EPISODE 304
Sea
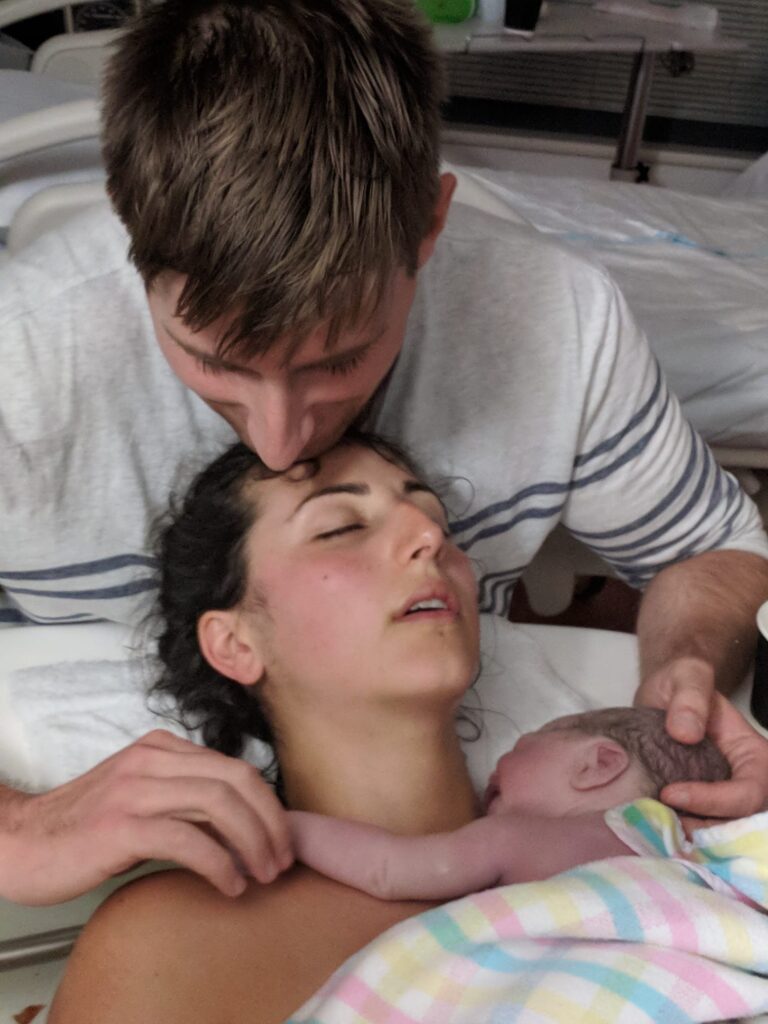
The youngest of seven children, Sea witnessed one of her sisters giving birth but admits that her knowledge was limited. When she fell pregnant with baby Luna she started listening to podcasts – including Australian Birth Stories – and as she had a really good family GP, she opted for shared care with her GP and the Indigenous Midwifery Group Practice at her local hospital.
“It was like having a private midwife without having to pay for it and I was so grateful for that. I was allowed to have as many people as I wanted in the birth space so I had my husband and my two sisters with me. Culturally we birth as a community so it’s so good to have this opportunity in the hospital system.
“I was nauseous and my palate was so sensitive in the first trimester, I always used to gag when brushing my teeth. But then as soon as I reached 13 weeks I felt so good and that continued right through my pregnancy. I finished work on the Monday and on the Tuesday it was our one year wedding anniversary. I had tightenings that morning and I noticed I’d passed my mucous plug. That evening my sisters told me I needed to have sex to get things going so they went out for dinner and my husband and I did the deed and it definitely moved things along. I laboured into the night, I was lying on the lounge on my side so I could sleep between contractions. We went to the hospital at 1am and my midwife asked if I wanted to be checked and I did, I was 4cm and doing really well. I felt like I couldn’t do it but my husband and sisters encouraged me to get in the bath. I hung over the edge of the bath and it was comfortable there.
“My midwives monitored the baby’s heart rate in the water and I didn’t have any more internals. I begged for the epidural but my sisters told me I was so close and I could feel pressure building so I pushed and my waters broke. Luna was born within a few pushes and I felt on top of the world. She was born at 3:55am. I got out of the bath because there was quite a bit of blood and the midwives find it hard to measure in the water. We did delayed cord clamping and once the cord was cut my husband held Luna and I went to the bathroom to birth the placenta on the toilet.
