EPISODE 340
Cammie

“I was in such denial that I was pregnant but two lines popped up on the test and that was Archie. In the US, when you have a good health insurance policy it covers quite a bit of everything so I was interested to hear that my private health insurance only covered my hospital stay and not my private obstetrician. We went to our local public hospital to have a look around and then we opted for Cabrini Private Hospital, mostly because we don’t have family support here and the extra nights in hospital after birth was something we wanted.
“We did a little bit of research and it was an okay experience, but if I was to go private again I would do it a bit differently. It was a smooth and uncomplicated pregnancy apart from three weeks of intense nausea in my first trimester. We did an all-day workshop with the hospital but I was also keen to have a low-intervention birth so I watched a lot of youtube videos and I read Juju Sundin’s Birth Skills.
“At 39 weeks I had an appointment with my obstetrician and my blood pressure was a bit elevated. I had no other symptoms but she sent me to get bloods and a CTG and she scheduled me for an induction at 39+4 because of the potential for a preeclampsia diagnosis and my baby was measuring a bit big. I wasn’t too worried as we grow big babies in my family. I felt really discouraged when she suggested an induction but I was reassured by the CTG and the blood results. I told her that I didn’t want to be induced at 39+4 and she accepted that. I felt some tension but I also felt good about how I was advocating for myself although I very much felt like I was on the clock.
“I walked away from that appointment and embraced all the natural induction techniques – walking, spicy food, sex. I woke up at 40+4 with back pain that was coming in waves but I wasn’t getting any cramping in my front. I was tentatively booked in for an induction that evening so I had an appointment that day and my obstetrician checked me and I was 2cm at that stage which made me feel a lot better about an induction. I was admitted that evening and they told me that my obstetrician would come in at 7:30pm to put the cervical gel in but unbeknownst to me, my waters broke when the gel was in. I just thought it was the gel that was coming out of me because there was no gush. You have to lie down for that first hour after the gel is administered and my back was aching and when I could get up I got on the fitball. They checked my pad and the second midwife confirmed that it was my waters and that I was in labour.
“The first time I was meeting the midwives was when I was in labour so I didn’t have any rapport with them…it was disappointing. I felt like I connected with the second midwife because she was aware of what I was experiencing instead of just going off the induction plan. My back pain was really ramping up, I never experienced any contractions in my front, they were all in my back and it was excruciating. The midwives were asking me about what I wanted from pain management which was disappointing because they weren’t suggesting alternative positions, I felt like everything I’d prepared for was going out the window.
“I had a bag of tools for labour but it sat in the corner of the room the whole time. In hindsight, I wish I had communicated more with my husband about what I needed from him. I couldn’t believe how quickly I became non-verbal apart from really loud moans and they were moans of fear, not labour progression. The gas and air didn’t work for me at all. There were a lot of babies being born that night and because they hadn’t anticipated for me to be in labour, there wasn’t much midwifery support.
“I realised very quickly that I wasn’t coping and I asked for an epidural. And I knew it was the beginning of the cascade of intervention. The contractions were one on top of another. Once the epidural was in I couldn’t feel my legs but I still had back pain so I couldn’t sleep and I moaned through the night. An obstetrician checked me through the night and I was still 3cm. I asked if I could lay on my side but the midwife told me that because I had the epidural I had to be on my back which I know isn’t correct. Then at 6am another midwife came in to see how I was and after I explained my back pain she put me on my side and used a peanut ball to relieve pressure and it was amazing. It took two midwives to turn me because I couldn’t move my legs and once I was on my side the pain went away immediately.
“I pushed for about an hour and the obstetrician was concerned that I was going to have a severe tear so she gave me an episiotomy and she used the vacuum and he was out within moments. He came out crying and was pink straight away and he was on my chest for 15 minutes before the paediatrician had a look at him. He was then on me for another hour before I had a shower and we moved to the postnatal ward.
“My recovery was overshadowed by some of Archie’s health issues. On day two I noticed his right arm was twitchy and the next day it was getting a bit compulsive and his head was bobbing so our midwife told the paediatrician and she was in our room within 30 minutes. She recognised that it was neurological and she used the word seizure and she ordered a cranial ultrasound. It was devastating to get this information and within an hour he was getting an ultrasound but it was inconclusive so we were sent to the Mercy Hospital via ambulance. I can’t say enough about the team there, one of the paediatricians said that perhaps Archie had had a stroke during birth and there was something reassuring about what he was saying. The statistic is that 60% of babies who have a stroke just move past their systems. He had to have brain monitoring and I was connected with a lactation consultant who helped me pump as we weren’t able to hold him for 24 hours. After an EEG he wasn’t showing signs of more seizures, the anti-seizure medication had worked and he moved to special care while we waited for an MRI. The test results confirmed that he had a stroke a few moments after birth so we did one more night at the Mercy and then we were discharged.
