EPISODE 297
Kate
Kate’s first pregnancy wasn’t planned but she was absolutely delighted with the news. Living just outside of Darwin, she only had two choices for pregnancy care; the local private hospital which had a high intervention rate, or the midwifery programme in the birth centre at the public hospital. She was interested in labour and birth with low intervention so opted for public care in the birth centre.
“In all of my labours, my contractions were close together from the get go. I started contracting ten days past my estimated due date and when we got to the birth centre the midwives encouraged me to settle in, even though I was only in early labour. Because I was there for so long the midwives had to change shifts and I couldn’t stay in the birth centre so I had to move up to the hospital and I found that quite disruptive. I still remember them telling me that I was only 6cm and I felt really disheartened from then on, the language they used made me feel really disappointed. I wanted to get back in the shower but they wanted me to lay down and rest so I did but the pain was really intense and I just lost my mental strength and I opted for an epidural. I was monitored from then on because of the epidural and my baby started showing signs of fetal distress and that was when I was told I would need an emergency caesarean.
“I didn’t know anything about caesareans because it wasn’t something I ever considered for myself. By then I’d been in labour for a really long time and I was so exhausted that I don’t think I could have even pushed out my baby. I was quite disorientated in the theatre and once Sunny was born they put him on my chest but I was feeling like I couldn’t really breathe and having him on me made it worse so my husband, Liam, held him.
“We had a really hard time getting Sunny to latch. Breastfeeding was really painful and I went through all the lactation consultants available to us and at eight weeks he was failing to thrive so we were feeding and expressing to top him up. I ended up using nipple shields to help make my nipple a bit bigger to help him attach and it was smooth sailing from there. We used them for a few weeks till Sunny was bigger and then weaned him off them, they saved our breastfeeding journey.”
Kate had an ectopic pregnancy between her first and second boys. She was still getting regular periods so didn’t know she was pregnant but when she started bleeding mid-cycle she knew something wasn’t right. She took a pregnancy test and when it was positive she knew something was wrong considering the timing of her cycle. She went to the GP and she was sent straight to emergency at the hospital where they did bloods and a bedside ultrasound. She was measuring eight weeks pregnant via her HCG levels and it was confirmed that she had an ectopic pregnancy.
“I knew a bit about ectopic pregnancies so I knew how serious it was. I chose to have methotrexate – mediation to pass the pregnancy – but it didn’t work so I had surgery to have my fallopian tube removed. It was really scary at the time and I was really concerned about my fertility because I knew I wanted more children. They checked my other tube to make sure it wasn’t blocked while they were in there. We had to wait six months after that to conceive because of the medication I took. It took a while for us to conceive when we felt the time was right and there was a lot of stress in our life at that time and I think that contributed. When we did fall pregnant I was quite worried about having another ectopic pregnancy but it was all fine.”
Kate prepared for a VBAC and at 11 days overdue she kindly declined an induction. She had a doula as she wanted to do everything she could to prepare for a VBAC, she also had a lot of things in her birth kit for the possibility of another caesarean. She took probiotics (Lactobacillus rhamnosus GR-1 and Lactobacillus reuteri RC-14) to prevent GBS because if she did have another caesarean, she wanted to ensure she could do vaginal seeding.
“After arriving at the hospital with her partner and doula, she was 3cm and opted for an epidural; soon after her cervix started closing. She tried everything to dilate, including the support from an amazing midwife, but Kate eventually agreed that a caesarean birth was the best option. She did vaginal seeding, optimal cord clamping and immediate skin to skin.
Kate’s third pregnancy was unplanned but she knew from the outset that she would have a planned caesarean.
“When I had my second caesarean they recommended I didn’t attempt another VBAC as my scar was quite thin. I had an appointment with the same obstetrician who helped me birth my first baby, he brought up the possibility of a maternally assisted caesarean and told me that as well as scrubbing in and wearing gloves, I could also have skin to skin immediately after birth. I know some women have to really fight for their preferences and here I was with an obstetrician who was suggesting it.
“I was so confident that I wouldn’t go into labour early but then I woke in the middle of the night before my scheduled caesarean feeling like I was having light contractions. I put it down to nerves but I got up and realised I was in early labour. I called the hospital and they really encouraged me to go in and by the time I got in the car the contractions were quite intense. Once we were at hospital they confirmed that I was in labour and they took me to theatre soon after.
