Podcasts Tahlia’s Journey: From Heart Surgery to NICU Mum – A Story of Resilience and Hope
EPISODE 604
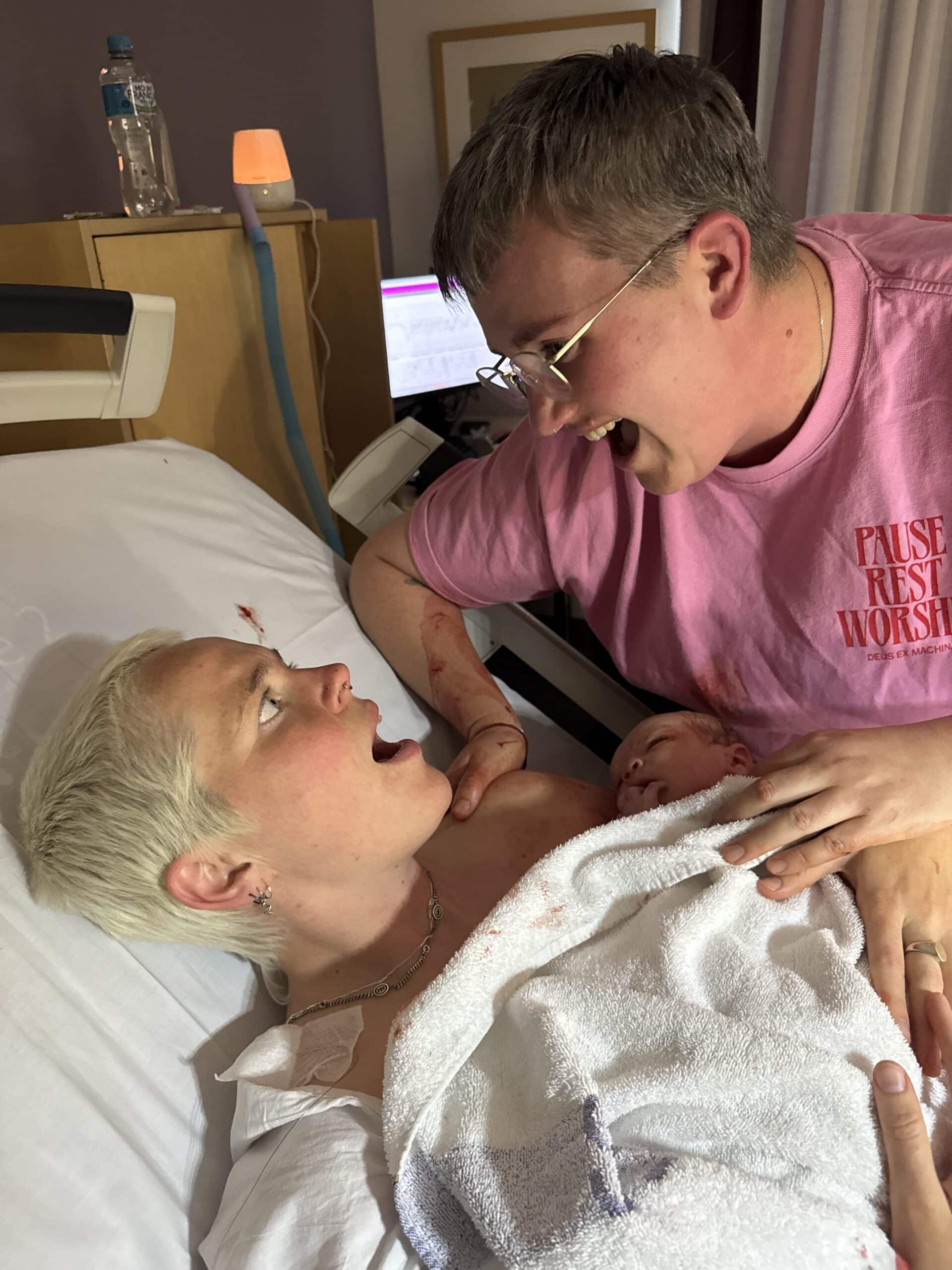
Tahlia’s Journey: From Heart Surgery to NICU Mum – A Story of Resilience and Hope

Tahlia’s story begins at birth, when she was diagnosed with a complex congenital heart condition. “The left side of my heart didn’t develop. So I only technically now have the right side. So one pump and one chamber,” she explains. Over her lifetime, she’s undergone three open heart surgeries, with the most recent being a pacemaker insertion in 2021.