“In January 2021 we decided to start trying for a baby and we fell pregnant a few months later. I had a dating scan and there was no heartbeat and the baby was measuring at 6 weeks. I knew it wasn’t going to be a viable pregnancy so a few days later I saw my GP and had the blood test to show my hCG levels and they weren’t rising so I’d had a missed miscarriage. My anxiety was through the roof and I was having panic attacks so I went to the public hospital to have a D+C. However my hCG levels had gone up and even though another ultrasound still showed no heartbeat and an embryo measuring at 6 weeks, they couldn’t give me a D+C so they told me to come back in a week for another ultrasound. It was so disheartening. A week and a half went by and my body wasn’t showing any signs of miscarrying naturally so I went back into the hospital and had the D+C and luckily I recovered from that really easily.
“I was seeing a therapist for my anxiety and panic attacks and together we decided to go on medication and one that was suitable for pregnancy and it has been a really good choice. We waited a few months before trying again because I wanted to recover mentally, and physically.
“I fell pregnant easily with Flora. At 22 weeks I had a telehealth appointment with an obstetrician from the Royal Women’s Hospital. There was a bit of confusion about where I was going to birth and it ended up that my BMI was 1.5 points too high for me to give birth at my small, local hospital. It created a lot of stress and I really struggled because I’m a fit and healthy individual – I exercise and I eat well but I have a large frame. This is who I am. It was really hard to learn that because my body is larger, I couldn’t birth at the hospital I wanted to be at. I was devastated. I called Sandringam hospital to talk it through and I spoke to a lovely midwife who explained that it was the anaesthetist that sets the BMI recommendation which was frustrating because I knew I wanted a low-intervention birth.
“It was even hard for me to access my care at the tertiary hospital because I wasn’t able to bring Archie to appointments so I didn’t end up seeing any midwife or obstetrician in person till I was 30 weeks. I began to explore the potential of a homebirth but my husband was a bit apprehensive and yet he admitted that I wasn’t receiving any care anyway so it couldn’t hurt. At 28 weeks I called MAMA Services and they had a gap in their schedule for my due date in April. They do use BMI but they’re cut off was five points higher than the hospital and the midwife told me that my BMI was not going to be a problem. The next week I met with my midwife and it was a 90 minute appointment where they took all my history and embraced Archie’s presence at the appointment. I had a couple of appointments at home which was great and I was working with my psychologist to work through my anxieties and fears. I had a fear of haemorrhaging because my obstetrician had mentioned that I needed a syntocinon injection because she was concerned about my bleeding after I birthed Archie so my midwives encouraged me to access my birth notes from Cabrini hospital and they showed that I only bled 300ml which is less than average. Once I had that information I was really reassured.
“Flora turned breech at around 36 weeks. I was at the Royal Women’s Hospital for my final appointment with them and the midwife discovered that she was breech. I immediately downloaded spinning babies and the next day I knew she had turned, I knew she was head down. I cut ties with the Royal Women’s and then only saw MAMA services from then on.
“I began having contractions on a Wednesday evening and they were so much better than back labour. My waters broke (it was later confirmed it was probably my hind waters) – there wasn’t a lot of fluid, but it prompted me to go to bed and get some rest. I was in there for 30 minutes and in that time there was another gush and I hopped into bed with my sister who started timing them and they were five minutes apart. My husband and sister started setting up the birth space and one of the midwives from MAMA services arrived and she did my vitals and my blood pressure was high. She encouraged me to get into bed and relax for an hour and I was trying to meditate and relax. My blood pressure did go down but my labour fizzled out and completely stopped. The next day a midwife came out to see me and my blood pressure was taken and it was up again. If it stayed high and kept going up I knew I would have to birth at The Royal Women’s. I had to go in for them to rule out preeclampsia and an obstetrician came in (I’d kept a history of my readings on my phone) and she could see it was a bit elevated but she wasn’t concerned. I had asked her if she could check me and give me a sweep, mainly because she mentioned a possible induction if my blood pressure kept going up. She did observe that Flora wasn’t engaged, too.
