EPISODE 436
Dom | Postpartum – birthing on country model of care, waterbirth

It’s so important to remove the stigma associated with perinatal mental health, medication and psychiatric hospital wards because they support countless new parents every year in Australia. While there are public hospitals offering parent + baby psychiatric care, if you have private health insurance and want to access a private hospital, the Australian Government allows you to upgrade your hospital cover for psychiatric care without a further waiting period; just call your health fund to request it.
“I had a water birth with my first baby and birthed him through an Indigenous model of care called Birthing in Our Community and they supported me right through pregnancy and beyond. I had no idea the programme existed but they have a group of midwives, family support workers and other allied health professionals services.
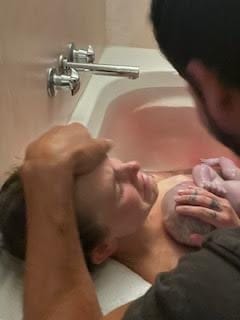
“I was 39+3 when I noticed some mild contractions so I put the TENS machine on and cruised through early labour. It intensified pretty quickly so we drove to hospital and once I got to hospital my midwife ran the bath and Mannix was born soon after. We did delayed cord clamping and he fed straight away. I wanted to be discharged within three hours but he had meconium stained waters so I had to stay a bit longer. I have memory loss around the first few weeks but my husband told me that the midwife came to visit us at home and Mannix was breastfeeding and sleeping really well.
“Throughout my life I’ve had zero mental health issues; in my pregnancy I was just really happy. In my work as a paramedic where I witnessed some really terrible things but it never affected my mental health. After Mannix was born my husband had five weeks off work and my family noticed my mood changes about a week after that. I went to my GP and talked about my anxiety and they brushed it off as mum-guilt. Knowing myself I may have downgraded my symptoms because I don’t like people worrying about me and with a medical background I tend to take care of myself. It spiralled out of control after that. It was like I’d run into a concrete wall.
“We had a baby monitor and even though Mannix was in the room next to us and we knew he was asleep and well, I couldn’t help but constantly look at it. I was sitting up at night with my eyes locked on it for hours and hours and hours. I couldn’t sleep and I was anxious about his sleep. If I put him down for a sleep I’d watch the clock, really aware of the 45 minute sleep cycle. I worried that if he woke up I wouldn’t know what to do; would I pick him up? Do I feed him, rock him? Am I creating bad habits? It tore me to shreds inside and I was just full of anxious thoughts. My family saw it from early on and because I’m a bit of a perfectionist, I wanted to do a really good job of being a mum. I see it now as a competitive thing, especially in relation to my four older sisters having multiple children each and I think I wanted to be seen as doing a really good job and being the best; I wanted my baby sleeping through the night at an early age, I just had really unrealistic expectations and it was really detrimental to my mental health.
“My mum wrote a journal for me because I ended up having electroconvulsive therapy (ECT) and one of the side-effects is memory loss. She got up to 300 pages – from the day I called her to tell her I wasn’t well to the day I was discharged from hospital, she wrote down everything from every day in a journal. I’ve read it a few times and it still makes me cry, for everything I went through and everything my family experienced, too.
“My first red flag was a panic attack; it was the first one I’d ever had. I called my mum and I told her I was sitting in the corner of my room rocking back and forth. I moved outside and looked up to the sky and thought I was going to die; I couldn’t control my breathing or my thoughts, I was pulling out my hair and I thought there was something seriously wrong with me. I called PANDA and while I was on the phone to them my mum couldn’t get through and thought I’d committed suicide. I eventually called her back and she told me to pack my things and come straight to her house which was about an hour away.
“I packed everything up and drove to my mums and I don’t have any recollection of this but I handed Mannix over to one of my sisters and just cried in my other sister’s arms. My mum thought it would be good for my mental health to be surrounded by family; she knew it wouldn’t fix me but it would be the support I needed. But it wasn’t enough.
“I deteriorated to the point where I was psychotic; I was rocking back and forth on the kitchen floor, pulling out my hair, I couldn’t stop the thoughts of: I’m a terrible mother, my son’s not sleeping enough, he’s not thriving, I can’t do this. The whole time I thought I didn’t want to be here anymore, my husband and son deserve better and if I get up and walk out of this house I won’t be coming back.
“My husband and mum took me to emergency at my local hospital and I was put in a secure room on the mental health ward. I had to wait for a doctor to assess me and while I was there I just kept wondering why I was putting my son through this. The door locked from the outside, there was a board of wood over the window where glass used to be and there were cameras in the room. I just kept thinking that the room was making me worse. The doctor assessing me thought I was safe enough to go home to my family and the next day the outpatient mental health team came to visit me at home. The next day I deteriorated again and was admitted to the short-stay mental health unit but they didn’t think it was the best place for me.
“Mannix was only 7 weeks old and I was still breastfeeding. There are two mother + baby units in Queensland and I had private health insurance so I could access the Brisbane Centre for Postnatal Disorders (BCPND) at Belmont Private Hospital. I admitted myself there and while I took medication which would initially work, the anxiety would just come back again.