As a mother herself now, Tahlia reflects on what her own mother endured: “I actually have no idea how my mum did it. I was also the second born. So with me being in hospital and needing all these surgeries, mum was juggling a toddler at home as well.”
The Fertility Journey: Timing and Heart Health
The conversation about pregnancy began when Tahlia was 25. Her cardiologist’s advice was clear: “If you are thinking about children, sooner rather than later.” The reasoning was sobering – as Tahlia explains, “The way that he would describe my heart as a muscle and how hard it has had to work to get to where I was, muscles age quicker if you overwork them.”
Despite this medical advice, Tahlia and her partner Maxie weren’t ready for children at 25. It wasn’t until COVID lockdowns that they seriously considered starting a family. After her pacemaker surgery in 2021, they began trying naturally for about 12 months before turning to IVF. Remarkably, “IVF actually happened. It took on the first transfer, which was, I know a miracle in the world of IVF.”
High-Risk Pregnancy Management
From the moment of her positive pregnancy test, Tahlia was under specialist care. “I was on certain kind of blood thinners that actually weren’t safe during pregnancy. So it was seize those medications, switch onto something else,” she recalls.
Her care team was extensive: “Emails were sent copying in the head of obstetrics. I got allocated a wonderful high risk midwife who was my point of contact throughout our whole experience.” The monitoring was intensive – fortnightly ultrasounds from six weeks, focusing particularly on placental development and blood flow.
Facing Difficult Conversations
At 11 weeks, during a foetal heart ultrasound, Tahlia encountered an unexpected and devastating conversation. The specialist asked: “Have you considered all your options? Because one of the options may be termination. If this path isn’t what you want because of the risks.”
Tahlia describes the impact: “We hadn’t even thought about that. And it was kind of a heavy conversation to then leave. And we were like, why would we consider that? And what are the risks and everything? And it just sort of escalated things a little bit more.”
NICU Preparation and Reality
At 21 weeks, Tahlia met with the head of neonatal care, learning about the realities of premature birth. The conversation included sobering statistics: “Generally around 24, 25 weeks, most babies tend to be over the 500 gram mark. And it was sort of a protocol within RPA that they, anything under 500 grams is do not resuscitate.”
The tour of the NICU was confronting: “I was quite emotional walking through there, seeing these tiny little babies and all these tubes and in their little fish tanks. And they just, that was really, really confronting.”
The Birth: 30 Weeks and 817 Grams
At 29 and a half weeks, during a routine ultrasound, Tahlia was told she wouldn’t be going home. After steroid injections to help Sunny’s lung development, she had a planned caesarean at exactly 30 weeks.
The theatre was crowded with specialists: “There was honestly probably about 30 people in the room. I had cardiology or like a team from cardiology there for any risk of anything happening to me. I had midwives in their obstetrics team that were delivering the baby. And then I had a team sort of over in the corner waiting from neonatal.”
Sunny’s arrival was promising: “I heard her cry, which was phenomenal because at 800 grams to cry means she was able to inflate her own lungs.” At 817 grams, she was tiny but strong.
The Hardest Day: Separation
The most challenging aspect wasn’t the surgery or the medical complications – it was the separation. “I actually wasn’t able to be taken down to meet her or see her until almost midnight that night. So that was probably the hardest thing I’ve ever done.”
Technology became a lifeline: “My husband was down there with her and then he FaceTimed me from there and I actually screen recorded it. And you know, he’s holding the camera and he’s like, there she is.”
Finding Purpose Through Pumping
Expressing breast milk became Tahlia’s way of connecting with and caring for Sunny. “Every time I managed to get a meal and then it would grow to two milth room, it was a celebration and it was a press the button, call the nurse, look what I got.”
The emotional significance was profound: “It felt like the biggest achievement and the most wonderful thing that I could do for her because there was nothing else that physically, I felt that I could even do for her.”
