EPISODE 281
Emma

Emma had been on the pill since she was 17 so she went off it with the hope to regulate her cycle and get to know it in preparation for conception. “I planned to give myself six months to learn how my body worked and I saw a naturopath who guided my nutrition and helped my partner and I eat really well. My GP also did blood tests and noticed that my Vitamin D levels were low so I went on supplements for that. She was really thorough with everything and had all bases covered, she even checked that my immunity had lapsed on a few of my vaccinations so I had the boosters before I conceived.”
“We fell pregnant the first month we tried which was a bit of a shock but a lovely surprise.
I’m Aboriginal and at the Royal Women’s Hospital in Brisbane they have a midwifery group practice called the Ngarrama midwives; there are a team of three midwives and they are with you throughout pregnancy and one of them will support you at birth and then they visit you at home during postpartum. They also have a physio and a dietician who you can chat to; it’s such a great program and covers all the bases. I’ll have my six-week check-up with the physio soon to assess my pelvic floor and create a plan to move back into exercise safely.
“Before I conceived I knew my pelvic floor was tight and ‘switched on’ a lot of the time so prior to conception I saw a physio and she confirmed what I already knew; I was tight and holding on when I shouldn’t have been. We worked on relaxing, letting go and being aware; when I’m training I need it on but I need to be conscious of relaxing it when I wasn’t training. My GP and my midwives were supportive of my training; I had to make sure my core body temperature didn’t go above a certain point and if I was doing high intensity training I would monitor my heart rate and if it went up I’d just stop what I was doing. I felt confident with that approach.
I really wanted to have a waterbirth and I wanted a drug-free birth. As well as doing hypnobirth I did The Birth Class and one of the most important things I took from it, especially at the end, was Optimal Maternal Positioning. I was always very aware of my position to encourage Gracie into a good birth position and using breath and sound in labour. It was a big deal for me because my mum had two big babies and she had two emergency caesareans; I felt confident in my body but her experience, and the fact that genetics does come into play, was always in the back of my mind. That was a lingering fear for me.”
At 39 weeks Emma started getting light period-like pains while doing a workout one morning and while she thought it could have been something, she was also conscious of expending too much energy. The pains continued throughout the day and by 2pm they were about 15 minutes apart.
“During my pregnancy I had a diary that I updated regularly and I wrote in it that day. It was a nice time for me just to settle but I noticed that the pains fizzled out. At 5pm I went for a short walk around the block to get things moving and it worked. By 7pm I got in the shower and I admitted to my partner, Nick, that I thought it was actually happening, it wasn’t a drill.”
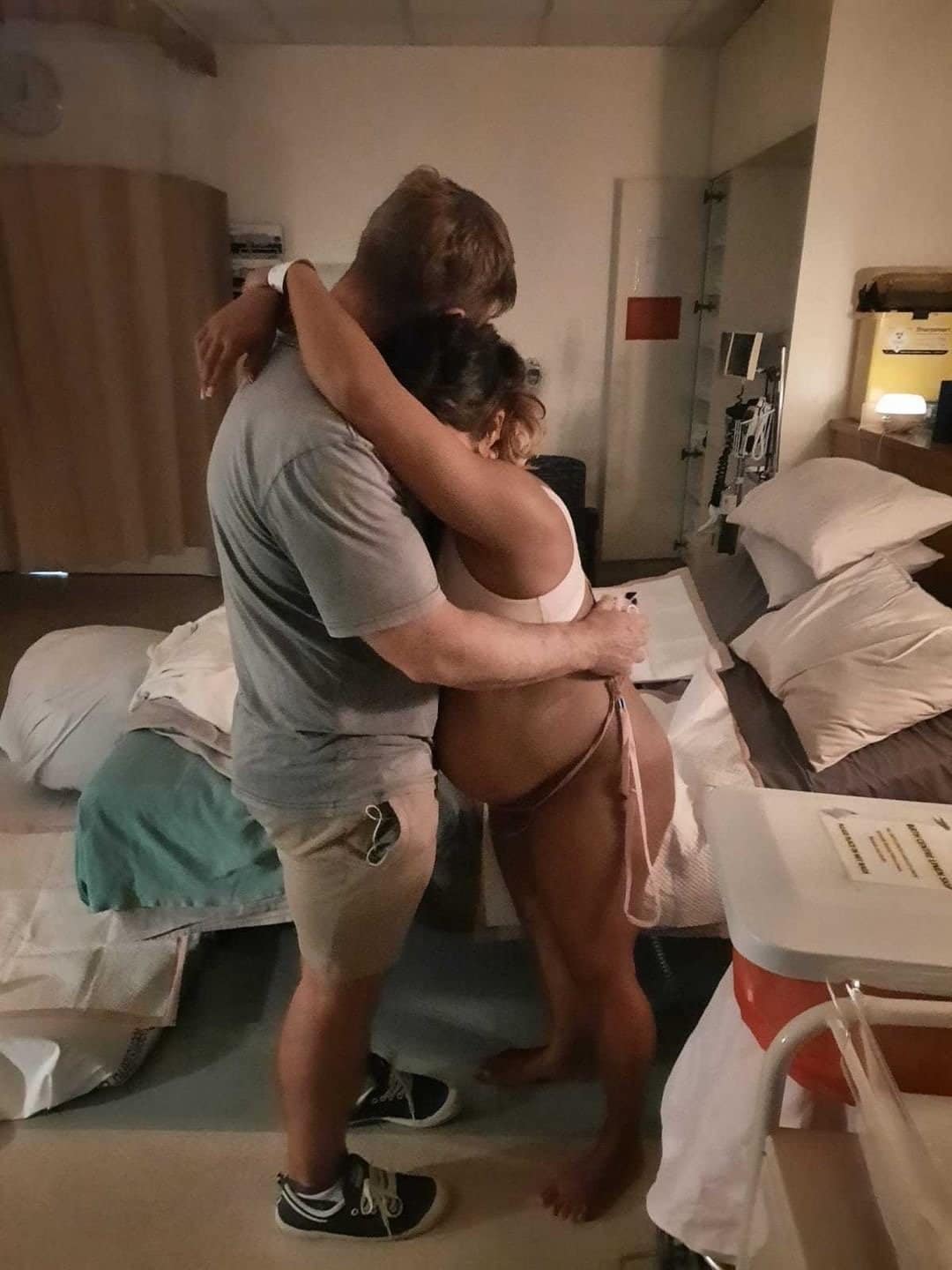
Emma laboured at home and by 10:30pm she felt like she was in her zone so Nick called the midwife who encouraged them to stay at home for a bit longer. When it was time for them to go to hospital, Emma made a point of requesting a water birth so her midwife called around the hospital to ensure a midwife trained in waterbirths could assist her birth. Emma spent the first two hours at the hospital in the shower (sitting on a fitball between contractions, standing up while she contracted) which helped Gracie’s position and encouraged her to move further down.
