EPISODE 248
Keira – IVF, Hyperemesis Gravidarum (HG)

“We’ve had six losses and we tried for 2.5years before Hunter was conceived. The first few miscarriages were early and they didn’t affect me as much but in January 2018 I had a Heterotopic pregnancy (one baby in the womb, one in the fallopian tube). It was misdiagnosed for four weeks and after finding out I was pregnant I instantly had pain in my left side and shoulder and I knew that there was something wrong. The scan showed the embryo and the sack and regardless of me telling the hospital staff that something was wrong, they didn’t listen.
“I ended up miscarrying the baby in my womb and then I had an ectopic pregnancy in my fallopian tube. That’s when I was introduced to trauma in my journey because I wasn’t being heard. It opened me up to the world that miscarriages and pregnancy loss are not spoken about enough and they’re so taboo. I fell into this world of infertility and trying to conceive after loss is such a gruelling process.
I had surgery, my left tube was removed and before then I had had regular periods and no pain. After the ectopic pregnancy I had debiltating pain and at times i looked six months pregnant. I had surgery and they found stage 4 endometriosis. It had grown from a stump of my fallopian tube that was left after the operation. There was a certain comfort in knowing that the endo was the reason I was losing my pregnancies.”
Keira sought out her third fertility specialist and went to her first appointment with a renewed determination to get some definite answers
“I just requested that he treat me and test me for everything. He finally found out that I have a genetic blood clotting condition called Factor 5 Leiden. There’s a lot of emerging studies that show it causes stillbirth in the second and third trimesters and it also affects implantation and first trimester loss.”
After receiving that diagnosis, she sought a new fertility specialist as recommended by her friend Rachael (you can hear Rachael’s story in episode 51) where she began her IVF journey.
“The whole process of IVF was an interesting and mind blowing experience. I had been conditioned to consider the first round as a test round and I never expected to fall pregnant. We ended up with four fertilised eggs and four embryos on the first day. I was really disheartened by that but I reminded myself that it was quality over quantity.
“I went on blood thinners – clexane – to prevent clotting. I did two intralipid infusions which are still quite controversial in the IVF world. Basically it’s a fat concoction that you have in a drip and it helps to nourish and thicken your endometrium and encourages implantation. I was also on progesterone.
“I never truly celebrated this pregnancy till I was 20weeks and it took till 28 weeks to be officially diagnosed with Hyperemesis Gravidarum (HG). I had scans every week with my OB who specialises in high risk pregnancies but it wasn’t until I felt him kick that I really settled into it. That said, I was dealing with constant nausea and vomiting and spent weeks in bed – resting and working and realising that it wasn’t going to abate, I just needed to get on with it.”
Keira took the same approach to her daily clexane injections which are renowned for being incredibly painful (a strong sting or burn). She admits that icing her skin and injecting into the love handle was more manageable than injecting into the belly. It was important for her to go off clexane 48 hours prior to birth to minimise the risks (including placental abruption) so she was booked in for an induction at 38+4. Baby Hunter had other ideas.
“I did acupuncture on Saturday (I’d been doing it all through my endo pain and IVF) and my acupuncturist was showing my partner, Anthony some acupressure points. On Sunday I lost my mucus plug and I was a bit crampy but I thought it was just acupuncture doing its job. At 4am on Monday I had a gush of warm liquid and I thought I’d wet myself. I went to the bathroom and I felt more of a gush. I lay back down on the bed and there was just a massive gush and it was like a tap dripping.
“I was shaking and laughing and so in denial about what was happening. I called my OB, we then called the hospital and we live 1.5 hours from there so we really quickly packed our hospital bags. I was having three contractions every ten minutes and they were pretty intense. When we got to the hospital there were bright lights and covid screening tests and all of a sudden my contractions stopped which was really disappointing. I couldn’t have my doula because of Covid and the hospital was really busy so we couldn’t have a birthing suite with a bath. By 10am I was contracting mildly but my OB recommended an induction, knowing my history of PTSD from my past hospital experiences, he was concerned that my labour would stall completely.
