EPISODE 298
Steph
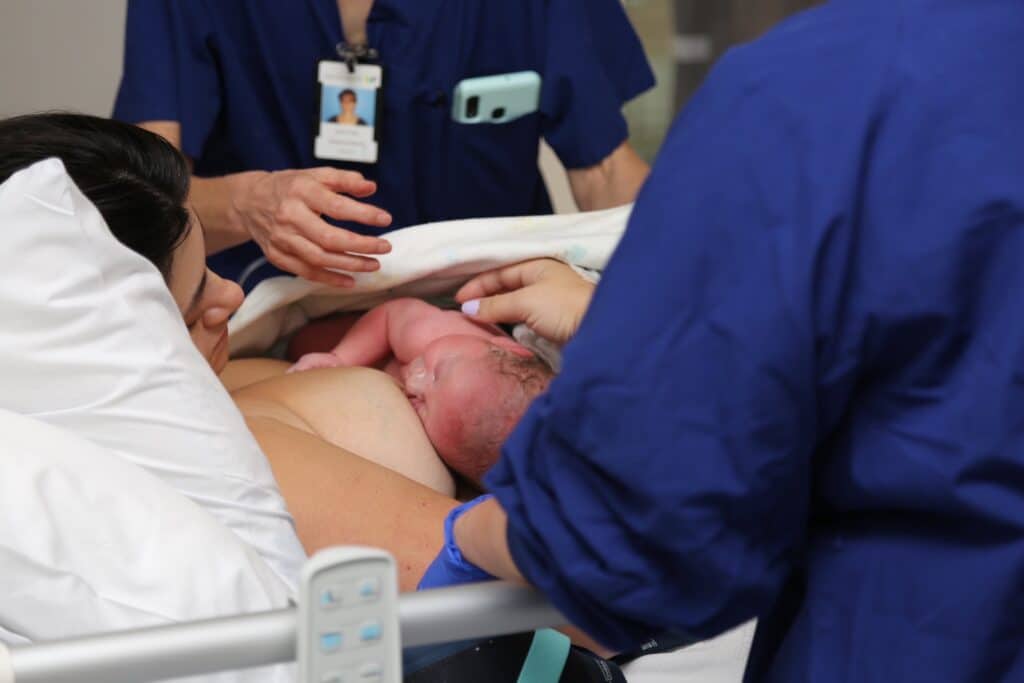
Three months after a chemical pregnancy, Steph conceived again but discovered at 8 weeks that her baby was growing in her fallopian tube, a condition known as an ectopic pregnancy.
“I was 8 weeks and I had a funny feeling…I think once you’ve had a miscarriage you’re walking on eggshells and you’re peeing on a million pregnancy test sticks and I just said to my partner, Ash, something doesn’t feel right. I booked in for a scan because I was so anxious and I asked my mum to come with me. I didn’t have any other symptoms but my gut telling me that something wasn’t right. I’d never heard of an ectopic pregnancy before and I just didn’t understand. The doctor bluntly told me that the pregnancy needed to be terminated. My scan was at 11am and I was in surgery by 2pm so I only had a few hours to process. I’d been internally bleeding for quite some time and if I hadn’t had the scan, and if I had left it, my fallopian tube would have ruptured. They ended up removing my baby and my left fallopian tube.
“They kept referring to her as ‘it’ or ‘the fetus’ and in order to heal I needed to name our baby and every piece of me believed she was a girl. We named her Arie.I got post-traumatic stress disorder so I was placed on the maternity ward and the experience was awful, it was not a nice experience at all. We didn’t know how much we wanted a baby until it was taken from us.”
Steph’s GP advised her to wait a few months till she fell pregnant again but she craved another baby so opted to start trying straight away. Three or four months later she conceived baby Sunny yet she was very aware of the statistics following an ectopic pregnancy; after you’ve had one, there is a significantly higher chance of another. She admits that she wasn’t coping so she reached out to Mums Matter because her thoughts were dark and she felt her mental health spiralling.
