EPISODE 348
Sarah’s pregnancy and Breast Cancer journey

“I started doing ovulation tracking with the kits from the supermarket and we fell within the next month. Unfortunately we lost that pregnancy; it was a missed miscarriage. It definitely rocked us…we came home from the ultrasound and it was like the world had just gone black and white, it was just so sad. I had a D+C and I had to wait a month to fall pregnant again and that was when I fell pregnant with my daughter Audrey. A little part of me was hoping that I’d get to the next milestone, the miscarriage prompted me to feel lots of anxiety. After a miscarriage it can be really tough.
“I would have loved a waterbirth but I needed to be induced at 41+6. They broke my waters and then hooked me up to the syntocinon drip. I tried gas + air but it made me feel drunk and I really didn’t like it. I asked for an epidural and luckily the anaesthetist was just outside the door so I got it straight away. The obstetrician came in because Audrey was distressed and she suggested a forceps birth and I actually needed two episiotomies. When she was born she was really pink and let out a really loud cry and I immediately felt a wave of relief. She scored a 9 on her first APGAR and then she started grunting and they took her straight to NICU. I got stitched up and showered and I had my mum with me. Josh was with Audrey and she was on the CPAP machine. We were told that her lungs had collapsed and they would heal on their own. I can’t speak more highly of the NICU team, we were so lucky that we birthed there.
“After 48 hours she came off the CPAP machine and then she was monitored for another three days before she was discharged. Because she’d had a syphoning of the lungs, a lactation consultant told me that breastfeeding may be a bit challenging. I wasn’t offered any support for my pelvic floor recovery and apart from the episiotomies and the fear that it would make sex uncomfortable, I didn’t have any symptoms.
‘We had a tricky time conceiving Pearl and I went through secondary infertility. All the mums in my mother’s group were moving onto their next pregnancies and nothing was happening for us. I had a few investigative procedures and I got back really good results which was lucky. I realised that I was ovulating on about day 20 but we’d always started trying on day 14. Infertility is a sad and lonely journey, especially when everyone around you is having babies.
“Pearl’s pregnancy was a wonderful and lovely pregnancy. I elected to have a caesarean after my first traumatic birth. The trauma came back as soon as I was pregnant again and I felt the birth looming. I wanted to avoid all the unknown, because I felt like I was taking more control by having a caesarean.
“At the 28 week mark I got out of the shower and I put stretch mark cream on my belly and breasts and I immediately felt a lump on my breast. It felt as big as a grape but it was long and an odd shape. I booked into the first doctor I could get into and she was lovely. She was very reassuring but she sent me for an ultrasound and she encouraged me to go as quickly as possible. On the day I had the ultrasound the lady who was doing it had a trainee with her but they didn’t speak the entire time. The doctor came in and he didn’t sugarcoat it at all. He told me it didn’t look good and he was going to do two breast core biopsies that day. Straightaway I knew it was serious. I went to the doctor a few days later and I was told it was a stage 3 invasive ductal carcinoma.
“It felt like life and death; I was growing a baby and growing cancer. There are a huge number of women who are diagnosed in pregnancy or while breastfeeding. My cancer is triple positive cancer and it feeds on hormones so being pregnant makes it grow faster and more aggressively.
“I have a fantastic oncologist and he agreed to remove the tumour first. I was terrified, I felt like the captain of a sinking ship, because I was so conflicted about Pearl’s wellbeing. During the operation there was someone taking care of Pearl because the general anaesthetic does cross the placenta. I woke up in recovery and felt her kicking and it was the greatest sense of relief I’ve ever felt.
“They couldn’t do a mammogram or an x-ray because I was pregnant but all the cells around the tumour that they took out weren’t cancerous which was the best possible outcome. The lymph nodes were also clear. The chemotherapy was like a good insurance policy and we planned to start it a few days after the birth and so a vaginal birth allowed me to recover much quicker. But Pearl kept flipping from breech to head-down and I knew that a caesarean would push the chemotherapy back a week. I was scheduled for an induction but once I was in there Pearl went tachycardic and they immediately took me to theatre for a caesarean. It was a wonderful atmosphere; it felt like they were having a party. It was really lovely, such a nice experience.
“Pearl had to go to the NICU because she was only 35 weeks and then I felt the shift; I had one week recovery and then I started chemotherapy. I didn’t have good veins for chemotherapy so I had a portacath put in three days after Pearl was born.
“I had expressed colostrum before Pearl was born and then afterwards I was given some drugs to suppress my milk. I’m now halfway through my six rounds of chemo. The first round was really tough but the second session was much better in terms of the side effects and nausea. My hair has fallen out and my husband shaved my head and to be honest it was quite a lot of fun.
“I will probably have to do radiation therapy after the chemo and then I’ll have to go on hormone therapy because my cancer is hormone driven…it means I’ll go through early menopause. It’s hard but I’m grateful to live in Australia where everything is available. Once I have genetic testing that’s when the discussions around a mastectomy and hysterectomy will begin.”
