EPISODE 263
Hollie

Hollie and Hayley consulted IVF Australia and sourced a sperm donor from the United States to start their family (they have the same donor for all four of their children). Hayley opted to go through the IVF process first, mostly due to her age but they agree it was a very organic decision process. Hayley’s second cycle was successful and after being diagnosed with gestational diabetes, she was cared for by a specialist midwife program that also offered her continuity of care and managed her condition with a very low dose of insulin and diet.
“Before you start the IVF process you try to do as much research as you can because it can be quite stressful. Thankfully our experience was incredibly positive; there weren’t any complications or issues with the injections or feeling down. I know we are fortunate that we didn’t experience infertility or any issues. The process was really smooth and we felt really educated by the specialists.
We knew from the outset that gestational diabetes would most probably lead to an induction but in hindsight it could have been avoided. Induction began with the cervical gel and by midday the syntocinon drip had started. Hayley only laboured for five hours and while it was intense, she handled it really well. I felt really confident in the education we had and as a support person I was focused on making sure I was a conduit between her and the medical staff so she could make informed decisions and not digest additional information that she didn’t need. She made the whole birthing experience look very easy which was very deceiving.
While Hayley was being induced, Hollie got her bloods done in preparation for her first round of IVF. They were aware that the chances of falling pregnant on the first round are extremely low so they never expected to fall straight away. However, less than a month after Hayley gave birth, Hollie fell pregnant.
“My pregnancy was really cruisy; the only thing that stands out for me was feeling like I was out of breath. I think it was just the increase in blood flow. You have a lot of scans with IVF but I also think it’s quite an individual situation based on the woman and the specialist. I developed gestational diabetes as well and I was in the same midwifery programme as Hayley and we ended up with the same midwife which was amazing.
“Induction was scheduled for 39 weeks; they applied the cervical gel in the morning and hooked up the syntocinon drip later on. It was a really slow start. They gave me something to sleep overnight and the next day they broke my waters at about 1pm. As soon as they did I experienced incredibly intense contractions; it was a completely different birthing environment. I felt like I didn’t have any control over what my body was doing. Initially I tried the gas but it made me feel really nauseous and I vomited a few times. I had an epidural but I still had sensation and it was a really positive experience because I could feel what was going on without the distraction of the intensity of deep labour.
“I was on the monitor and her heartrate had dropped a couple of times which resulted in a medical team coming in to intervene. The most important thing that I got out of that experience was how fantastic my midwife was in that situation. We’d had many conversations with her about the birth and she knew that if the baby and I were ok, we wanted to avoid any suggested intervention. There was a moment where the baby’s heart rate had dropped and my midwife said to the obstetrician and the team; just let her be and the next contraction I gave birth. It was that encouragement and support that really empowered me to get through that moment, to make sure we were both safe, and if it wasn’t for having that advocate I’m not sure I would have been able to do it because you’re just so overwhelmed with everything that’s going on. I felt like I needed that external encouragement from someone I trusted.”
Hayley did one more round of IVF but unfortunately, it wasn’t successful. Hollie decided to do another round and it was successful; a test at four days post-transfer revealed that she was pregnant.
“I don’t know why we tested so early because rationally it doesn’t make sense. But we did. When we tested after that it was showing very strong lines and the possibility of twins crossed my mind but I really didn’t think about it any more than that. It’s tempting to hypothesise about what’s going on in that period but a lot of things can happen and we were just trying to stay level headed.
“We’d had the two week wait and we had subsequent blood tests to show that the hCG levels were rising. The 7 week scan showed a sack and what we thought was one little person. But then a week or so later I was incredibly fatigued which was a new experience but then my hCG levels were through the roof. At 9 weeks I was very sick and my first thought was I was carrying a boy but later that week I found out I was pregnant with MCDA (one placenta, two sacs) identical twins. There was an overwhelming feeling of shock but it was also phenomenal. It also justified why I was feeling so terrible.”
Hollie had a hematoma – at its biggest it was 7x5cm – and it caused weeks of bleeding and anxiety. There was a concern that it would continue growing and affect the placenta. She was over 20 weeks when the bleeding subsided and scans revealed that her body had absorbed it.
“I found the experience forced me to mentally separate from the babies because I was scared of losing them. The anxiety was there constantly and I’d check every time I was in the shower or on the toilet. We moved to Darwin halfway through the pregnancy and I was placed in the continuity of care midwife program as well as being linked up with a student midwife. My student midwife ended up being one of the most positive things that had happened in my pregnancy. She was so supportive, so thorough, she kept us in the loop, she was professional beyond her training and ultimately she was a fabulous addition to our experience.