“I didn’t take medication, I had a bit of a stigma about that actually. I’m on medication now for depression and anxiety but I did see a psychologist throughout my pregnancies and my postpartum. At my 20 scan I got that reassurance that things could be ok but it really wasn’t until I reached close to term, about 35 weeks, that I felt like it was really happening. Honestly, it wasn’t until I had Sunny that I felt that everything was ok.
“I was very sure that I wanted to be in Midwifery Group Practice because I wanted continuity of care, especially considering my history and my mental health. My midwife also taught me hypnobirthing and she helped me navigate psychological support. I was diagnosed with gestational diabetes so while I would have loved to have a water birth, the hospital didn’t support me because they wanted me to be continually monitored. I didn’t have the education that I do now so I went with it. My midwife suggested an induction at 39 weeks because he was measuring in the 99th percentile but at the time I didn’t know about the cascade of intervention so at the mention of an induction I had no fear, only excitement.”
Steph ended up going into spontaneous labour at 37+6weeks and after driving into hospital, her midwife confirmed that her waters had broken and she was in early labour. Her anxiety was high and her contractions had slowed so she went home and had a plan to return 24hours later for induction. She laboured all night and Ash drove her back to hospital the following morning.
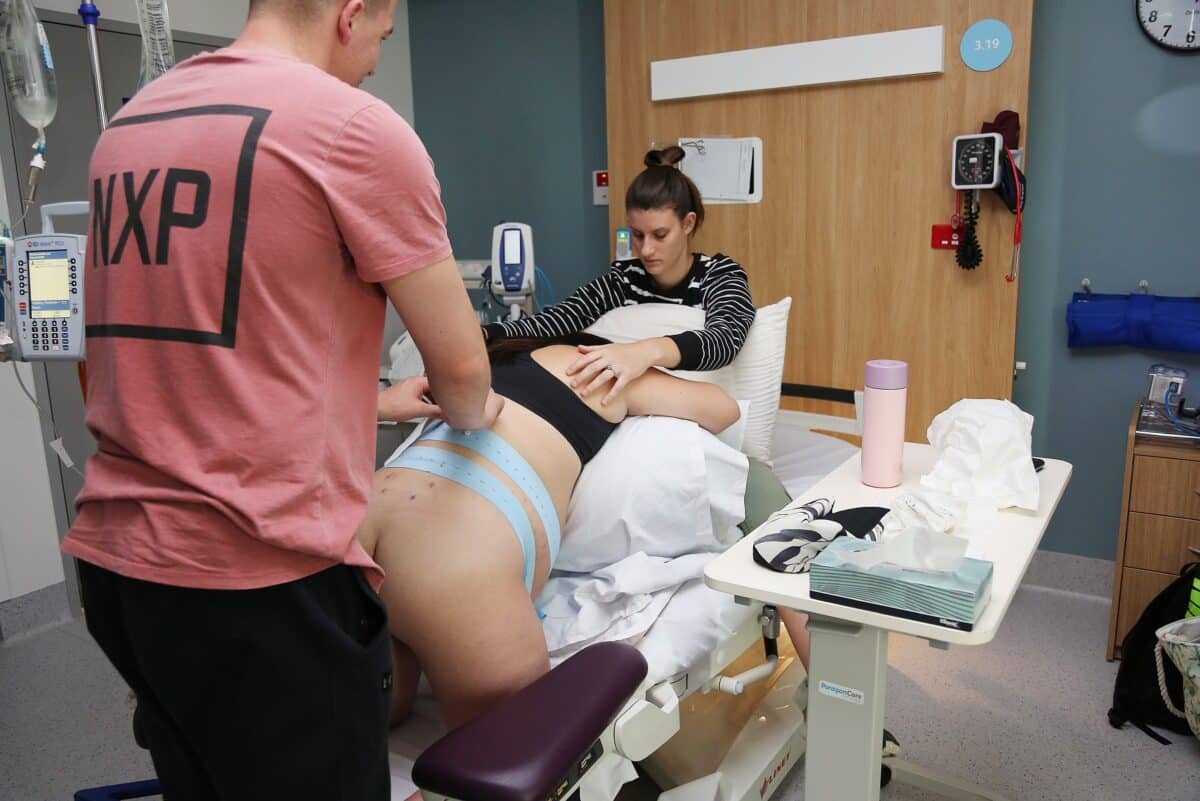
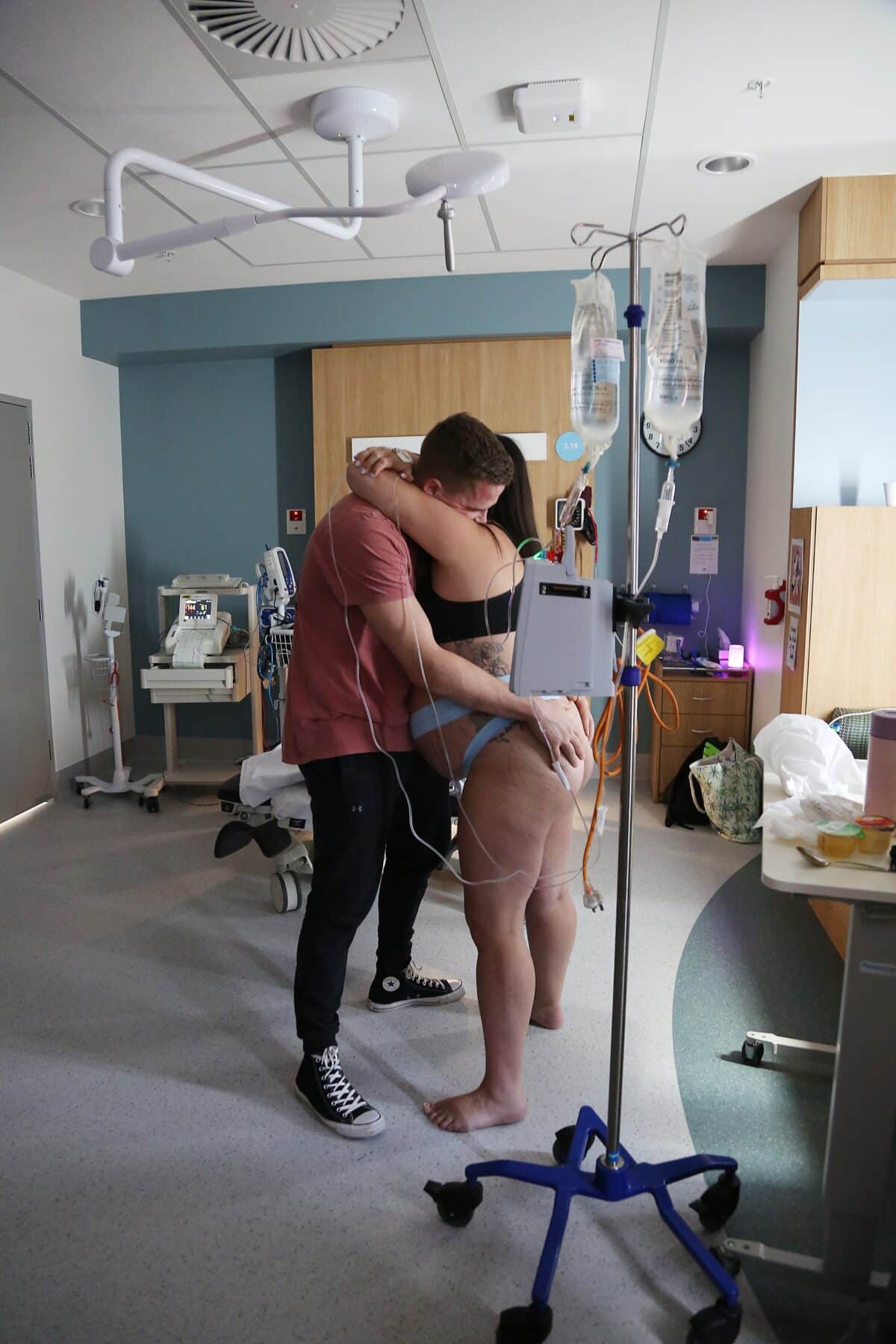
“I was so sure that I wouldn’t want to know how dilated I was but then the excitement took over. I told the midwife I needed to know and I was only 3cm, after 24 hours of early labour. Once I was on the syntocinon drip and on the continual monitor, I had no break between contractions at all. Monique, my sister, and Ash were amazing at supporting me. I had the gas which did nothing apart from making me feel sick. The midwife suggested the water injections but never will I ever get them again, they caused shocking pain. Annoyingly, they did offer relief. I spent about eighty percent of my labour in hospital sitting on the toilet, it gave me a lot of relief just sitting there. My midwife suggested an epidural because Sunny was posterior and she really wanted me to relax and I agreed that I needed a break.