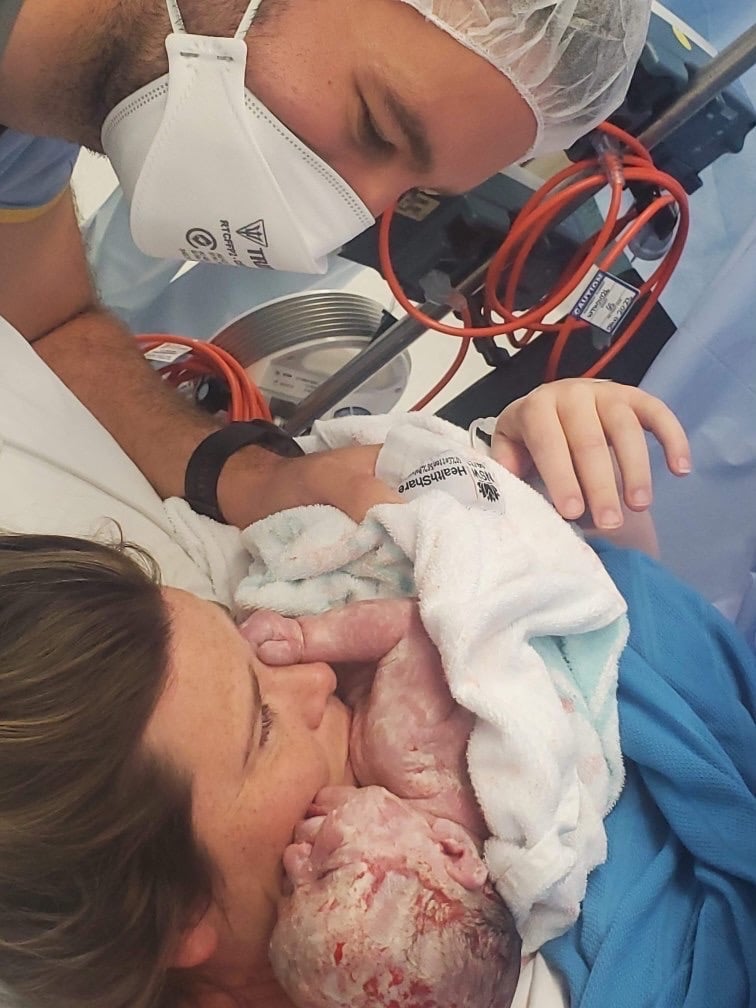
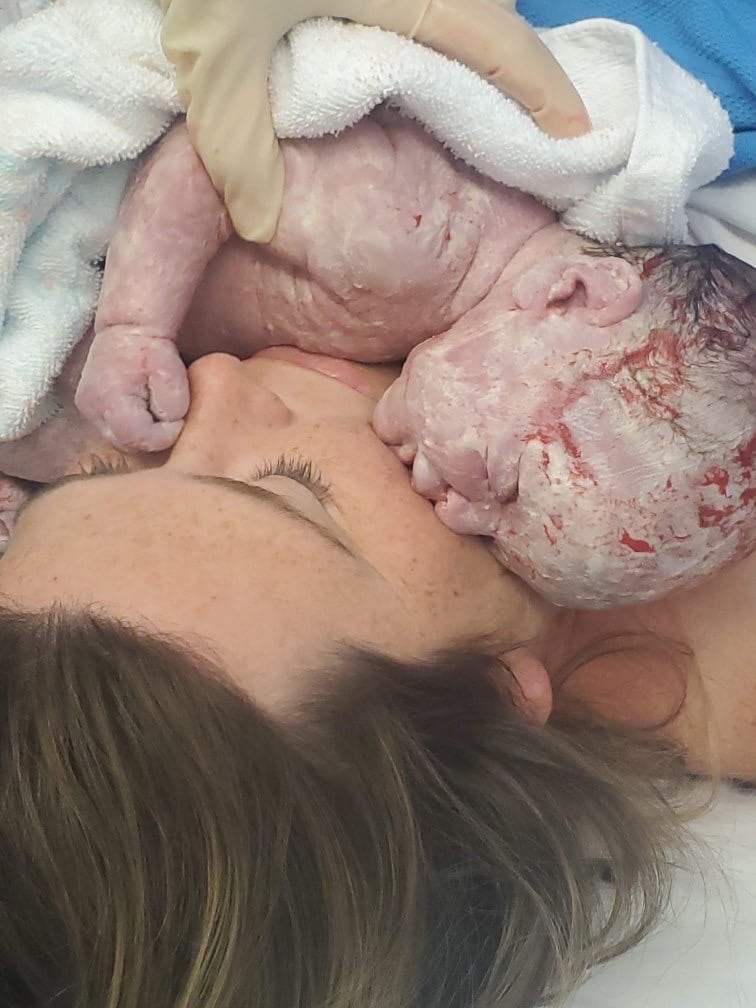
Topics Discussed
Breast cancer, Two births, Caesarean birth, Secondary infertility, Missed miscarriage, Induction, Forceps, Episiotomy
Episode Sponsor
Today’s episode is brought to you by the KiwiCo Panda Crate.
The Kiwico Panda Crate is designed just for infants and toddlers, Panda Crate is grounded in the study of early childhood development in a way that’s made helpful, practical and convenient for parents. Every crate comes with a magazine and activity cards featuring research-backed content and activities to nurture your little ones.
All shipped right to your door. And there’s no commitment, so you can pause or cancel anytime.
Give the gift of brain-building play and create a foundation for learning with Panda Crate from KiwiCo.
Get your first month FREE plus free shipping at kiwico.com/birthstories
Categories
Related Products
-
The Caesarean Birth Class
4 reviews$198.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