“I was tested quite early for gestational diabetes and it came back positive – I needed medication at night to assist with my fasting levels. The twins were on top of one another; one was posterior and one was anterior so I felt all the movements in the same place. Having one placenta for two babies poses some risks towards the end of pregnancy so 37 weeks was the goal for us. There was a lot of talk expecting them to come early but we tried to be realistic in the sense that I would potentially birth them before 37 weeks. In an ideal world I didn’t want interventions but by 36 weeks I was trying to naturally induce labour
“Two weeks before birth twin B decided to turn breech but luckily twin A was head down. I was more than happy to have an epidural for the birth but it was more to avoid a situation where there was an emergency and I needed to go under general anaesthetic. The outcome was to have two healthy babies and a healthy mother and I had prepared for a general but it was absolutely not what I wanted so I did everything I could to mitigate that risk.
“I was having fortnightly scans from 13 weeks because of the hematoma and MCDA twins, leading up to 37 weeks. I had weekly traces too and in my last trace it showed I was having contractions; I could only feel pressure and I just presumed it was the size of the babies. I started to contract five days prior to my induction and I tried every old wives tale to go into labour – I was bouncing on the ball, eating pineapples, eating spicy food because I really wanted a spontaneous, drug-free vaginal birth even though I knew that it wasn’t realistic. It was still something I was very much hoping for. One thing that was prevalent all through the pregnancy was that I embraced hypnobirthing and that was a vital part of the twins’ birth.
“I was scheduled for an induction at 37 weeks. We went in after lunch, I had an internal and I was already 4cm so they cancelled the induction and I made the choice to stay in hospital which ended up being a good decision because my waters broke that night at 9pm and the twins were born an hour and a half later.
“As soon as my waters broke I had the sensation of wanting to push. There was no rise and fall of contractions; it was all rise. And this is where hypnobirthing came into play, I had to call into those skills I learnt during pregnancy to stay in that calm headspace. The contractions were so intense that I couldn’t walk and I was also thinking about the epidural. Baby A was head down and they were more than happy for me to push him out.
“I definitely felt during this labour that the babies birthed themselves. The only thing I had control over was my mind. And that was something I was focused on throughout the pregnancy; I knew my body would do what it needed to do, I knew the twins would do what they needed to do, but I needed to make sure my mind was strong otherwise it would interfere with the birth. I felt like my body was doing it all by itself. It was a magical, incredibly challenging, empowering experience.
“There was 12 minutes between the twins. Baby A came out and he was fine, I held him and was contracting while I was holding him but I had sensory overload and handed him to my partner. I was listening to a meditation the whole time and I was very focused on keeping my body relaxed. Twin B was breech and I was very firm in saying if there was no issue with the baby or me, then just let me birth him and obviously the hospital staff wanted to manage risk and at that time they couldn’t find his heartbeat. My midwife was quite assertive and just told them to let me do it and they did. He was born in his sack; his body was out and then they broke the sack. My recollection of the birth is somewhat distorted because I was so intrinsically focussed but I do remember them putting a lot of towels around because often the sack explodes. There are photos of the obstetrician breaking the sack.
“It was very much like a healthy singleton pregnancy; they had delayed cord clamping, they were healthy weights, I had them on my chest straight away. I did have to have my placenta manually removed though and I do regret not having a good look at my placenta.
“I was focussed on having a fear-free birth and that included having birth preferences in various scenarios and my partner and my care providers were aware of them. We didn’t feel that people were making decisions for us; we were realistic in our expectations but we also felt that we had discussed all the eventualities and we were informed about all the possibilities.”
