Podcasts Johanna Nicholson
EPISODE 200
Johanna Nicholson

Jo admits that she started off feeling very relaxed about falling but after a year without success she decided to see her GP who encouraged her to have a series of tests and scans. Everything came back normal; she was ovulating regularly, her hormone levels were normal and her basal temperature reading didn’t show any unusual signs. Encouraged by the results, Jo and James continued for another year before they sought the advice of a fertility specialist.
“She told us to keep trying but looking back I think we probably should have started to make some serious decisions then. It was in the third year we went back to our GP and we got a referral to do ovulating tracking which involved lots of blood tests over a three-month period. From there we decided to do IVF.”
Even though her inability to conceive didn’t consume her, it was always in the back of her mind. Jo administered the injections herself and admits to feeling a bit like a pincushion after all her recent tests. After the first round she had Ovarian Hyperstimulation Syndrome and she had to wait two months for her hormones to normalise so they could do the transfer.
“I got 30 eggs but they weren’t all usable. Thankfully we got two embryos from that cycle. Even though I was told not to do an at-home test I did about 5000 so when it was time to do the blood test I knew that we were pregnant. I went a long to the 7 week scan with James and we saw the tiny heartbeat. It was measuring a few days small but knowing that didn’t raise any alarm bells for me at the time. They wanted to do a follow up scan the next week and at that scan there wasn’t a heartbeat. I was alone and I just remember this long silence.
“I went into the hospital to have another scan to confirm the miscarriage and they gave me the otpion to wait to see if things would happen naturally or whether I wanted a d+c. I decided to wait for things to happen naturally although I really didn’t know what that involved and James and I were due to go on a roadtrip to a friend’s farm in South Australia.”
Jo and James were on the road in country NSW when she started to pass their baby and she felt incredibly unprepared for the pain of it.
“It was a more significant experience than what I expected. There was a lot of pain, a lot of bleeding, so much pain that I was vomiting. We felt like we needed to name the baby…we felt connected and that we needed to honour them in some way. We called them Blueberry because that’s the size of them when they passed.”
Jo decided to wait for a couple of months before transferring the second embryo. She was genuinely surprised when the test came back positive and although she was nervous throughout the first trimester, she enjoyed a very smooth and joyful pregnancy. She did a free birth course online during the height of Covid and listening to Australian Birth Stories regularly.
A week before her due date her Obstetrician booked her in for an induction which she thought was a bit premature. Each day passed and nothing happened and she found she was getting really fixated on the induction date as so much of what she had read and heard encouraged spontaneous labour.
“I felt really conflicted about the decision to be induced, it felt strange to have the power to make that decision. It felt really weighty and after talking it over with James we decided to go ahead with the doctor’s advice and we went to hospital that evening to start the induction process.
They monitored Henry for half-an-hour and it showed some very small dips in Henry’s heart rate so the midwives were watching it like hawks. They were concerned about these small dips, especially considering I wasn’t yet contracting, so they left the monitors on for a few hours and the doctor was called in from home. He broke my waters and headed home for the night, expecting to see me the next morning.
“The midwife all of a sudden asked James to go out and ask another midwife to come in and all of a sudden these people started rushing in. I started to shake and couldn’t control it, I think it was partly adrenaline and stress. Henry’s heart rate had gone down to 50 during the very first, very mild cramp. They gave me an injection that would slow down the contractions and the doctor came back in and said that we really needed to deliver the baby and do an urgent cesarean.
“I was asking all these questions on the way to theatre and they gave me an epidural so I could stay awake during the cesarean. I was so determined to have a natural birth and that’s where all my research was focussed. I couldn’t believe how quick the cesarean was, I just had no idea.
