Podcasts Nerique
EPISODE 245
Nerique
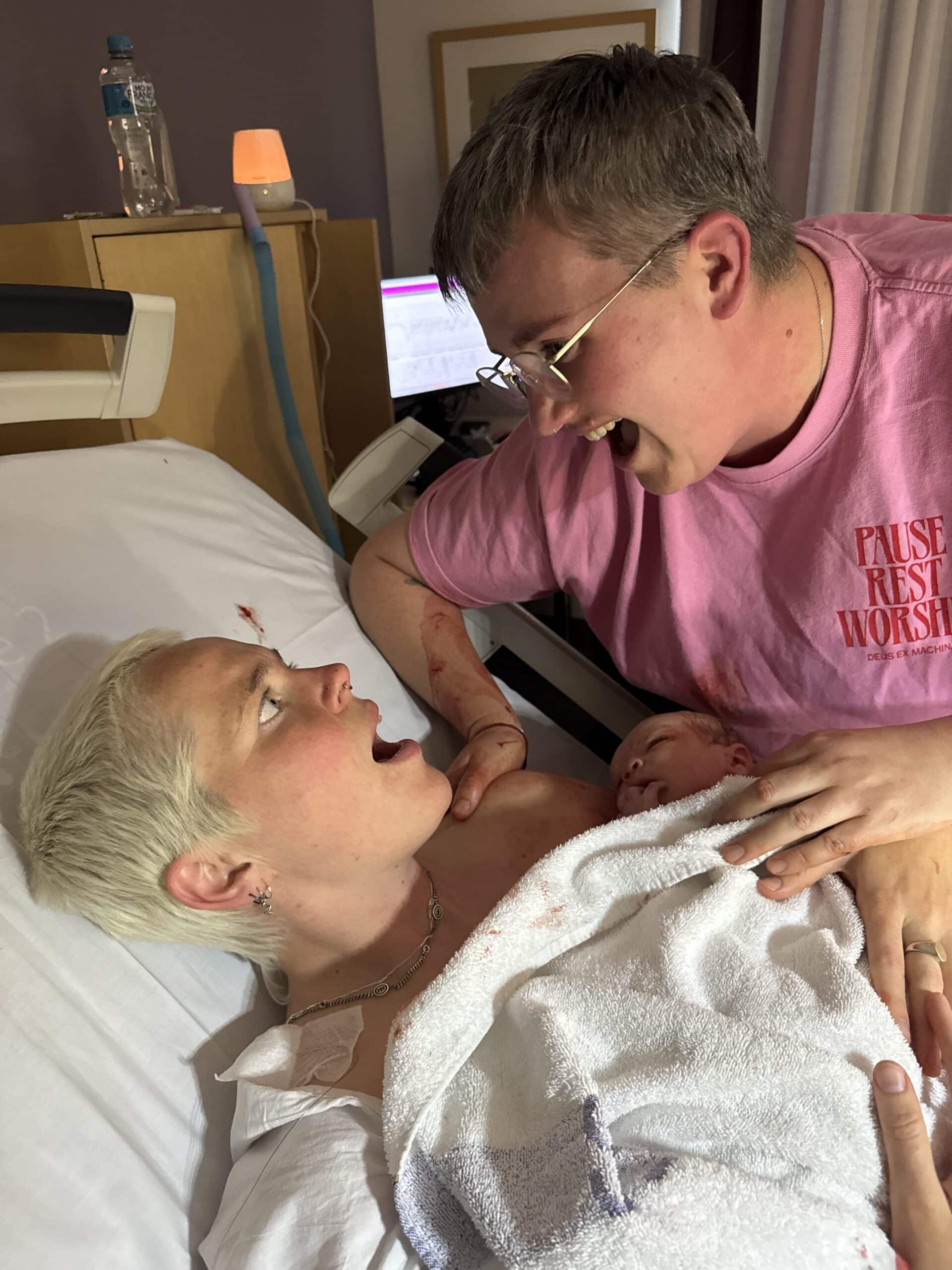
“We started trying for a baby in 2019 and we fell pregnant in the first month. That pregnancy went smoothly until our 10 week scan. I had the nausea, everything was fine, the six week viability scan looked fine and then when we went for our next scan we discovered that the baby didn’t have a heartbeat. I hadn’t had any signs of a miscarriage so I saw my GP and she told me I could wait to miscarry naturally or see an OB for a D+C.