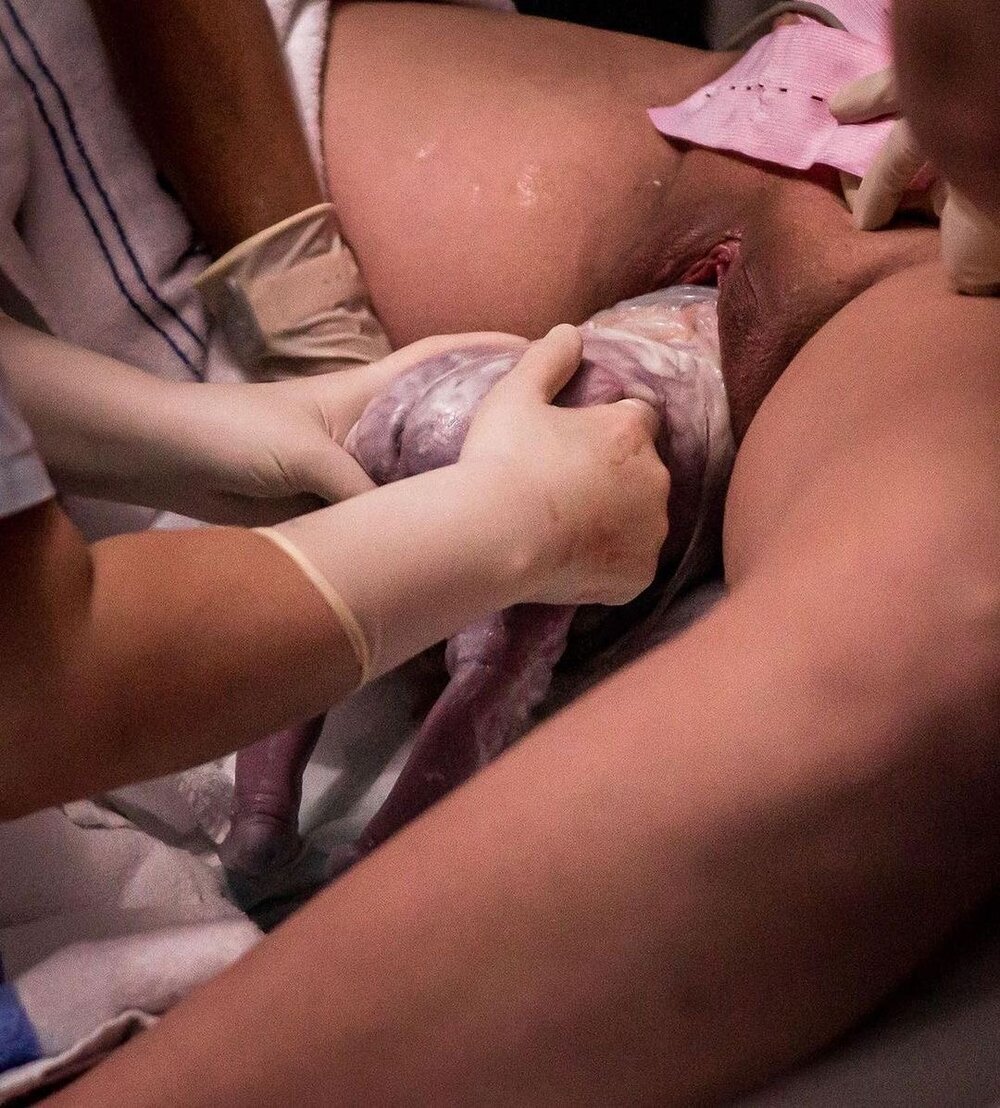
Image by Birthright Collective
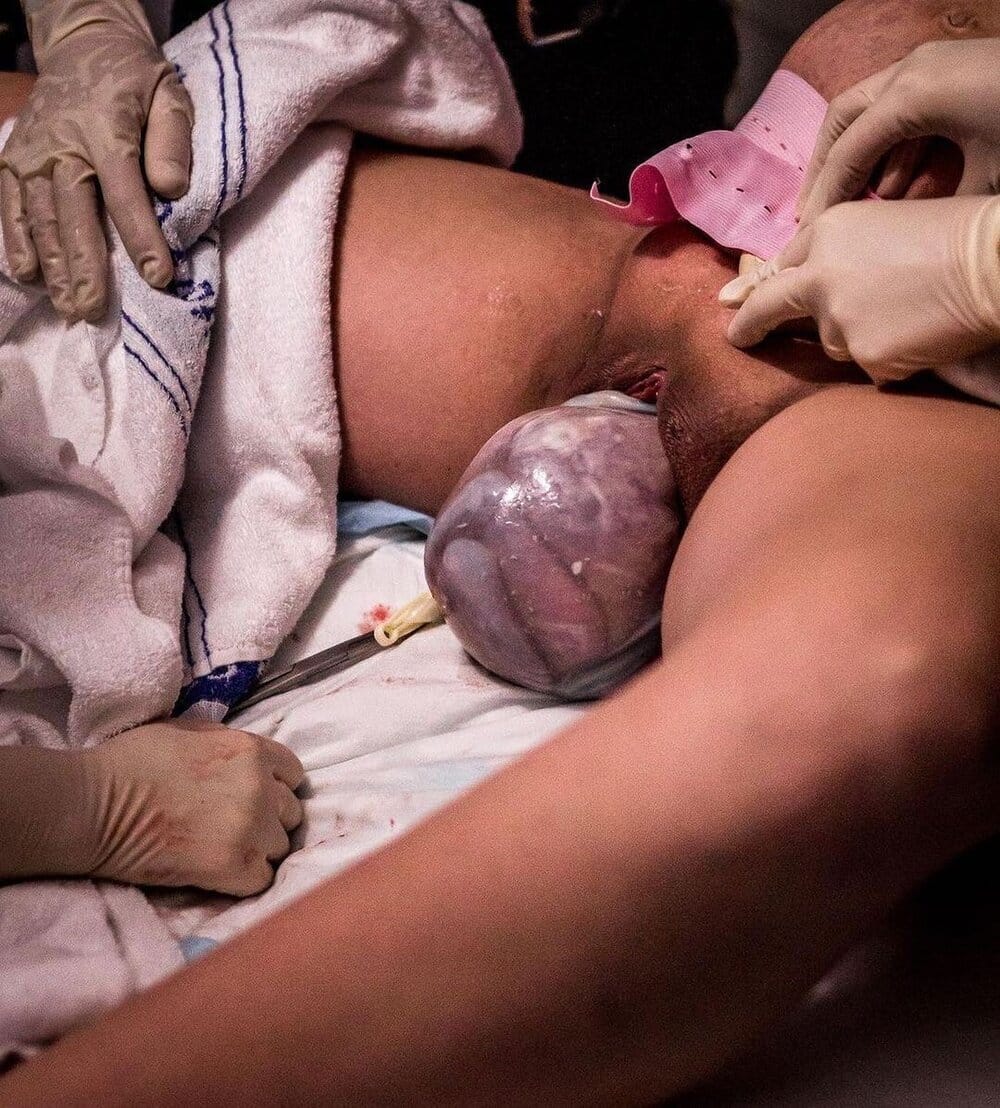
Image by Birthright Collective


Image by Birthright Collective
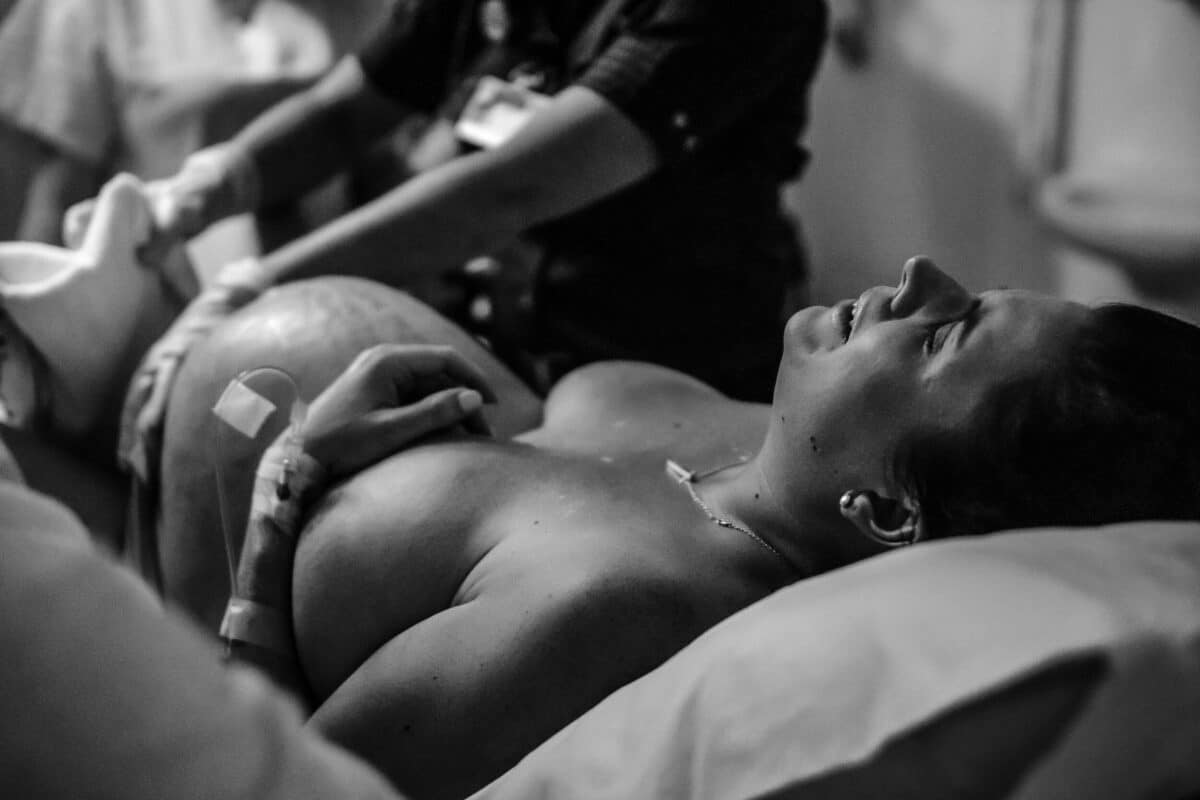
Image by Birthright Collective
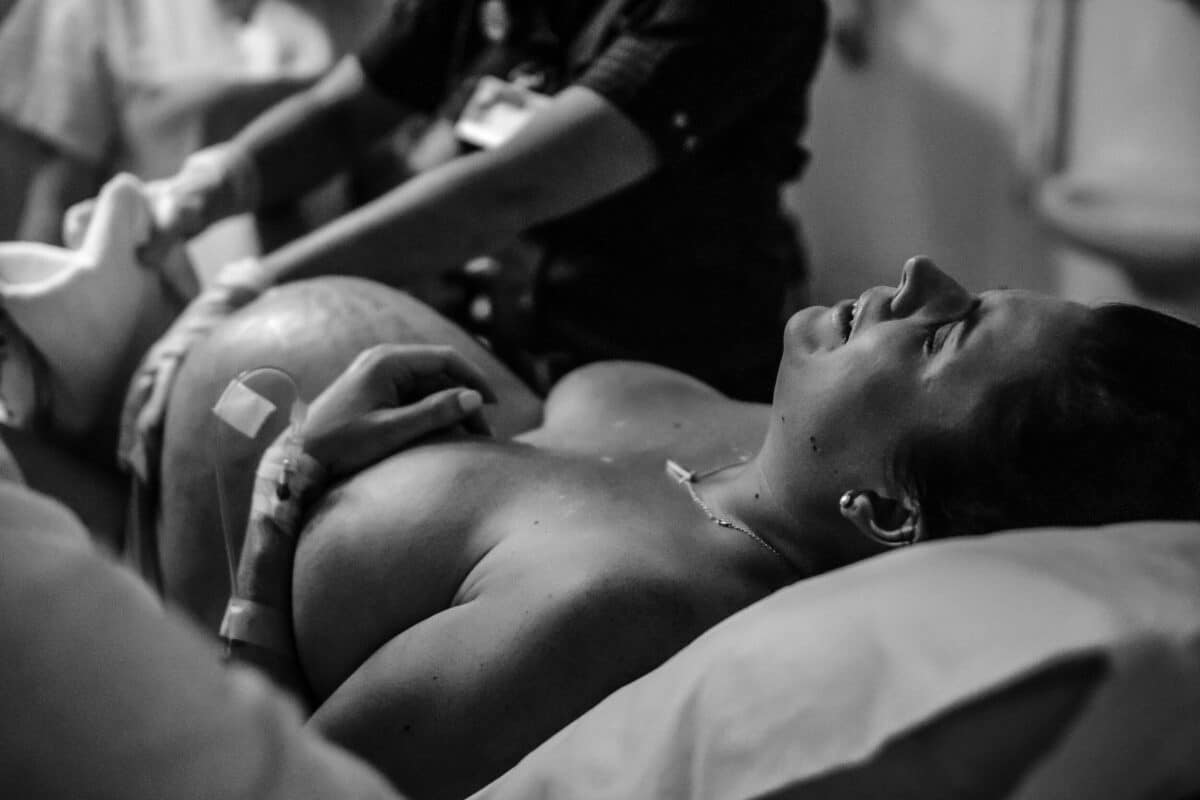
Image by Birthright Collective
Topics Discussed
Gestational Diabetes (GD), IVF, MCDA Twins, Same sex relationship, Sperm donor, Three vaginal births
Episode Sponsor
Today’s episode is brought to you by DockATot. This multi-award-winning baby lounger is uniquely shaped to recreate a womblike environment to soothe and settle your baby. The DockATot has thousands of 5-star reviews from parents across the world who’ve enjoyed its calming effects on their babies. New parents often say the DockATot is like having an extra set of hands always at the ready because it offers baby a safe place to rest or play wherever you are. Being lightweight and portable, the DockATot can be used around the house and is also perfect for family adventures to the park, beach or beyond.
Handmade in Europe from premium quality materials, the DockATot has become an absolute global parenting must-have. So if you’d love an extra set of hands around the house to help you as a new parent, check out DockATot.com.au and as an ABS listener you can enjoy 10% off any DockATot and their amazing range of accessories. Just enter the code ‘ABS10’ at checkout.
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