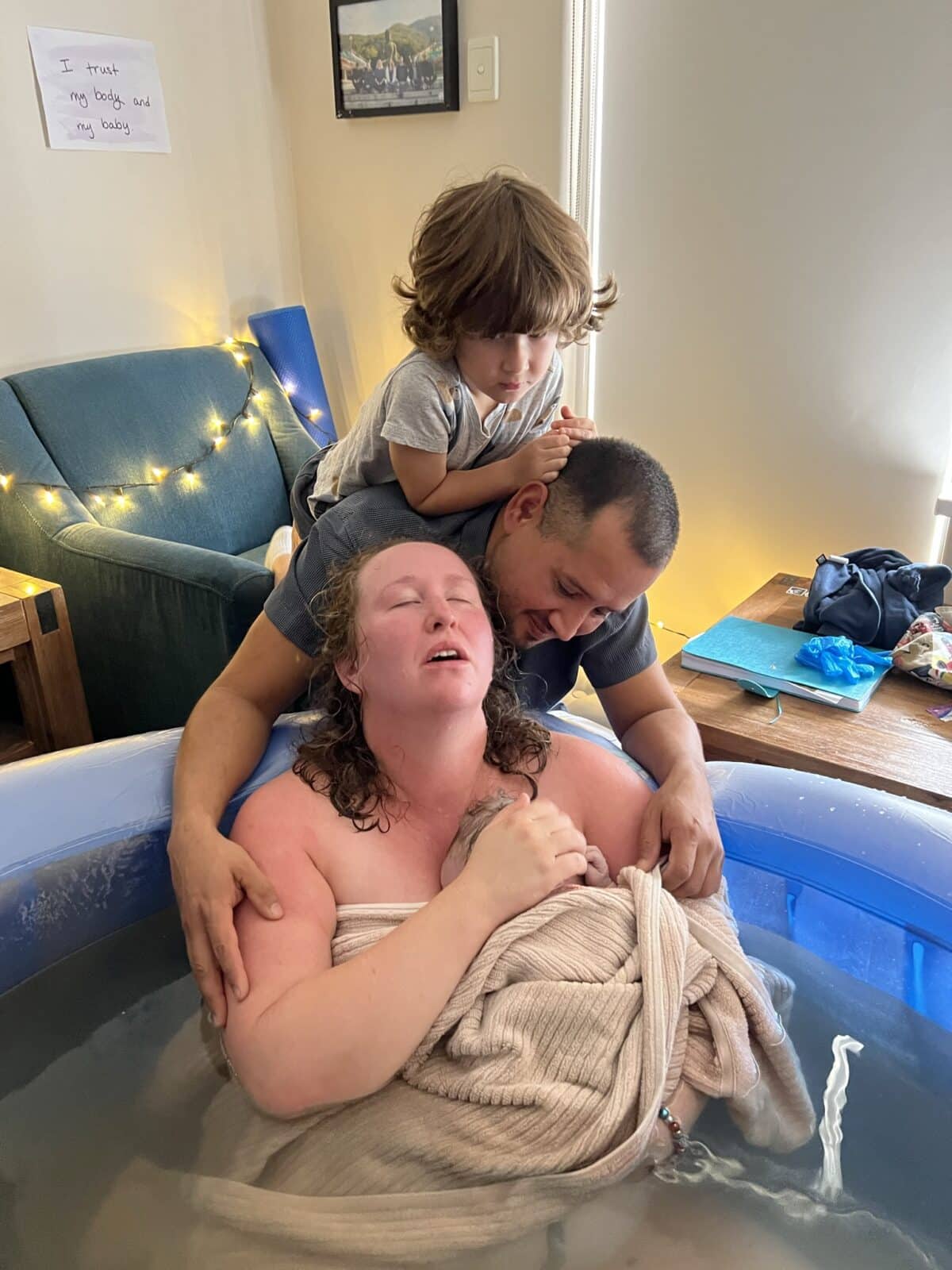
“We went home that night and the next morning I did everything I could to get Flora into a good position. We went to the playground and I started having contractions and they were strong. We got home and the contractions were regular and intense; I was doing horse breath and sniffing my clary sage essential oil and I felt good, I felt like I could do it for hours. I felt like I was in active labour from about 12:30pm. I put the TENS machine on soon after and the midwife arrived and at about 2:30pm they started filling up the pool. I was starting to moan towards the end of the contractions and within 15 minutes of being in the pool I was transitioning and it got really intense and it felt like it was constant but looking back on my birth video I could see that there was breaks in between contractions where I really internalised. Then I felt the first urge to push and it was amazing. I pushed for twenty minutes and I felt my waters burst and right after that I could feel her head. My midwives encouraged me to slowly breathe her out and then finally her head came out and when her body was born I lifted her onto my chest. I had a physiological third stage and within 10 minutes of Flora being born I had the urge to push and I birthed the placenta in the pool.”

Topics Discussed
BMI, Epidural, High blood pressure, homebirth, Induction, Missed miscarriage, Private midwife, Private obstetrician, stroke, Two Vaginal Births, Vacuum
Episode Sponsor
Today’s episode is brought to you by the Australian Birth Stories 10 Million Downloads sale.
You can enjoy 15% off all the Australian Birth Stories products with the code: 10million
This offer is valid for 7 days. Head to australianbirthstories.com/shop
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