“I put Luna on me and she did the breast crawl and started feeding. I was exhausted and she just fed while I dozed. Once my second degree tear had been stitched I went home a few hours later. I was so excited to get in my own bed and have my own food. My midwife came that afternoon and the next day and visited me twice more in the following ten days.”
As soon as she found out she was pregnant for the second time she called the Mater Hospital and was accepted into the same MGP programme. She admits that she’d become a bit obsessed with birth and was excited to experience labour and birth all over again.
“I was really proud of myself for my first birth but this time I didn’t want to lose control. I was 39+4 when I started having mild contractions but they would drop off before starting again. By 40 weeks I was in labour…I went for a short walk with my husband and everything picked up. He counted during contractions so I could be subtly reminded of my inwards and outward breaths.
At 1:30pm I was feeling great and dealing well with contractions but my sisters were insistent that we go to hospital. Between the car and the birthing suite I had four contractions. As soon as I got there it was like my body knew; I was ready, in a safe space and I could let go. I got into the shower and I was making these mooing sounds and drilling my head into the wall. I was in transition and my husband and sisters encouraged me through it so by the time I got into the bath I was calm. I was able to scoop her up and bring her up to me. We got there at 1:30 and I birthed her at 2:30pm. We named her Lilykoi Iluka and we went home that evening.”
Sea’s third pregnancy was unplanned and coincided with a move to Cairns. It was a disruptive process that caused her anxiety, mostly because she was leaving behind her beloved midwifery group practice and entering a system where she couldn’t access continuity of care. Her 20 week scan showed a possible obstruction in baby London’s intestine which placed her as high risk but even so, she only saw a midwife once by the start of her third trimester. At 34 weeks her fundal measurement was 28 so she had to have more scans but she intuitively felt that everything was fine. At 39 weeks she tested positive for Covid which forced her to rest for a whole week; the silver lining of the virus and the ideal preparation for labour.
“I had pre-labour contractions for days, much like Lilykoi’s labour. The night before I went into labour I felt like the contractions were getting more consistent so my sister’s flew up to Cairns to support me. I tried to relax, I felt so in control, the sensations were there but it wasn’t painful. I could feel that she was dropping, my body was dropping.
“By the early evening my husband and I went to hospital and we chatted all the way there. I didn’t know any of the midwives which was hard but thankfully I got a room with a bath in it. I wanted to stand and sway in this labour and my husband was pushing my hips while my sisters were on facetime. The midwife told me the rules changed that morning so my sisters could come and they arrived within half an hour. The room was dark, there were fairy lights, I just felt so safe. I got in the shower and everything just seemed to stop. I got into the bath and I was breathing down and breathing her out and I brought her up onto my chest and it was just amazing. I didn’t realise you could birth and you could breathe through it all and stay so in control and feel it all, it was the most empowering experience.”
Sea talks about her changed perspective on postpartum; instead of getting back into exercise she relished lots of time in bed, slow days, skin-to-skin snuggles, nourishing meals and not getting too caught up in sleep expectations.


Topics Discussed
Breastfeeding, Indigenous, MGP, Postpartum, Three physiological births
Episode Sponsor
This episode of Australian Birth Stories was proudly brought to you by our friends at Bellamy’s Organic. With so many food choices, it is difficult to know what’s best. At Bellamy’s Organic, they only make certified organic, nutritious baby food. They believe that a meal is more than nourishment and that’s why they’re committed to introducing an early love of nutritious, wholesome organic food to children. Research shows that starting babies early on healthy foods early in development, helps foster healthy eating habits throughout life.
Their range of organic cereals, pastas, rusks, snacks and pouches help babies adapt to new flavours and textures and are approved by paediatric dietitians. With Bellamy’s Organic, you can be confident you are giving your little ones a pure start to life. Available in your local supermarket or pharmacy, or shop directly on the Bellamy’s Organic website. Use the code ABS20 for 20% off your next baby food order!
Categories
Related Products
-
The Birth Class
108 reviews$249.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