“I really wanted to do a D+C and move forward. The great thing about that was that they could test the tisse. It was a little boy and he had an extra chromosome; he had three chromosome 16s and he was never going to be viable. I admit, there was some comfort in finding those results.
“The miscarriage completely blindsided me; I’ve joined so many support groups and spoken to so many women and found this incredible community – the Pink Elephant Support Network (pinkelephants.org.au) – who are there for those who have experienced miscarriage and early infant loss. They offer levels of support for the different stages you go through; when you’ve miscarried, once you’re ready to start conceiving again and then when you’re pregnant after loss.”
Nerique wanted to get pregnant soon after miscarrying but her cycle was irregular; she would have extremely long cycles and painful periods. After six months with no signs of improvement, she went to see a fertility specialist at IVF Australia. She didn’t think IVF would be a necessary option but she wanted to have more thorough tests conducted, including ovulation tracking and a sonohysterogram. The sonohysterogram revealed that scar tissue from the D+C had resulted in a blockage in her cervix which explained her painful periods and also flagged why she was having trouble conceiving. The specialist broke through the scar tissue to flush out her tubes and recommended Nerique start on letrozole which helped make her ovulation cycle more predictable. She also had regular scans to monitor her cycle which revealed that she was ovulating late in her cycle (day 22). Two weeks later she did a positive pregnancy test.
“My sister had a great experience with Midwife Group Practice so I knew I wanted the same care. I also knew that I needed to call early to get in so as soon as I did a positive test I was on the phone. I stayed with my fertility doctor till 12 weeks, she knew my story and made me feel really supported, especially considered my miscarriage and my anxiety surrounding the scans. She handed me over to my midwife at the start of my second trimester.
“I was really excited about giving birth, I wasn’t scared.. I’ve done an ultra-marathon, I’ve done an ironman, I’ve been a competitive horse rider…I felt like I had the big match temperament to get on with it. I also felt really informed from my reading and listening to your podcast. I didn’t have a birth plan but I did know that I wanted to have a vaginal birth, I was very open to pain relief and I bought a tens machine. I suppose my plan was to go in with an open mind.
“At my 38 week appointment I mentioned that I felt like my belly hadn’t grown in the past two weeks and after measuring my fundal height we realised I was right. They monitored me for an hour and her heartbeat was fine but my midwife felt that getting an ultrasound would be the best option. They picked up that she was really small; she was in the second percentile and measuring at 2.4kg. The doctor felt that she wasn’t getting what she needed in my belly and it was time for her to be born. I just burst into tears.”
Nerique stayed in hospital that night to be monitored and her waters were broken the next morning. Thirty minutes later she started the syntocinon drip and they increased the dosage every fifteen minutes.
“I went into active labour very quickly. The contractions were very regular and very intense very quickly. Within half an hour they were a minute long and a fifteen second break in between. The birthing unit room was so big but I was positioned in one corner, between the bed and the wall. I was on my hands and knees in a corner of the room and that’s where I was going to stay. I asked for the fitball and I lent onto it and was breathing through the contractions. My husband was on the other side of the ball and he was holding my hands, and I was grasping onto him through each contraction.
“I was really struggling and was focussed on each moment and getting through each contraction. I requested the epidural but then after an hour of active labour I started to get an urge to push; just after the period of me feeling like I couldn’t go on and couldn’t cope. Obviously that was me in transition.