“Mannix came with me and he had his own room and was sleeping well. I was doing therapy sessions with my psychiatrist and the unit nurses and everything was getting better. Mannix was moved from his own room to the open nursery and he was being woken regularly and that’s when my anxiety peaked again. I spiralled and my anxiety, guilt and depression sent me into a relapse.
“It’s written in the journal that I handed Mannix to one of the nurses, told her to give him to Daniel and said I couldn’t do it anymore and I was going to leave. She understood that to mean I wanted to commit suicide and that’s obviously what was going through my mind at the time. She had no other choice but to put me onto a secure ward – it’s locked up and you aren’t allowed your baby in there. I couldn’t control my emotions and I was so heightened; I punched the wall and I fractured my knuckle. I didn’t let anyone assess me so I went for a day with a swollen hand so I was taken from Belmont secure ward to another hospital with an orthopaedic ward. I don’t remember any of this.
“I was on the secure ward for a week and did ECT therapy under the emergency act; I was so sick that I couldn’t agree to or deny it. The hospital sought my family’s permission but when I speak to my mum now she’s still not a fan of it. ECT is where they put electric leads on you which send your brain into a seizure; it’s supposed to create new pathways in your brain and forget about short-term memories. It’s not a nice thing to witness but I don’t think I’d be here if it wasn’t for that. From my family’s point of view, it was traumatic to say the least, to give consent and also wonder how it would affect me for the long term. My family were advised to watch videos of the procedure and to really understand the benefits and the risks before they gave consent. They not only had to force me to do it but they could also see the implications of it. I had 16 sessions of ECT and that’s quite a high number; 16 to fix me.
“I’ve got a memory lapse from Mannix’s birth to 12 months; I don’t remember much at all. That could be a combination of the ECT, the drugs I was on and my experience of postnatal mental illness. When I was in the secure ward I unfriended my mum and my husband because I said they were killing me because they were forcing me to stay in the secure ward and how dare they take my son away from me. The medical team agreed that being in the secure ward was making me worse so with everyone’s support I was discharged home and I was there for a week. I had another episode where I felt like I needed to leave and get away and I was readmitted to the hospital again. All up I was there for three months and Mannix was with me and I think it was good for him; he was also cared for by the nurses, there were other babies there and he received so much attention and socialising and adapted really well.
“Mannix was only separated from me when I was in the secure ward for one week. The rest of the time he was with me in the mother and baby unit and it was just like I was at home; I fed him, changed him, bathed him and did it all. When I was having ECT the nurse or my family would care for him. When I was in the secure unit I was still pumping so Madix was with my husband that week and he was mixed fed with a bottle.
“They help prepare you for returning to home and your baby is your responsibility but if you’re having a bad day and in the early stages, overnight feeds are considered a hindrance because it interrupts your sleep so the nurses would do those feeds. In the later stages of my admission, I got up in the night to do those feeds. I sometimes look at my postpartum and recognise that I didn’t have a traumatic birth and my baby was really settled and fed and slept well, I don’t know why I was so anxious. I couldn’t think of a trigger for it which only compounded my anxiety.
“I formed a really tight bond with the other mums there and we’ve still got a connection. I don’t know their faces very well because I’ve got that memory block but it’s still good to chat because we’ve been on similar paths. When I got discharged I was still seeing my psychiatrist monthly and I was still on medication. My husband was my rock and it’s hard to express my gratitude for how he supported me throughout the whole experience. With the support of my psychiatrist I weaned off my medications at 11 months postpartum and didn’t have any mental health concerns at all.
“I was quite nervous to have another baby because I was at a high-risk of developing a postpartum mental health issue again. With my second baby I had more realistic expectations and I saw my psychologist regularly. I also had a close relationship with my midwife and she checked in with me throughout my pregnancy. In postpartum with Queen I haven’t even had the baby blues; there was no dip in my mood at all. I’m three months postpartum now and I’ve had so much support. I’m so passionate about sharing my experience and hopefully comforting another mum who’s going through it.”

Topics Discussed
birthing on country model of care, ECT, Indigenous, mother + baby unit, PAD, panic attacks, psychiatric unit, Waterbirth
Episode Sponsor
Today’s episode is brought to you by Kiwi.co.
I must confess I’m not much of a crafty mum but Kiwi Co’s panda crate has been the best educational investment for Ottie. Every month we receive a subscription box filled with playful, open-ended activities backed by research and designed especially for naturally curious and creative babies and toddlers. It makes the perfect Christmas gift that keeps giving well beyond the festive season.
I’m a big fan of quality activities that create the opportunity for play-based learning and Kiwi Co delivers hands-on projects that get the whole family involved. Whether you have a brand-new baby or a trailblazing toddler, the Panda Crate is perfect for your little one’s developing brain.
Unwrap more than a gift. Discover hands-on fun with KiwiCo.
Get your first month FREE on ANY crate line at kiwico.com/birthstories
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