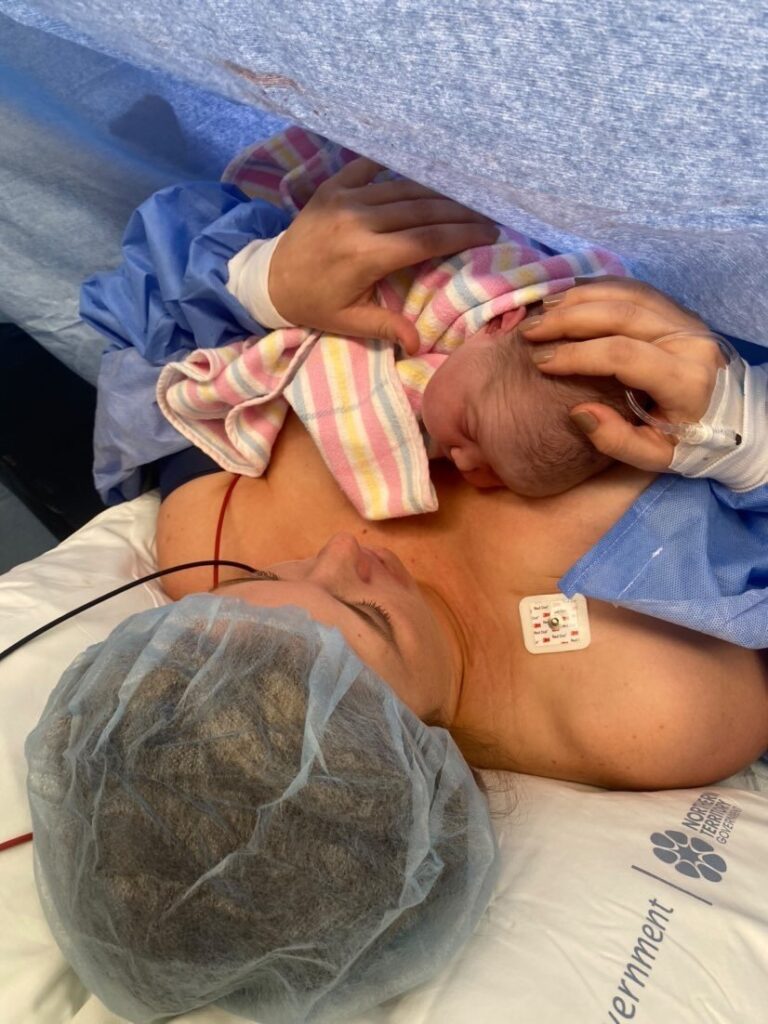
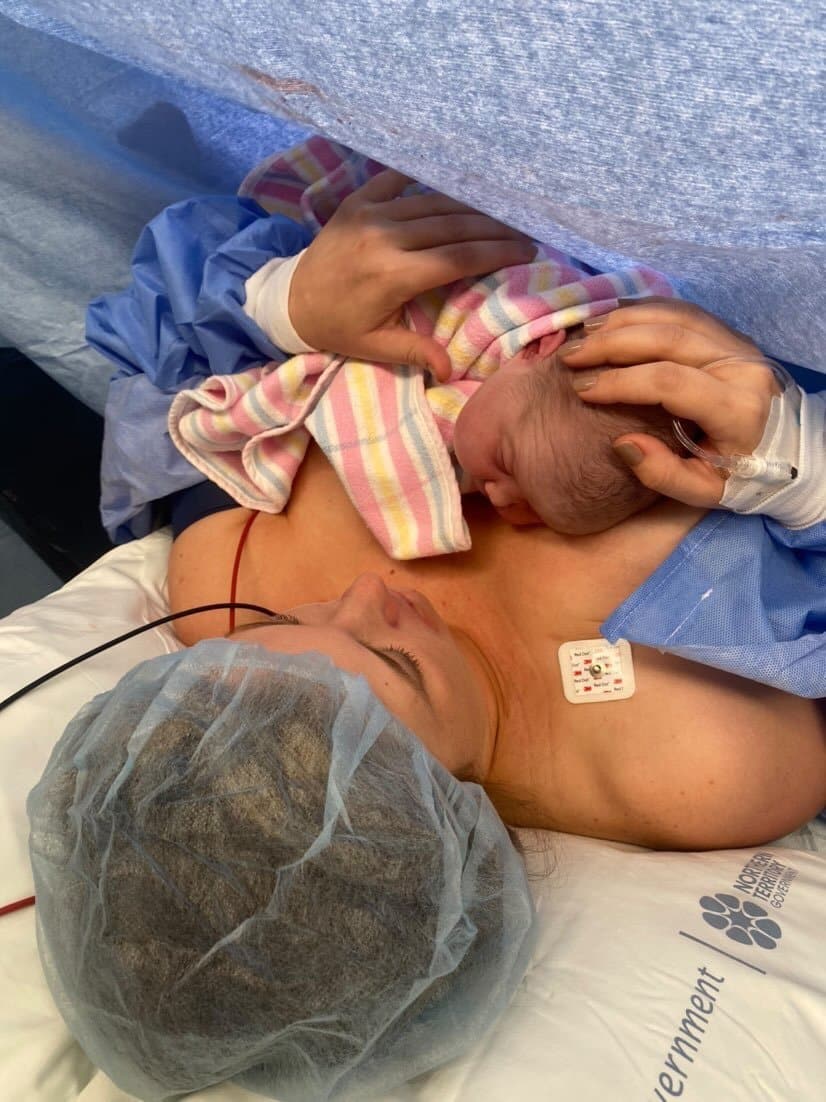
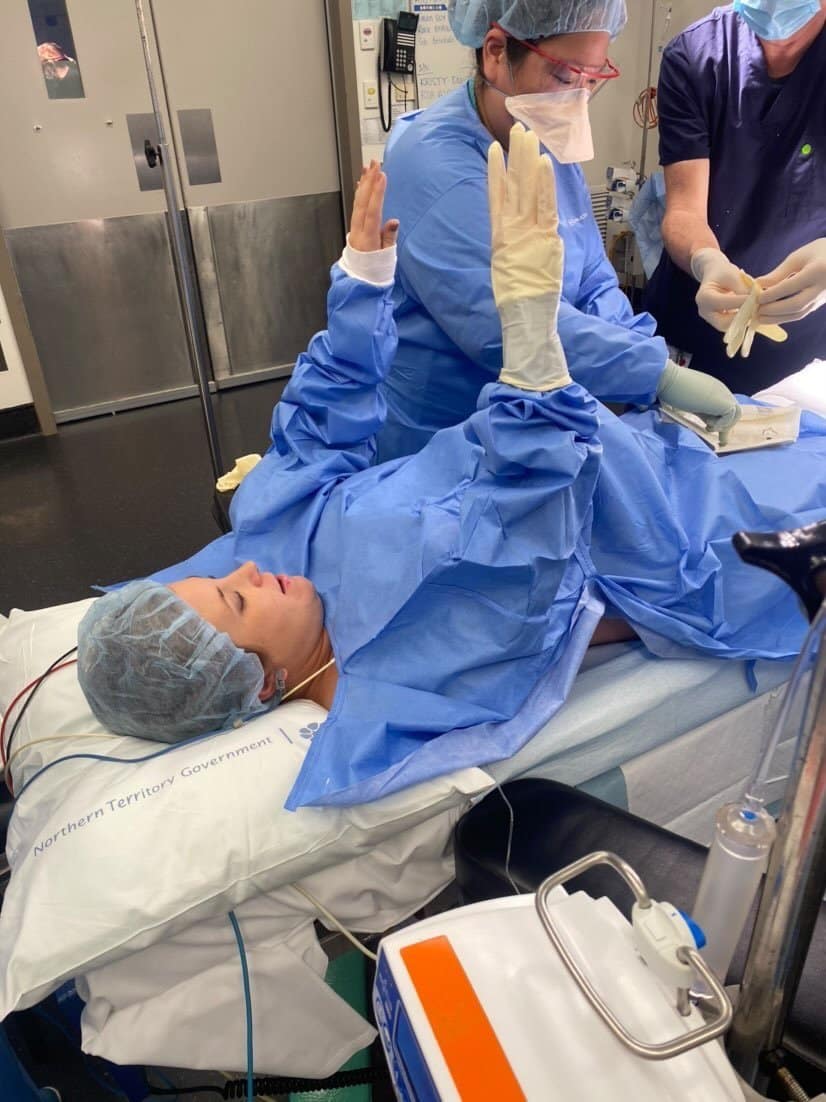
“It was the first maternally assisted emergency caesarean to be performed in the Northern Territory. I had to scrub in while laying down which was really tricky. Angus’ head was out but his shoulders were still in so my OB hooked my fingers under his armpits and I helped bring him out but it was so slippery, once his shoulders were out I brought him up and I brought him to me and had immediate skin to skin. It was the most amazing, magical experience ever.”
Topics Discussed
Three caesarean births, Maternally Assisted Caesarean, Ectopic pregnancy
Episode Sponsor
You can enjoy 15% off Mere Botanicals with the discount code ABS15.
Categories
Related Products
-
The Caesarean Birth Class
4 reviews$198.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






