Podcasts Hannah
EPISODE 147
Hannah

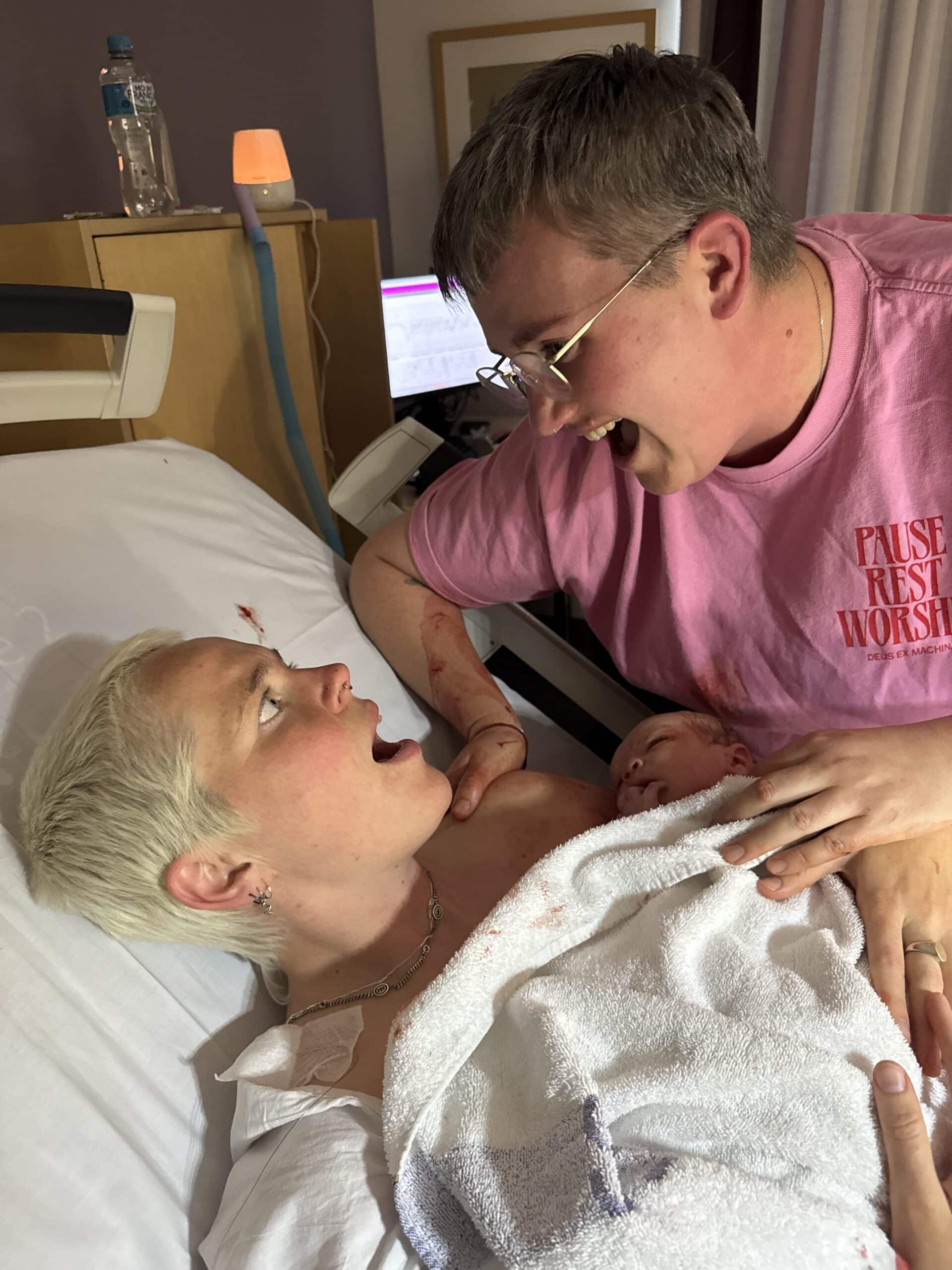
Hannah’s transition from hospital to home was a unique experience with her first son, Cliff. He had spent the first four weeks of his life in NICU and Special Care after being born at 32weeks so those first days at home were actually the very first time Hannah and husband Phil had been alone with their baby. “The day that we went home…that was the day that felt like he was born. It was the best day of my life,” she says.
Eight weeks prior she had left home with a suitcase and jumped on a plane to Bali with Phil. They had been together for a year when they unexpectedly fell pregnant, embraced the surprise and moved out of a share house and into an abode of their own. Hannah had nausea and dreadful heartburn but apart from that she was gliding through a trouble-free pregnancy. Phil planned their Balinese babymoon as a surprise and they spent the first week in a remote part of the island before heading to Seminyak to shop and eat. It was during dinner with friends that Hannah first started to experience period pain cramps that came every half an hour. She didn’t think much of it, put it down to the heat and went to bed that night to sleep it off. She was 29weeks and 4 days pregnant. The next day she woke with a sore lower back, went out to shop and when it was time to have lunch she couldn’t get comfortable enough to sit down so she went back to the villa with Phil. By evening she was in hospital; her mucous plug had come away and she was regularly contracting.