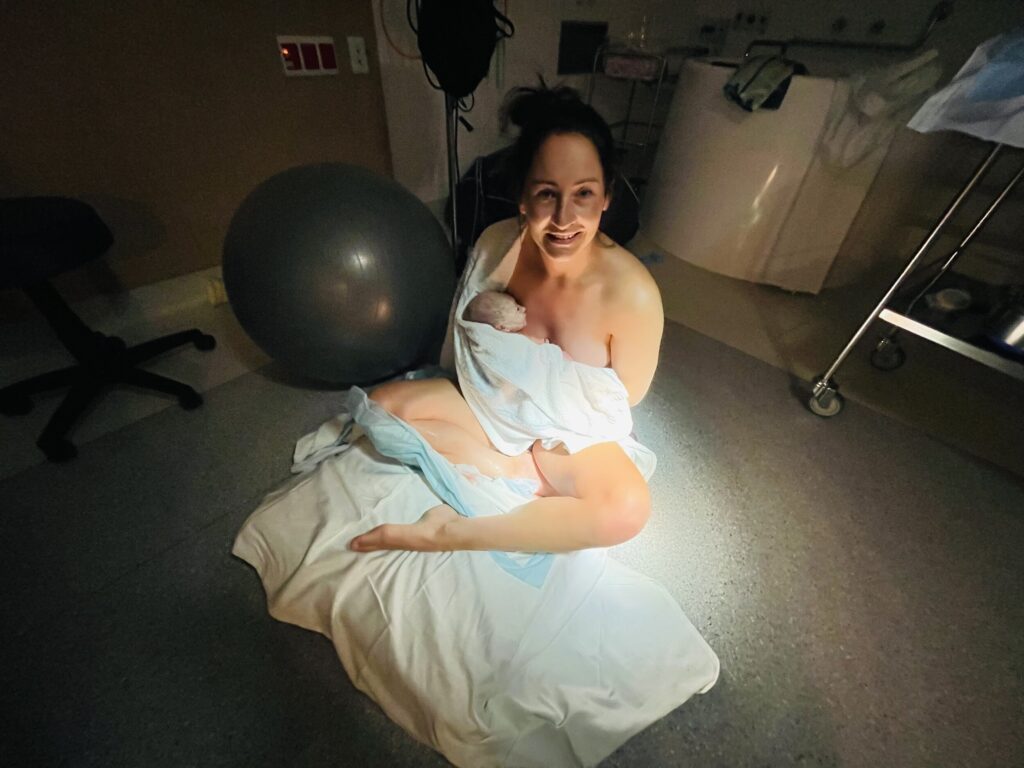
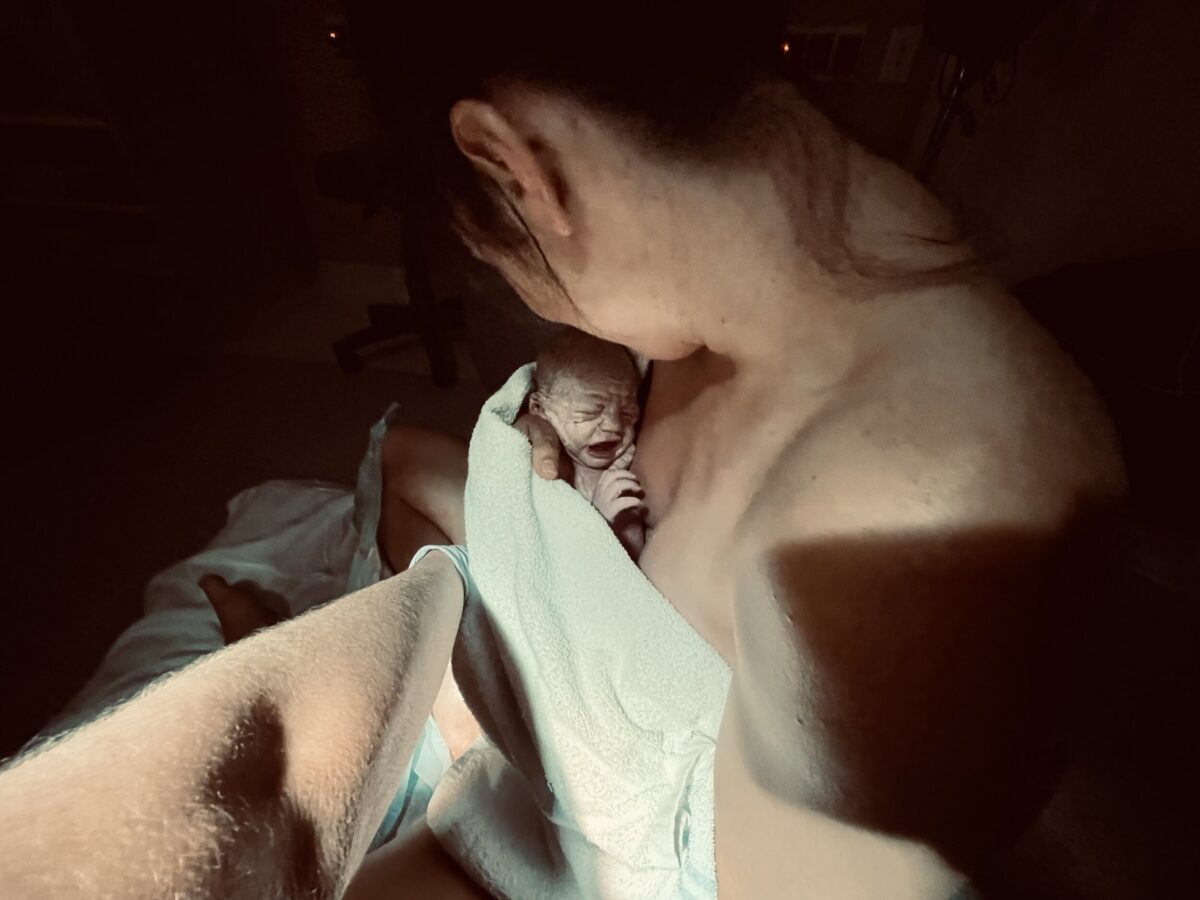
“Once I could start pushing I started feeling more positive because I could use the contractions. I felt like my body was riding with the contractions, they weren’t painful. As soon as the contraction stopped, I stopped pushing. The whole time her heartbeat was being monitored and she was coping with the pushing but her heartrate was dropping a bit. Rosie, my midwife, recommended lifting one knee and it felt like I opened up my pelvis a lot more and it helped me push and she started to come down easily. I was on my hands and knees and they gave her to me through my legs. I sat on the floor and held her and she was tiny but screaming. She was 2.55kg and got an Apgar score of 9; she was small but perfect.”
Baby Lara struggled to latch in hospital and because it was a quick labour she swallowed lots of mucous and wasn’t interested in feeding. Nerique hand expressed colostrum and fed her through a syringe and then used a nipple shield to encourage her to latch; she used it for six months.
“It was challenging and I had to express a lot; it definitely hasn’t been the beautiful breastfeeding journey I hoped for. But now she’s on formula and solids and she’s thriving…deciding to stop feeding was a really good choice for my mental health.”
Pink Elephant: https://www.pinkelephants.org.au

Topics Discussed
D+C, Fertility treatment, Induction, Letrozole, MGP, Missed miscarriage, Nipple shield, Sonohysterogram, Vaginal birth
Episode Sponsor
Today’s episode is brought to you by tooshies by TOM. We often hear that parents don’t trust that eco options really work and when it comes to nappies and wipes for our babies, we want and need the best. It’s hard to imagine that well-performing disposable products can coexist with environmentally friendly ingredients.
tooshies by TOM made it their mission to make nappies and wipes that work, while also considering the environment. They searched the globe to find manufacturers aligned to their values, so they could make products with sustainable and ethically sourced materials that work just as well, if not better than those found in conventional products.
Tooshies by TOM wipes. Toxin-free, plastic-free and biodegradable. Available at select retailers. Or, shop directly at thetomco.com and receive 15% off your first plastic-free wipes order with promo code ABS15.
Categories
Related Products
-
Birth Meditations
$49.00Narrated by Sophie Walker, these soothing and informative meditations help you feel supported and confident around birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us