“The epidural was so successful for me, it really made a world of difference. When I was fully dilated I had an awful experience with an obstetrician who walked in and told me I needed to be prepared for an emergency caesarean because my baby was in distress. I was in tears and so upset so Ash asked to speak to the obstetrician outside the room and when he came back in he told me I had an hour to give birth to Sunny before I had to have an emergency caesarean. I ended up pushing for two hours and I well and truly admitted defeat, I felt like I failed. I signed the waivers and I was taken straight to the theatre.
“I asked for the lights to be dim, I asked for no conversation between the staff. But I was pale and vomiting the whole time and I was so ready to meet my baby and know the sex…that got me through.”
Steph passed out shortly after Sunny’s birth because of a postpartum haemorrhage. Ash admits it was the scariest moment of his life and he was alone in a room with Sunny, feeding him expressed colostrum, while Steph was in theatre for another 90 minutes. As well as recovering from a caesarean birth, her cervix was also torn and she lost 1.7litres of blood. It was an incredibly challenging healing process for her but she admits when she got home, with Sunny in her arms, it was a grounding experience that she’ll never forget.
When Sunny was nine-months-old, Steph and Ash went away for a weekend between Covid lockdowns and upon their return home, Steph discovered she was pregnant. After a confronting experience with an obstetrician at her local hospital, she opted for a homebirth midwife and developed the most beautiful, supported relationship with her.
“I was 32 weeks when I was in bed and thinking that I really needed the baby to move. I went to get Ash because I was in pain and I couldn’t help but squirm. We called the midwife, Ash quickly packed the bag and we were on our way to the hospital because we knew we couldn’t have a baby this early at home. I spent the 30 minute car ride on all fours, without my pants on, just hoping my baby wouldn’t come out in the car. I was in denial because I thought I’d get to hospital and they’d stop labour.
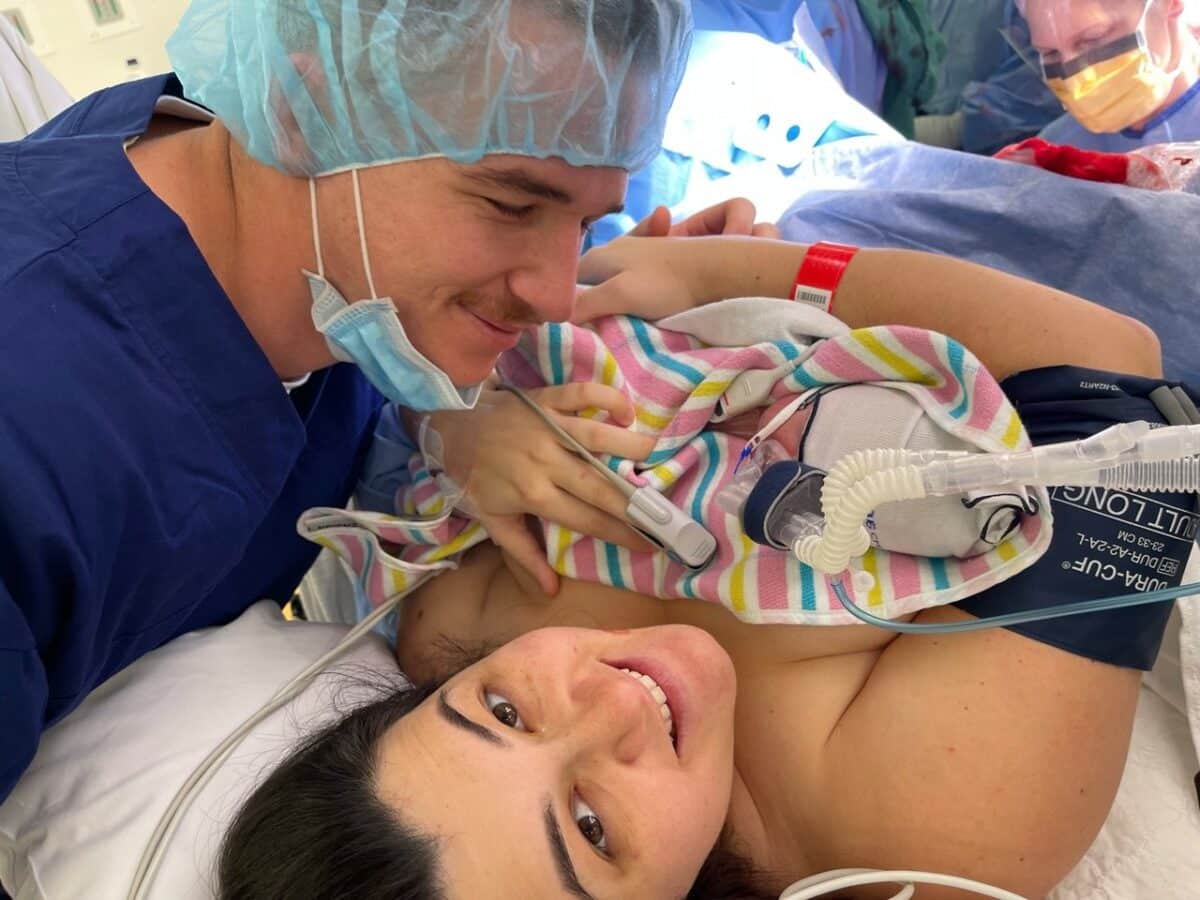
