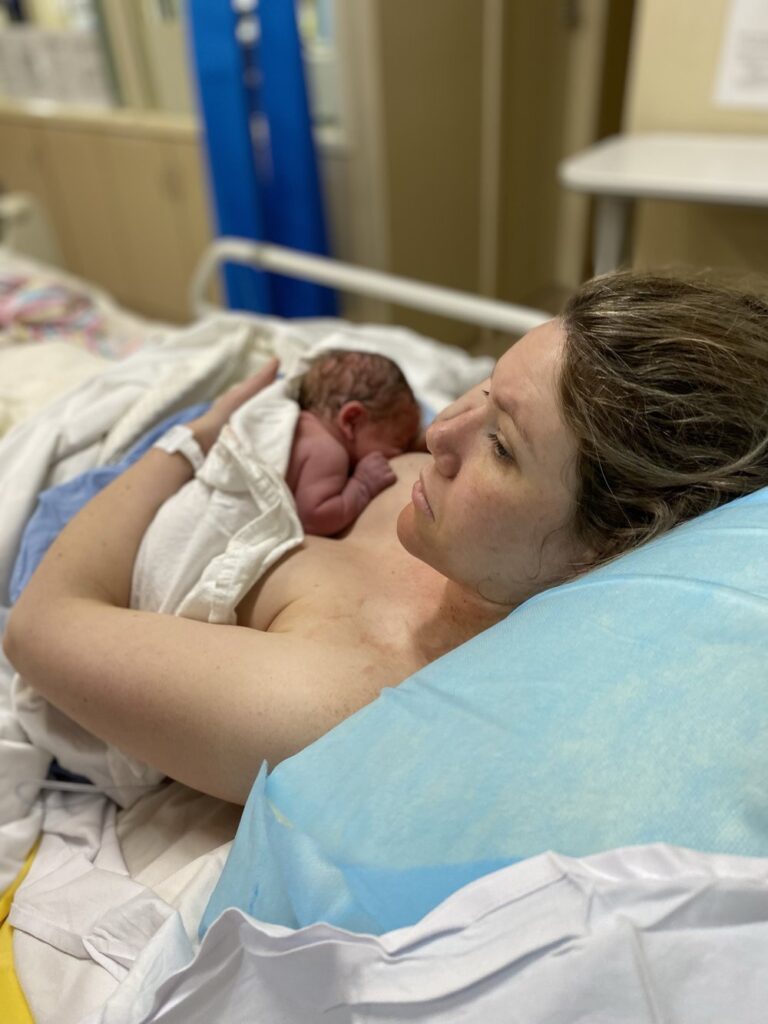
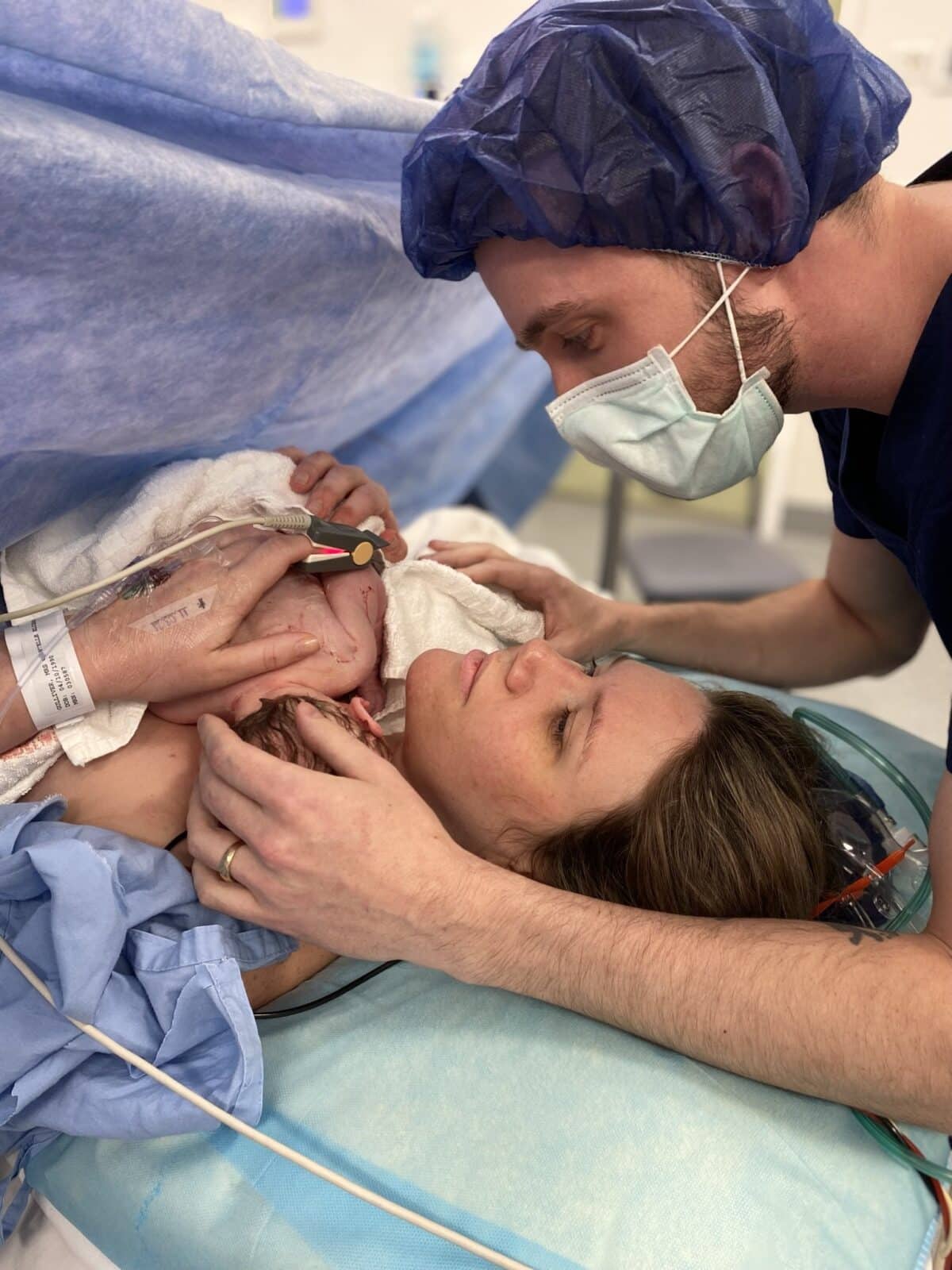
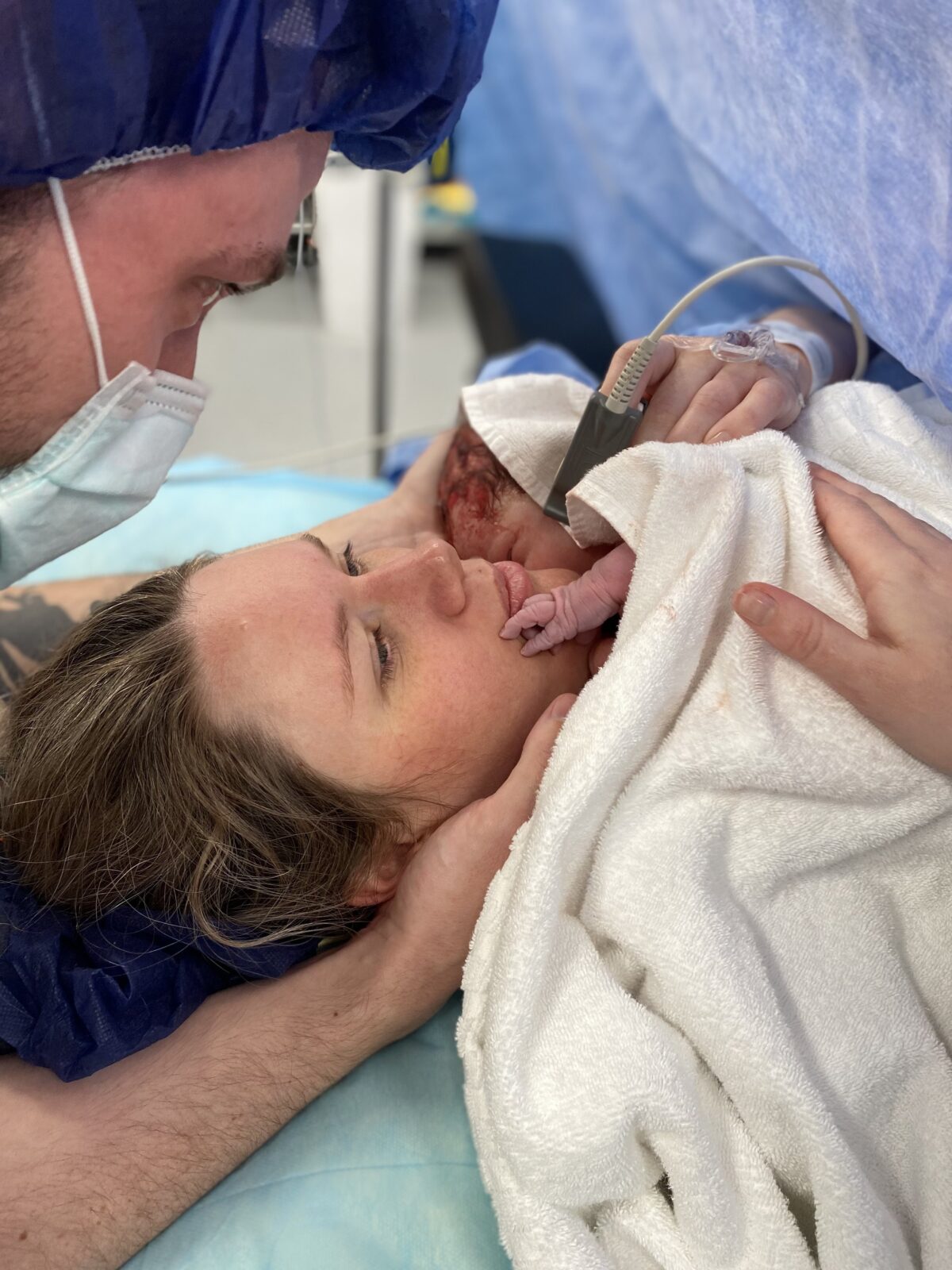
“Everyone in the theatre was excited and as soon as she was born she was on my chest. Rowan and I were crying and shaking. My student midwife took so many photos. The reason why I wasn’t dilating was that I had a bottleneck of uterus that wouldn’t stretch so there’s no way I was ever going to give birth vaginally. The doctors said it could be because of my connective tissue but it really needs more investigation.
Breastfeeding has been really easy for Lucy and I, which has restored faith in my body.”
Topics Discussed
IVF, One emergency caesarean, Ruptured fallopian tubes, Three ectopic pregnancies
Episode Sponsor
Our understanding friends at Bonds reckon that when it comes to babies, anything can happen. And from personal experience, like the time when my Niko went 10 days without pooing as a newborn and we were hit with a poonami in the middle of Westfield I reckon they’re right. That’s why Bonds is introducing Bonds Baby Cover. A comprehensive ‘poo-licy’ for new parents. This tongue-in-cheek policy compensates parents for the first-time parent experience with free Bonds babywear.
There’s cover for ‘natural disaster’ we’re talking grade 5 Poonamis here, ‘Vandalism’ – wilful texta damage to walls and clothing – and ‘Third Party for when ‘it’ goes everywhere and on everyone. Even accidental-probably-on-purpose damage is covered. If my three boys are proof, little cuties can be massive liabilities. Get protection and compensation with Bonds Babywear. To be clear, that’s free product, parentals!
Bonds Baby Cover. It’s insurance that has your back, and their bum sign up now
Categories
Related Products
-
The Birth Class
108 reviews$249.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