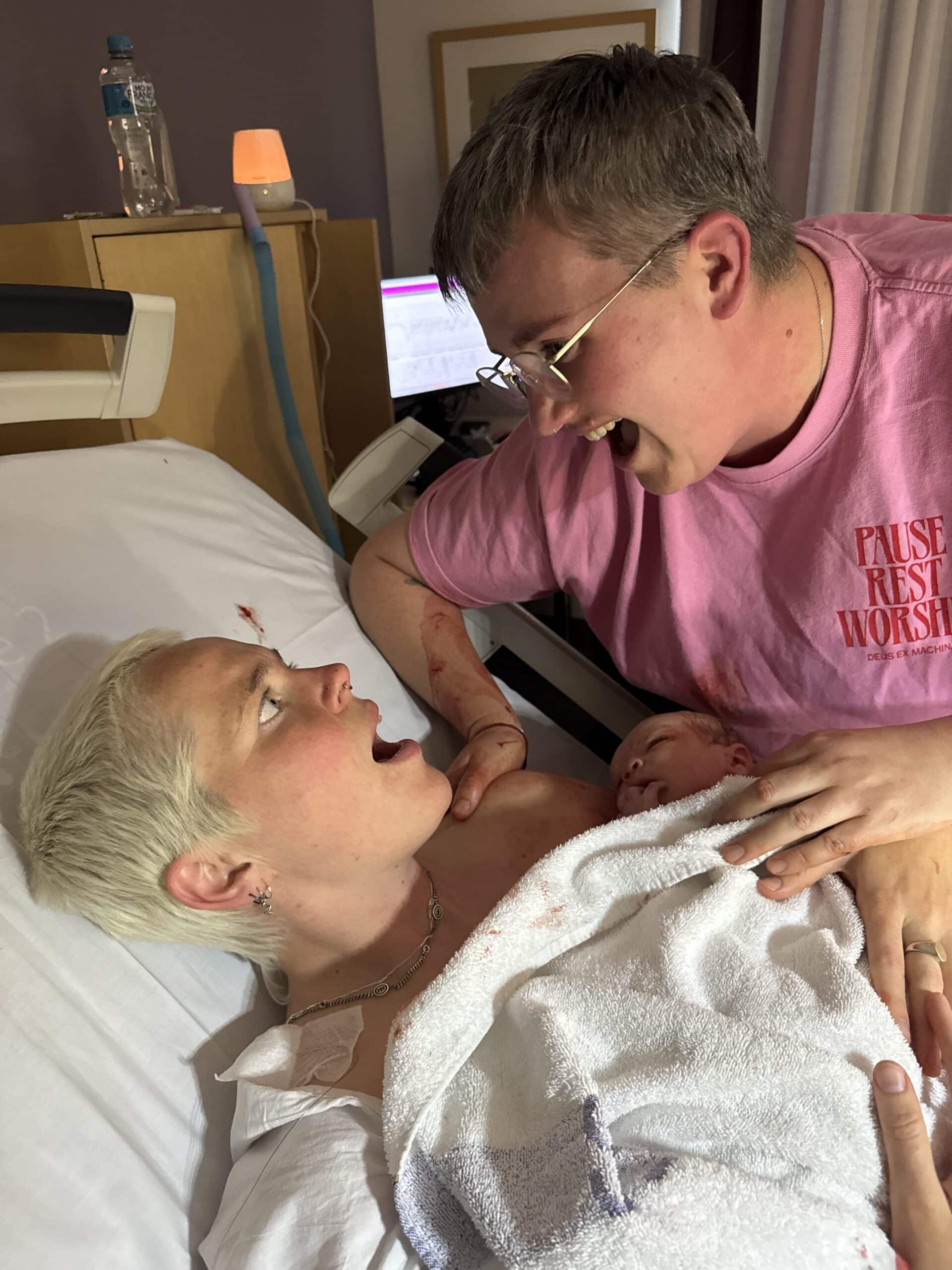
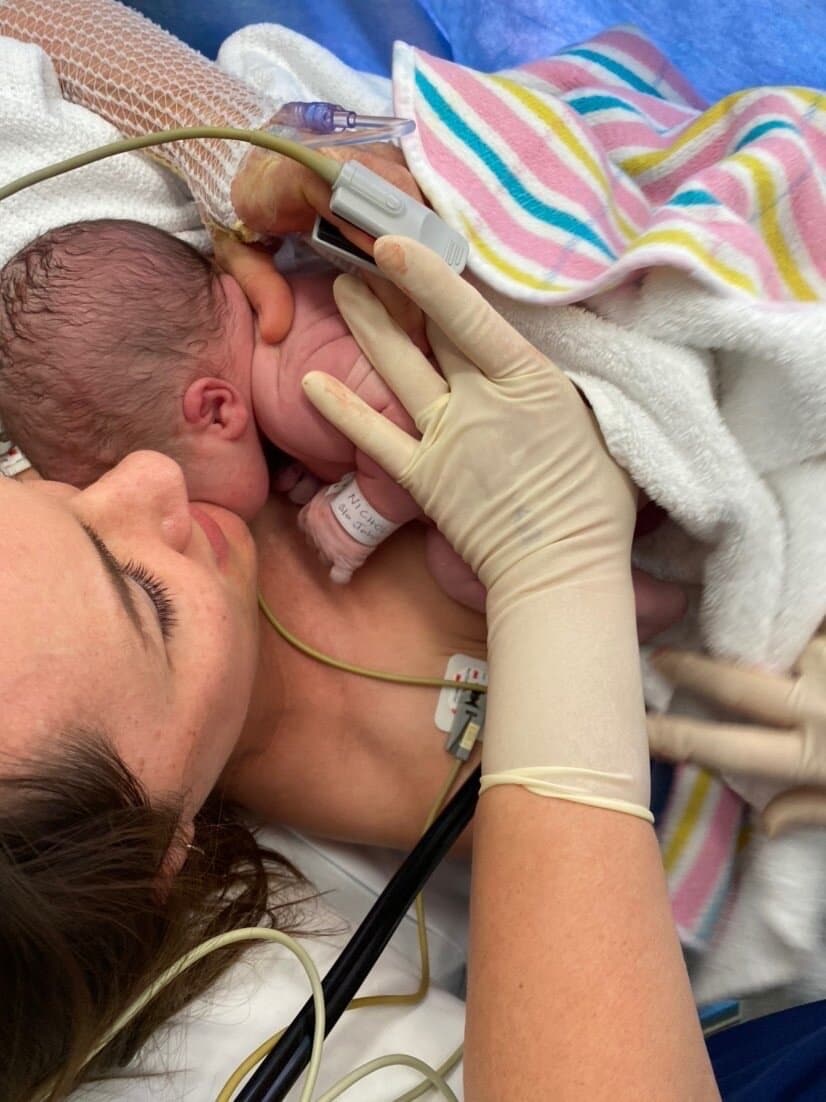
The tugging was strange; intense without pain. It was only 10 minutes and Henry was born. He was crying which was great and taken to the table to be checked but was back on my chest while I was being stitched up. We just looked at each other and I introduced myself to him and it was so nice but they didn’t have enough staff to keep him with me in recovery so I spent 45minutes there alone.
“Once I was back in the room James just burst into tears. He said he’d been quite robotic throughout the whole experience but then he was left in the room by himself with our newborn and he thought I was ok but he still wasn’t sure. He was just so relieved to see me.”
Jo had spent a lot of time researching breastfeeding while pregnant and had expressed colostrum in her third trimester, too. She was so buoyed when Henry latched straight away and although the first few weeks of feeding weren’t without challenges and pain, she was grateful for the expressed colostrum that she used for a topup, particularly in the first few weeks. Whilst she had the guidance of the midwives during her hospital stay, she found that she needed further support when home. The lactation consultants at her local community health centre have been a brilliant support and now, six weeks postpartum, Jo really feels like she has a great breastfeeding rhythm.
She admits that she’s so grateful for her birth experience but she can’t help but wonder what would have happened if she had denied the induction and laboured at home. “I feel like Henry was being protected and I know our entire church community was praying for him.”


Topics Discussed