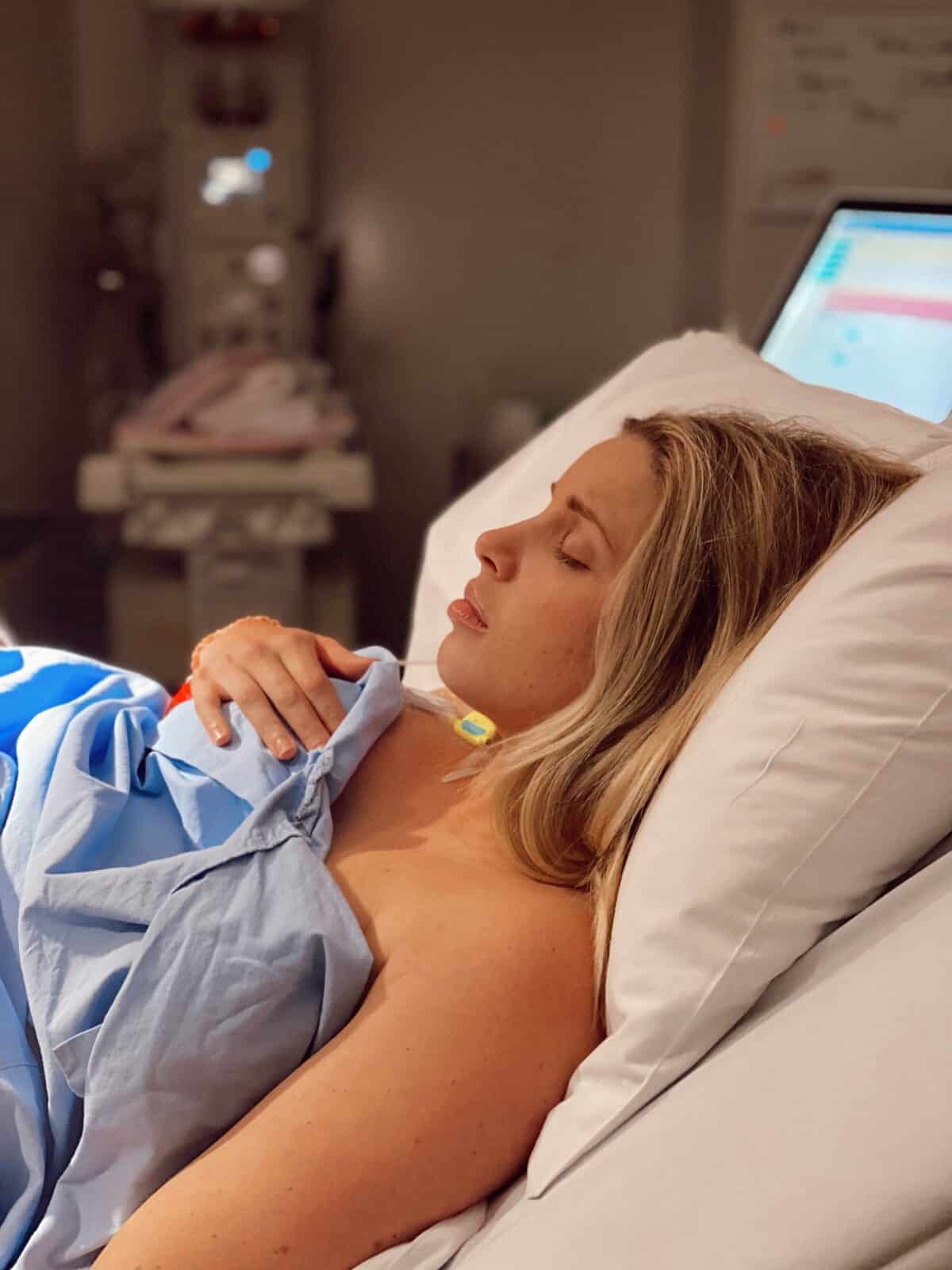
“When they turned the syntocinon up for the second time it became so intense; back to back contractions with no rest. It was really hard to focus my awareness on breathing but I used the gas for a few hours. I was only 3cm and it had been hours and I was so defeated. It was another few hours till I just looked at Anthony and told him I needed the epidural. I remember the relief of his face, that I’d finally surrendered. It was the longest five minutes of my life waiting for the anaesthetist. They did a really low dose of the epidural because I really wanted to feel a bit of the contractions so I knew how to push. The relief was amazing and within 20 minutes I went from 3 to 8cm just because I’d relaxed. I’d done a lot of research on epidurals and there was a lot of evidence to suggest that they can help your body relax and it definitely worked for me.
