EPISODE 312
Andrea

“The decision of who to carry the pregnancy just wasn’t something we needed to talk about because we always knew it was going to be me. I had that biological urge to carry and birth a baby. I did lots of preparation to get my mind and body in the right place and we did two rounds of IUI before we went to IVF. We switched to a smaller clinic – City Fertility – and I can’t sing their praises highly enough. They really do care about you as a person through the process. You need them to have your best interests at heart, especially considering that it’s such an emotional journey and it’s also a very commercial setting.”
Andrea and her partner, Emma, chose an Australian anonymous donor who was recruited through their fertility clinic. She admits that it’s an interesting process (you don’t get as much information as you would presume) and she ultimately wanted to find a donor that sounded like someone she would get along with. A clean medical history was also important.
“Even when you’re socially infertile, without health concerns and age wasn’t a factor, IVF was still an incredibly stressful process. On the second round we got two embryos and they are now our two children.
“I had spotting on and off with Leo through the whole first trimester and it was so exhausting. I was at the Mercy Hospital and they did a couple of scans and no one could find a reason for the bleeding. It was a pale, peachy pink colour; it was definitely in the red category. Any amount of blood in pregnancy is scary. I had the last episode about 14 weeks but I was on tenterhooks for the remainder of my pregnancy. I have anxiety anyway and so from an anxiety perspective the spotting wasn’t the best way to start the pregnancy.
“I became preoccupied with monitoring his movements in the third trimester and it became an overwhelming situation where I was up and down to the fetal monitoring unit two or three times a week. Even though I was concerned, I balked at their suggestion that they should get the baby out early. In the last few weeks I was so debilitated by the anxiety, I was just trying to keep him alive and get to 40 weeks but it was a day-by-day operation just to keep it together. Emma’s been really good at bringing me back to earth but when you’re the pregnant person, it’s wholly your responsibility to listen to your body and pick up when something isn’t right and I really felt the huge weight of that.
“I saw the same three or four midwives over and over throughout my pregnancy but in labour I met my midwives for the first time. It didn’t really matter anyway because it’s not as if I was really aware of who was in the room and it went so quickly.
“I was induced at 40+2 and they decided to induce me with prostaglandin, the cervical gel. We arrived in the morning, they applied the cervical gel once in the morning, then in the afternoon and again in the evening. I’ve since learnt that they don’t usually apply it three times. I was having what they call ‘prostin pains’ and regardless of what I did, I just couldn’t get comfortable. I was really worried about not being able to sleep because I hadn’t really slept the night before. The midwife offered me either panadol or morphine; there was nothing between those two medications. No one actually told me that through the night I was actually in early labour. By 4am I couldn’t really sit down and as I was getting off the bed my waters broke.
“I have to speak so highly of student midwives. This student was so great, she was a little ray of sunshine, honestly I wish I knew her name because she was so wonderful. The contractions were getting to the point where I couldn’t talk through them and both Emma and the midwives were quite concerned about how I was coping considering I was so early in the labour.
“I only used the TENS machine for thirty minutes before I had to stop because they couldn’t get a good reading of his heart rate on the CTG and they needed to use a clip, and I couldn’t use the TENS machine with the clip on. I was in so much pain and I cried when the obstetrician told me I was only 2cm. You go naught to red with an induction anyway; that’s the anecdotal evidence. I laboured for another 40 minutes as the contractions just went up and up and up.
“The midwife checked me and I was fully dilated. I’d gone from 2 to 10cm in 40 minutes and she’d really watched me and knew things had shifted. She said: go for it, start pushing. I flipped over so I was hanging over the back of the bed which is such a great position for birthing; I was on all fours, I had something to grab onto, the midwives can see everything, it’s soft on your knees. I wasn’t pushing as effectively as I could have been. It was naive on my behalf that I wrote on my birth plan that I didn’t want to be coached to push. The midwife put her hand where I needed to push into and then five or six minutes later he was born.
