EPISODE 318
Laura
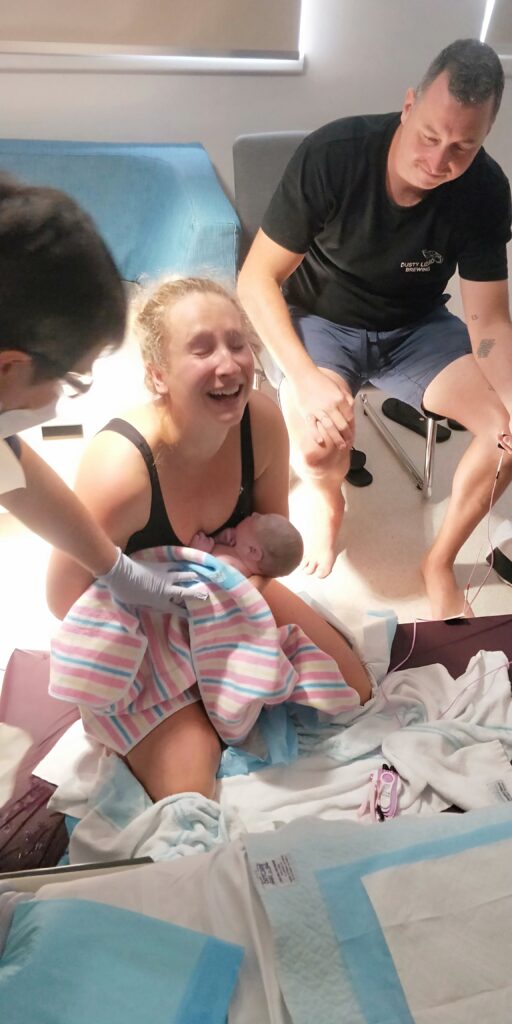
Laura and Ryan have been together since she was 19. After getting married and travelling overseas on and off for years, Laura fell pregnant while on holiday in Vanuatu. She had private healthcare and liked the fact that she could experience continuity of care with an obstetrician.
“The only thing that irked me about obstetric care is that they’re not there for your whole labour. They’re only really there for the end part. I developed varicose veins at 24 weeks. I’ve always had a few spider veins and they became more prominent as my pregnancy progressed, particularly on my right leg – hot and swollen especially after spending the day on my feet. I ended up having to wear compression socks on my lower leg and it definitely helped with relieving the pressure. They went away as soon as I gave birth, which was a relief.
“At a routine scan at 33 weeks they discovered that my amniotic fluid was really low. From there I had weekly ultrasounds and twice-weekly CTG monitoring so they could keep track of everything. Within two weeks the levels were at a normal level. At 38 weeks the amniotic fluid decreased again and my obstetrician recommended induction. It was the first time that I wasn’t happy with my model of care because I felt like I hadn’t been listened to. Earlier in the pregnancy I brought up my birth plan and she just wrote a few of my preferences in my notes which included no induction and no epidural. I felt quite defeated, especially when she said to me: we don’t want a dead baby. How can you go with your gut or intuition if someone says this? But that’s also not the alternative; it’s not induction or dead baby. I freaked out when she said induction and I didn’t ask questions and that’s something I regret.
“She booked me for the induction but she suggested a stretch and sweep first. I was already 2cm and she told me that she thought I’d have my baby over the weekend. I’d been drinking raspberry leaf tea, I’d been eating dates to soften my cervix, I’d been having sex and stimulating my nipples. After the stretch and sweep I started having cramps that afternoon and the next morning I had a bloody show.”
By 9am she was having contractions 1-2 minutes apart and she was having to actively breathe through them. She noticed that her leg was throbbing and she couldn’t stand on it during contractions, despite the fact that she wanted to be in active birth positions. Once Laura arrived at hospital, the midwife did a vaginal examination, told Laura she was 2cm and promptly told her that she was breaking her waters. The second that she did, her contractions were incredibly intense and she needed full length compression stockings to ease the pressure of her varicose veins.