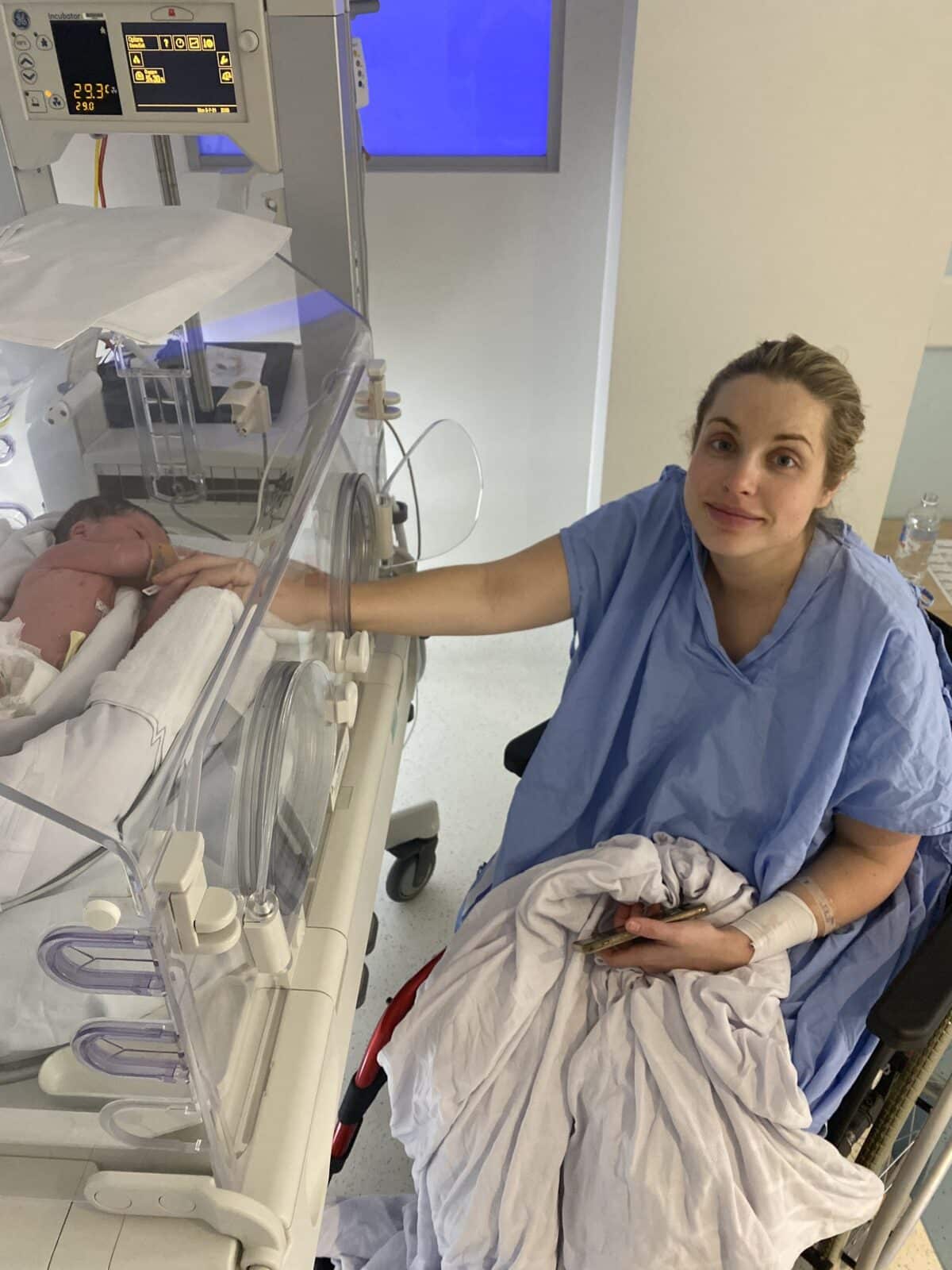
“I was actively pushing for 30 minutes and Anthony was holding my legs and watching as my OB guided Hunter out. He had so much hair! It was such an intense feeling but I feel like it really helped me with my pushing. His little hand came out just before his head so my OB pushed him back in and then once he was born my OB and Anthony passed him to me and I brought him up to my chest. He was incredibly blue and he wasn’t making much noise so Anthony cut the cord straight away and he was on the resuscitation table for 10 minutes. He wasn’t doing well at all. They brought him over with an oxygen mask and I got about 30 seconds of skin to skin before they took him to the NICU.
“He was over 3kg so he was a decent size but when they got him to NICU he was floppy and needed 100% oxygen and was unresponsive. I was so upset but I knew he needed to be there. He went down to 30% oxygen overnight but we couldn’t do skin-to-skin till 48hours after. It was really, really hard.
“A few days had passed and I was in the shower and Anthony asked me what I thought of our baby and I said Yeah, he’s cool but I’ve got no connection to him. I was so upset, saying that. I didn’t have that bonding time, I was petrified that it would stuff up our breastfeeding journey. I’m 100% connected now, now that we’re home.
“I told the midwife that I needed a plan and she told me he would probably have issues with sucking. But I just knew that he was a strong baby and I expressed some colostrum onto my finger and put my finger in his mouth and he sucked like crazy. My whole body just relaxed when that happened.
“I was really stubborn and just demanded a plan of action. My focus was feeding him and he was doing so well and the midwives that saw him when he first came in just couldn’t believe it was the same baby. Two days after birth he was getting lots of skin and skin and feeding well. By Thursday afternoon the midwives told me he would be going home with me the next day.
“It was the most enlightening feeling; walking out of special care with my baby. It was really surreal. We got back to my room and we did skin on skin and he crawled down to my nipple and I just sobbed. I just thought this is what it’s meant to feel like.
“We got discharged on Friday morning and it was the weirdest feeling. We got home and my postpartum doula came over and helped me feed, she made me a chicken noodle soup. The first night was tough though…we were still formula feeding and I was expressing. But then I connected with a NICU midwife and lactation consultant and she taught us so many tricks and since then Hunter has been breastfeeding beautifully.”
You can now hear Keira’s second birth story with her daughter Goldie in episode 405

Topics Discussed
Endometriosis, Factor 5 leiden, Heterotopic pregnancy, HG, IVF, Miscarriage
Connect
You can connect with Keira at @KRUMBLE and learn more about her new range Habitual Beauty here.
Categories
Related Products
-
The Birth Class
108 reviews$249.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