Caesarean delivery, IVF journey, Unexplained infertility
Episode Sponsor
This episode is brought to you by The Birth Class, my online childbirth education course.
Featuring 10 audio lessons with perinatal health specialists, you can listen from the comfort of your home when you’re relaxed and receptive to new information. The Birth Class is a conversation starter between you and your birth partner that informs, encourages and empowers you to journey towards labour with knowledge and confidence.
In The Birth Class you’ll be guided through every stage of labour and birth, including:
– the powerful role of your hormones to prompt contractions and moderate pain
– what to expect from each stage of labour; from the first contraction to birthing your baby and the placenta
– practical breathing and sound skills to help you navigate contractions and overwhelm
– the benefit of staying active in labour and how it can assist cervical dilation
– how optimal maternal positioning in late pregnancy can encourage your baby into an ideal birth position
– how to prepare for a successful vaginal birth after caesarean (VBAC)
– your pain-relief options, both non-pharmacological and pharmacological
– the risks and benefits of birth interventions and how they can help or hinder labour
– typical complications that lead to an emergency caesarean and what’s involved in the process
– what to expect in the hours after birth, including breastfeeding and blood loss
– breastfeeding advice to guide you through the fourth trimester with confidence.
– and so much more.
Learn more about The Birth Class here.
Categories
Related Products
-
The Birth Class
108 reviews$249.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us