“I ended up vomiting while I was having contractions and it was awful. I got in the shower; they didn’t have a bath at the hospital which was really disappointing. The midwives and obstetrician didn’t really suggest any positions or techniques that could help me and I didn’t really know how to ask. Within four hours I was only 4cm and since my waters had broken I was on the clock. They weren’t impressed with my progress. I was exhausted and they told me my only option was an epidural which, in retrospect, I know was not the only option. The midwife was really dismissive of my wish to have a drug-free birth and I just burst into tears. I saw the anaesthetist and I hated him; I didn’t want to see him or cooperate. I felt so angry in my head and overall just defeated. Once I’d had the epidural and they checked me again, they told me that the baby was posterior. I admit that the epidural did help me relax and it allowed me to dilate quite quickly.
“I came to terms with it and realised that my baby was well, I was well, and once I was ready to push I would have the energy for it. The midwife came in at 9pm and I started pushing and did so really effectively; Leila was born within 20 minutes. Because of the syntocinon and epidural, Leila was quite sleepy but she managed to latch and had a really good feed. I ended up spending six nights in hospital and breastfeeding was really challenging. She developed jaundice and her latch wasn’t great and I ended up with cracked and bleeding nipples. I ended up having to do top-up formula feeds and I developed really bad baby blues. Getting help from the midwives was really good but there were different opinions and by the end of the week I just knew I needed to get out of the hospital.”
Laura talks at length about her breastfeeding challenges, her choice to use donor breast milk and a supply line. As well as taking motilium to boost her milk supply she switched to formula top-ups at three-months but for a long while she was triple feeding; breastfeeding, expressing and formula feeding. Laura ended up breastfeeding in some capacity till Leila was 14 months old.
“I hadn’t had a period which is why I stopped taking motilium and breastfeeding. I went to the GP and she sent me for an ultrasound that showed a collapsed follicle which means I had just ovulated. It took us four months to fall pregnant. I really wanted to try and have the birth that I intended to have so I contacted MGP at 4 weeks and explained that I felt quite dismissed in my first pregnancy and birth. Yet from the moment I spoke to my own midwife I felt so heard and we had the same goals. It was quite odd to have less scans and appointments though.
“I made it my goal to listen to every podcast episode and I started from the first episode and then we did The Birth Class. We listened to it early in the morning in bed and we went back in late pregnancy to listen to Rhea Dempsey’s episode. I also hired a TENS machine and I’m so glad I got it. My varicose veins came back with a vengeance and extended into my foot and achilles tendon and I had to wear prescription stockings which were much more firm.
“The week leading up to birth was hard. My sister had her baby when I was 38 weeks and her birth was really traumatic and it really shook me. My midwife looked me square in the eyes and said: this is a different baby for you and your labour will not be the same as your sister’s. When I was 39 weeks my midwife offered me a stretch and sweep but I declined; she checked me though and I was 3cm and very soft. At 40+2 it all began. I lost my plug in the morning and when I got out of bed the contractions really took all of my attention and they were two minutes apart. I had breakfast with Leila and then at 8:15am I put on the TENS machine and it was so, so good. It was something else to focus on; it didn’t take the pain away but the buzz-sensation was a bit numbing after a while. We got to the hospital and my midwife checked and I told her I didn’t want to know but she did tell me I was more than the 3cm I was days ago.