“I remember a huge team of people in there and they prepared me and told us that when the baby was born it may not cry. I was 7cm when I arrived and my waters broke and then everything was a blur. Towards the end they told me I needed to go to the theatre because he was so little and they needed to assist his delivery. I got my VBAC which was a celebration in itself. Otis cried, he let out a huge cry, and he was perfect. He was 2.1kg and I thought for a moment that he wouldn’t need to go to the NICU. I got skin-to-skin with him for about 30 seconds but he was struggling to breathe. He was on CPAP for a week, which was really hard. We’d never seen a NICU and I remember being wheeled in there and you look in and there’s your baby with an eye mask and all these tubes and I didn’t know if it was my baby. I felt fear, I didn’t feel love or a connection. And then they put him on my chest and I talked myself up and I was very passionate about my kangaroo care cuddles from then on.
“I was discharged after one night and I pumped all day and all night. I could watch Otis through the webcam at the hospital while I was pumping – crying and pumping. He stayed in the hospital for four-and-a-half weeks and he ended up spending time in three different hospitals during that time.”
Steph was diagnosed with postpartum depression after Otis’ birth and NICU experience and is now happily and gratefully medicated (and on medication that also allows her to breastfeed).

Topics Discussed
Ectopic pregnancy, Emergency caesarean, Epidural, Gestational Diabetes (GD), Induction, Miscarriage, NICU, Postpartum depression (PPD), PPROM, Vaginal birth after caesarean (VBAC)
Episode Sponsor
Today’s episode is brought to you by DockATot. This multi-award-winning baby lounger is uniquely shaped to recreate a womblike environment to soothe and settle your baby. The DockATot has thousands of 5-star reviews from parents across the world who’ve enjoyed its calming effects on their babies. New parents often say the DockATot is like having an extra set of hands always at the ready because it offers baby a safe place to rest or play wherever you are. Being lightweight and portable, the DockATot can be used around the house and is also perfect for family adventures to the park, beach or beyond.
Handmade in Europe from premium quality materials, the DockATot has become an absolute global parenting must-have. So if you’d love an extra set of hands around the house to help you as a new parent, check out DockATot.com.au and as an ABS listener, you can enjoy 10% off any DockATot and their amazing range of accessories. Just enter the code ‘ABS10’ at checkout.
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