The Emotional Toll
Day three brought the full emotional impact: “I was hit really hard with those day three tears and the emotions and bore my eyes out all day.” Tahlia describes grieving “10 weeks of pregnancy that I didn’t get” and feeling overwhelming guilt: “I’m so sorry. I couldn’t do more for you. It’s because of you that you’re me that you’re this little.”
NICU Life: Becoming Part of the Team
Over 78 days, Tahlia and Maxie became integrated into the NICU routine: “They include you in a lot of the cares that they do for your baby and they encourage a lot of hands-on with that as well. So we would come in, you know, in our visits, we’d be there from morning to night and you would do the cares.”
The NICU became a community: “The nurses become a part of your family as well” and “you become very observant of the nicknames they even give like the equipment.”
Equipment That Makes a Difference
Throughout their stay, Tahlia noticed the donation plaques on equipment: “You can actually see they’ve got little plaques on them as to where they’ve been donated from. And for us, a lot of the equipment that we used with Sunny or they had with her was donated by the Humpty Dumpty Foundation.”
The breast pumps, in particular, were crucial: “The breast pumps became your little sidekick and I made friends with the other mums that are around me as well.”
Going Home: 78 Days Later
After 11 weeks in NICU, including a final “stay-in” night at the hospital, Sunny was ready to come home. “That moment when you get to honestly wheel your baby to the doors of the hospital and put her in the car was the best day of my life.”
The transition was surprisingly smooth: “We were ready. We were excited. We were like, if anything, we’re more equipped. We’ve been doing this already.” Sunny’s NICU routine actually helped: “She’s used to third hourly feeds. She’s like bit of clockwork.”
Life Now and Looking Forward
At 18 months old (born at 30 weeks), Sunny is thriving. Tahlia reflects on the experience with gratitude whilst acknowledging the ongoing considerations for future pregnancies: “There’s a lot of other things to consider and I do know that this is probably going to have to have, I’m going to have to have a conversation with my cardiologist who will probably be like, oh my God. What do you mean? You want to do it all again?”
Supporting Other Families
Tahlia’s experience has led her to support the Humpty Dumpty Foundation’s Mother’s Day campaign, raising funds for hospital-grade breast pumps. “There’s actually a few hospitals that believe it or not only have one pump to cater for the maternity ward, the neonatal, special care. So it’s really important, I feel from my experience that the hospitals have these equipments for women.”
This episode beautifully illustrates the resilience of both mothers and babies, the importance of specialist equipment in neonatal care, and how expressing breast milk can provide crucial connection during the most challenging of circumstances. Tahlia’s story will resonate with anyone who has faced a high-risk pregnancy, spent time in NICU, or simply needs reminding of the incredible strength that mothers possess.
To support the Humpty Dumpty Foundation’s breast pump campaign, visit www.humpd.org.au
Topics Discussed
Caesarean, IVF
Episode Sponsor
iL Tutto has just launched its beautiful new Trend Collection in Mocha.
The iconic Frankie and Louie Electric Recliners are now available in warm Teddy-Fleece and Corduroy fabrics, designed to support feeding, settling and those quiet moments of early parenthood, while still looking beautiful in your home.
To complement the chairs, iL Tutto has also introduced Walnut Sustainable Timber nursery furniture, including their Luca and Ollie cots with the matching Theo chest.
To celebrate the launch, they’ve created two complete nursery sets combining their recliners, cots and chest of drawers, making it easy to create a nursery that blends comfort, design and longevity.
And for a limited time, you can enjoy 20% off the Trend Collection and the rest of iL Tutto’s range of Nursing Chairs, Cots, Chests and CoZee Co-Sleepers, plus many more Nursery essentials. Simply use the code ABS20 at iltutto.com.au.
iL Tutto, designed for comfort, made to last.
Categories
Related Products
-
The Caesarean Birth Class
4 reviews$198.00The empowering online childbirth education program that will help you confidently prepare for birth.
Join the conversation
Sign up to get the latest updates, freebies, podcast releases straight into your inbox
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us
@AustralianBirthStories
Follow along with us