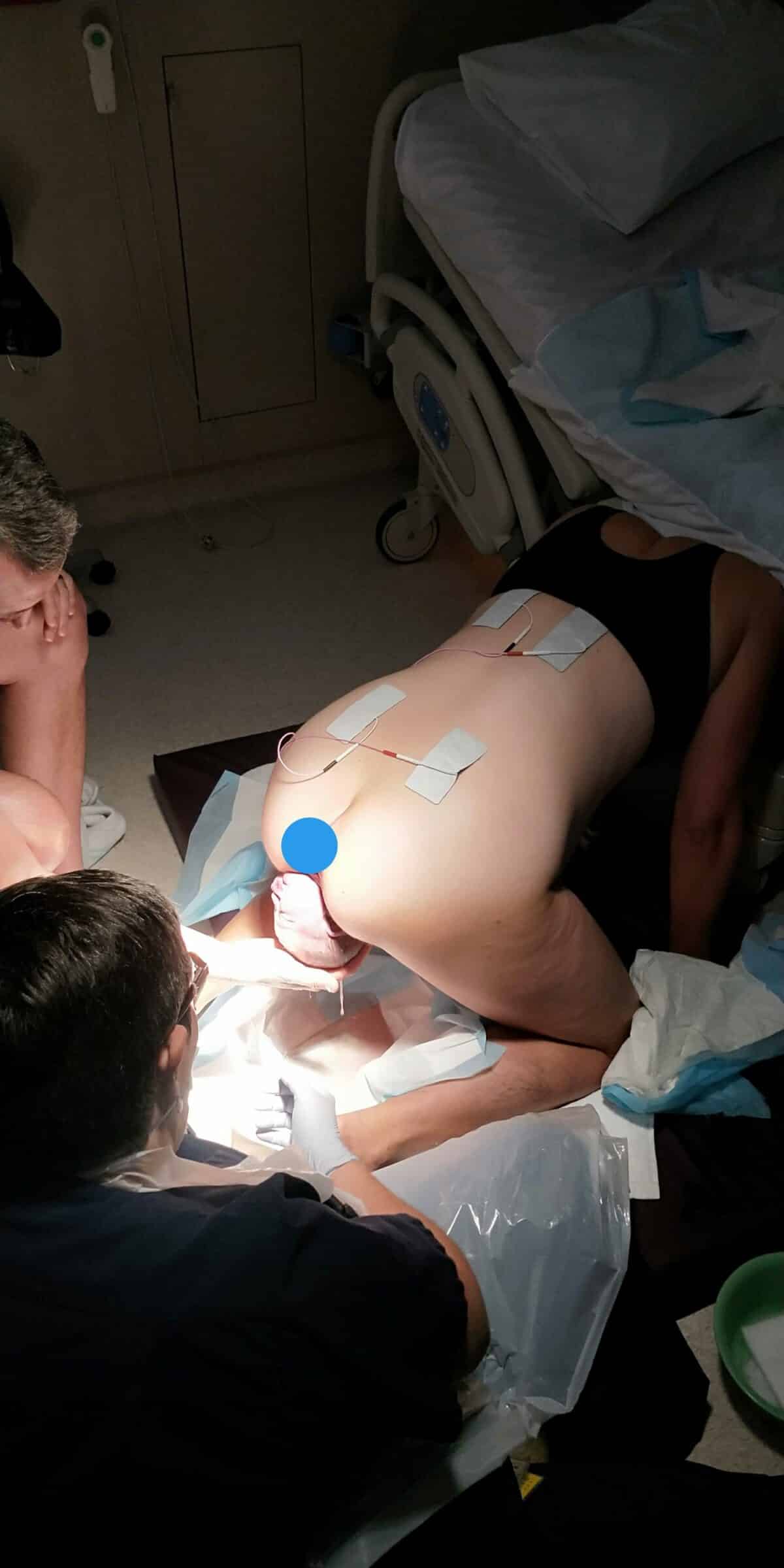
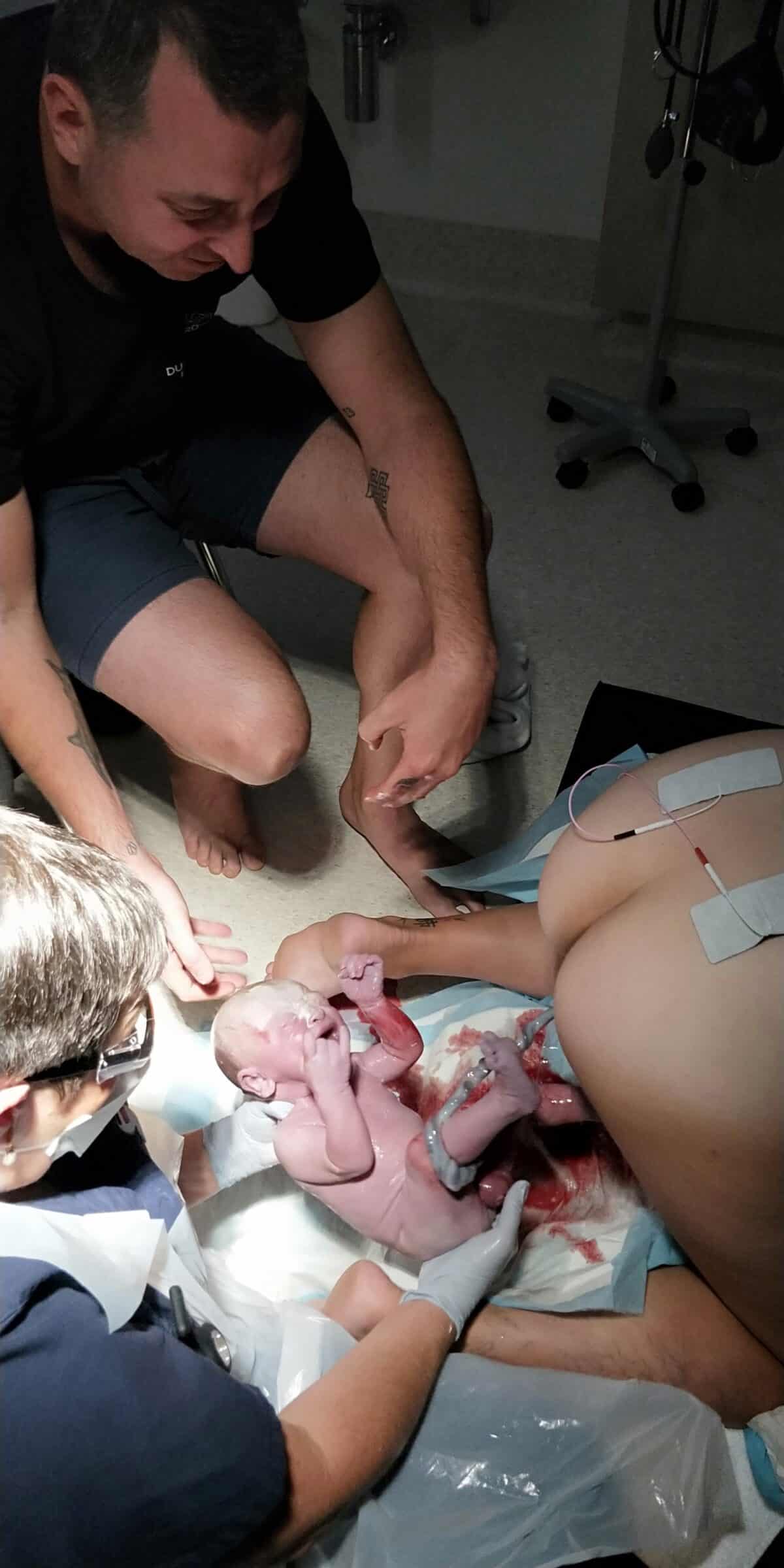
“I was down on the floor and told Ryan I wanted to push and he told me I was 9cm. I asked the midwife to check me again because I really needed to push and I was fully dilated with a bulging sac of waters. Three contractions later my waters broke which was such a weird sensation and then his head was born not too long after and he let out a cry while he was still inside me. And then there was a break between contractions and he was born on the next contraction.
“He latched a lot better than she ever did and he didn’t drop too much weight in the first few days. But by day 4 it was clear that my milk had come in and there just wasn’t enough so I got onto the Human Milk for Human Babies facebook page and a friend also offered her milk for me to use. One donor offered me 10 litres so it’s now sitting in my chest freezer and lasts for six months in there.”
Topics Discussed
Epidural, Low amniotic fluid, Low milk supply, OB, Two Vaginal Births, Varicose veins
Episode Sponsor
Bonds Baby Cover is a comprehensive ‘poo-licy’ for new parents that compensates parents for the first-time parent experience with free Bonds babywear. There’s cover for ‘natural disaster’ we’re talking grade 5 Poonamis here, ‘Vandalism’ – wilful texta damage to walls and clothing – and ‘Third Party for when ‘it’ goes everywhere and on everyone. Even accidental-probably-on-purpose damage is covered. If my three boys are proof, little cuties can be massive liabilities. Parents simply sign up to make a claim and be compensated with Bonds Babywear. To be clear, that’s free product, parentals! To sign yourself up head to BONDS
Categories
Related Products
-
The Birth Class
108 reviews$249.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