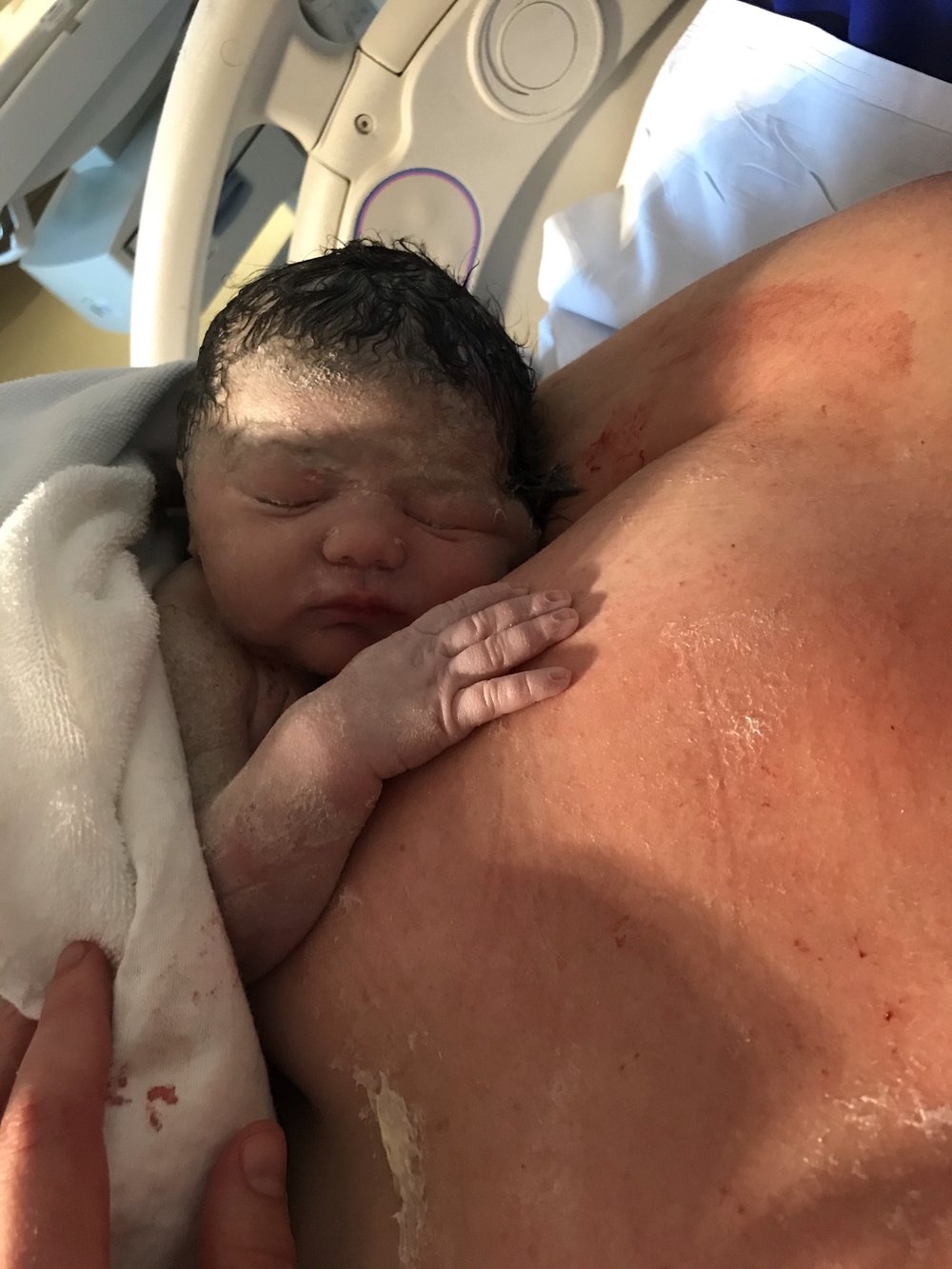
“I was in a lot of shock and I was shaking. You have these visions of how you’re supposed to be; it later upset me that I didn’t cry, I just remember they put him on my chest and I thought oh my god there’s been a baby in there the whole time. He was squealing like a piglet, super healthy and super gorgeous. On some levels it took me a little bit longer to bond with him, it was a layering and deep knowing and it always takes time to get to know someone. That shocked and interested me and it renewed my absolute awe of women in general. Anyone who births, it’s an incredible feat and mental game and it’s such a powerful, transformative thing.”