“The hardest part for me was not knowing how long I had to go and not knowing if I was progressing. I feel like I was already in transition or feeling the pushing reflex when I got in the bath. My pushing phase was only 18minutes so I didn’t use the water to its full extent because it was on, I was pushing. Nick sat on the edge of the bath with his feet in the water and I was on all fours leaning on his thighs. It was quite overwhelming, that shift to second stage, but it was so intense. Prior to getting in the bath I had been on the toilet because I felt like I needed to go but that was probably just bubby getting lower and lower. It was really good to feel something different. I was really feeling the fetal ejection reflex and when I had birthed her head my midwife told me that she was looking at her and she was so cute. I was waiting for the next contraction and that was the point where I thought: I am progressing! I pushed her body out and she was born behind me so the midwife caught her and passed her to me. She was crying straight away and it was just amazing.”
Emma had to get out of the bath quite quickly as the bath turned red immediately and her midwives wanted to investigate. She birthed her placenta five minutes later and Gracie stayed attached to her cord for then. While her perineum was intact, Emma had an internal tea, most likely caused by Gracie’s hand being beside her face during birth. After getting stitches, the little family of three snuggled on the double bed at the birth centre and messages their family and friends to announce Gracie’s arrival. They went home that afternoon. At 10 days post-birth, Emma developed mastitis; the first sign was flu-like symptoms which made her think she had covid. Once she had done a negative RAT test, she felt relieved but was also unsure what to do. Her temperature was 39.6 and her midwives encouraged her to go to the hospital where she stayed overnight and was put on IV antibiotics. She spoke to a lactation consultant who encouraged her to massage her breasts and express in the shower as well as feeding on demand. She’s been using nipple shields since Gracie was born but is hoping to phase them out.

Image by Jess Naera Creative

Image by Jess Naera Creative


Topics Discussed
Breastfeeding, Indigenous midwifery group practice, Mastitis, One vaginal birth, Pelvic floor, Physiological birth, Preconception health, Water Birth
Episode Sponsor
This episode of Australian Birth Stories was proudly brought to you by our friends at Bellamy’s Organic. With so many food choices, it is difficult to know what’s best. At Bellamy’s Organic, they only make certified organic, nutritious baby food. They believe that a meal is more than nourishment and that’s why they’re committed to introducing an early love of nutritious, wholesome organic food to children. Research shows that starting babies early on healthy foods early in development, helps foster healthy eating habits throughout life.
Their range of organic cereals, pastas, rusks, snacks and pouches help babies adapt to new flavours and textures and are approved by paediatric dietitians. With Bellamy’s Organic, you can be confident you are giving your little ones a pure start to life. Available in your local supermarket or pharmacy, or shop directly on the Bellamy’s Organic website. Use the code ABS20 for 20% off your next baby food order!
Categories
Related Products
-
Breastfeeding Guide
3 reviews$19.95A guide to inspire pregnant women to prepare for their breastfeeding journey.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us