Despite her fears of the Indonesian hospital system, it’s lack of NICU facilities, the cost of her care (regardless of travel insurance) and the language barriers, she was looked after with the utmost professionalism. She consulted with a Sydney-based OB who suggested she fly to Darwin instead of Sydney as it was a much shorter and therefore less risky flight. As soon as she left the hospital to go to the airport she started bleeding and contracting again. Needless to say, the flight was very challenging. They moved quickly through immigration and Hannah made her way to the Royal Darwin Hospital where she was taken straight to Maternity. “The care was absolutely incredible and I remember a few lovely midwives who did the first internal. They were all very calm and subsequently I presumed that everything was ok. But then they said: Your membranes are bulging….your baby is so close to being born. You are so lucky you didn’t give birth on the plane.”
Hannah and Phil met with countless specialists who prepared them for the following weeks and their inevitable NICU experience. Hannah stayed in hospital for 10 more days, was given medication and pessaries to stop labour and went to the delivery suite on three different occasions with false labour, before she was sent home to their Darwin rental. “I had to go to the hospital twice a day for CTG scans but I just needed to get out for the sake of my mental health. However, on the third morning out my contractions were picking up and I felt like I was coming down with the flu…I knew there was a risk of infection. So, I listened to my intuition, told them I wasn’t leaving, had a sleepless night and the next morning when I woke they took my bloods and noticed my infection markers were rising. They agreed that the best thing to do was to induce me so on Christmas Eve, with the monsoon rain coming down horizontal outside, I was moved to the biggest birth suite on the ward, hooked up to an IV drip and given the highest dose of pitocin which caused the most intense contractions.”
She found comfort in gas but around 9am she started to struggle with the pain. The midwife did an internal, announced that she was 4cm, broke the hindwaters and immediately hit the emergency button. Hannah’s baby had fallen straight into the birth canal and was crowning and born soon after; she went from 4cm to birth in less than five minutes.
“It’s quite a silence experience and you’re just holding your breath and waiting to hear your baby cry,” she says. Cliff finally did cry and was whisked away to NICU while Hannah stayed behind to deliver the placenta. “It wasn’t in a good state at all and was obviously affected by the infection…it made me really grateful that I pushed for the induction,” she says.
Despite his low birth weight of 2kg, Cliff did surprisingly well. He only needed breathing assistance for six hours and by the end of his second day he’d been downgraded from NICU to Special Care. Hannah pumped every three hours and had a great supply and she found so much comfort in kangaroo care, an experience that she believes all NICU parents and babies should push for. “We got into a rhythm and I got really confident with skin-to-skin, kangaroo cuddles. I’d sit there for four hours at a time and I felt like he started to come alive; it was so amazing!”
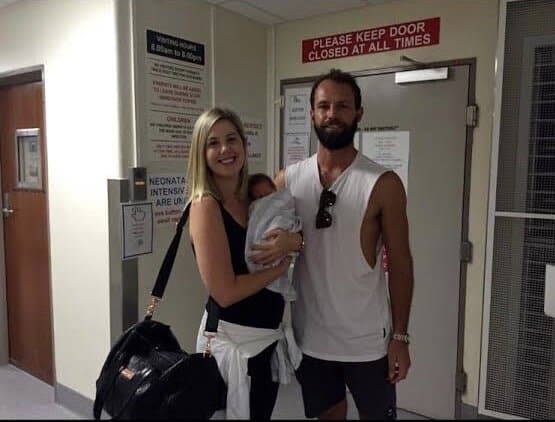
They were discharged four weeks after Cliff’s birth and despite slow weight gain, he continued to thrive. When he was 14-months-old they returned to Bali for a one-month holiday and surprisingly returned home pregnant. Hannah had a cervical suture inserted at 15weeks and was enjoying a smooth pregnancy until she started contractions at 29 weeks and 4 days – the exact same time she started labouring with Cliff. The remainder of her second pregnancy, with son Sid, was spent on strict bedrest. You can hear all the details of Hannah’s unique and intriguing story on this week’s episode.


Topics Discussed
Babymoon, Incompetent cervix, Induction, infection, NICU, Pitocin, Postpartum support, Premature labour, Vaginal tear
Connect
You can connect with Hannah at The Sleep Nurse
Episode Sponsor
Today’s episode is also brought to you by Cell Care. Be empowered and know the future potential of collecting your child’s umbilical cord blood and tissue. Rich in stem cells, there’s been 40,000 cord blood treatments for 80 approved conditions, and research is proving its potential for many new therapies. The cells are a perfect match for your child, and are more likely to be a match for siblings. Brenda’s son Brodie received cord blood cells to treat his cerebral palsy and t’s had a remarkable impact on his life. Read Brodie’s story at cellcare.com.au. The only opportunity to collect your baby’s cord blood and tissue cells is at birth. Cell Care is Australia’s largest and most experienced cord blood and tissue bank Request an info pack today – Cell Care; storing stem cells for the future.
This episode is brought to you by Zarpar Bebê. A range of Baby Carriers created to provide a beautiful, simple and ethical solution to YOU, the mindful parent on a journey through natural parenting practices. Zarpar’s passion is to create naturally inspired, yet practical products to simplify the everyday – to empower you to bravely follow your instincts. Neutral tones and textures to suit all stages of your journey from birth to toddlerhood. Zarpar wants to allow you the freedom to explore and connect to the world by simply experiencing life together. Through thoughtful sourcing they ensure fair wages and clean and safe working conditions for their makers. They are committed to using pure and simple fabrics which have been sustainably sourced respecting animals and the environment. By working with rural communities in Nepal and Indonesia, they help to strengthen the livelihoods of marginalized families. The Zarpar baby carriers not only support natural parenting, but also enrich the lives of their makers by building futures and changing lives.
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us