Andrea talks at length about postpartum anxiety, the intrusive thoughts she was having and the fact that her worry got in her way of her enjoyment in some way. When Leo was 15-months-old Andrea and Emma decided to try for another baby as they weren’t sure how long it would take. They had one frozen embryo from the same cycle and they said to each other on the drive to the clinic: “Wouldn’t this be amazing if it worked.
“We did the transfer, the embryo looked great, and on the way home I looked at the photo of the embryo and I said Oh that’s a girl. And she was a girl. I had shocking morning sickness from about five till fifteen weeks. I got into a group midwifery programme at Box Hill and all the midwives were amazing and I felt like our care was generally more inclusive. They were more contemporary in their culture.
“In Dacry’s pregnancy I listened to The Birth Class and it was so fantastic and filled in some major gaps in my knowledge. It was a good refresher and it also made me so much more aware, so thank you for making it. I still had my concerns over her movements and I think that confirmed that it was my anxiety. I was up at the foetal monitoring unit a lot in the third trimester and while the hospital didn’t have concerns over IVF being a reason for induction, she was measuring quite large and considering my mental health, we opted for induction at 38 weeks. I chose the balloon catheter but it didn’t really kickstart labour for me. It fell out the following morning so it obviously did something but being 2-3cm wasn’t particularly progressing as I know with second babies you can walk around being 2cm dilated for weeks. I requested two hours to see if I could get things moving but it just didn’t happen so at about 12:30 they started the drip and every half an hour they cranked it up and I was very comfortable for ages. I needed CTG monitoring and I used the TENS machine and I have to give a shout out to Jodi for her episode on breath and sound in The Birth Class; making sound kept me sane, it kept me feeling in control, as much as you can in birth. I couldn’t believe that something as simple as sound was so helpful from a pain relief point of view.
“By 5:30pm I was desperate for them to check me and by 6pm they checked me and I had a small cervical lip and it was gone within a few contractions. My midwife was calm and in control and told me what I needed to do. I knew when it had cleared because I could feel Darcy move down, honestly the feeling of her head coming through was indescribably. She moved down so much faster, things were happening really quickly. They told me to stop pushing as she was crowning and I pushed her out and I had a tiny little tear that didn’t even need stitches. Labour was just under two hours and I caught her in between my legs and brought her up.”
While Andrea had every intention of breastfeeding with Leo, issues arose two days after he was born.
“He had a great latch but a severe tongue tie, and he went 24 hours without a wet nappy. The pediatricians stepped in and said I needed to feed him formula. It took weeks of meeting with specialists and lactation consulatants (and withstanding a lot of pressure and criticism) till someone told me I have breast hypoplasia, also known as insufficient glandular tissue. You can have very normal looking breasts and have a lack of glandular tissue. I make milk but I don’t have enough glandular tissue to store it. I was on medication, taking supplements, eating the cookies and breastfeeding, formula feeding and then pumping. We met with so many people and I had to really emphasise that it wasn’t for lack of trying but it was never going to happen for us. We ended up mixed feeding but I pumped everyday and fed him one bottle of breastmilk a day till six months and the same with Darcy. I had enough colostrum to get Darcy through our time in hospital and we started formula feeding once we were home.”


Topics Discussed
Breast hypoplasia, Formula feeding, Induction, IVF, Postnatal anxiety, Prenatal anxiety, Same sex couple, Sperm donor, Two Vaginal Births
Episode Sponsor
Bonds Baby Cover is a comprehensive ‘poo-licy’ for new parents that compensates parents for the first-time parent experience with free Bonds babywear. There’s cover for ‘natural disaster’ we’re talking grade 5 Poonamis here, ‘Vandalism’ – wilful texta damage to walls and clothing – and ‘Third Party for when ‘it’ goes everywhere and on everyone. Even accidental-probably-on-purpose damage is covered. If my three boys are proof, little cuties can be massive liabilities. Parents simply sign up to make a claim and be compensated with Bonds Babywear. To be clear, that’s free product, parentals! To sign yourself up head to BONDS
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






